Clinical context and recognize the imaging findings of PML
Progressive multifocal leukoencephalopathy (PML) is a rare but sever viral subacute progressive demyelinating disease of the central nervous system (CNS) caused by the polyomavirus JC (JCV) infecting oligodendrocytes.
Primary PML developing in an immunocompetent patient is very rare.
It occurs almost exclusively in immunosuppressed individuals.
Is seen in clinical contexts such as severe combined immunodeficiency (SCID),
leukemia,
lymphoma,
systemic lupus erythematosus,
and organ transplantation) but more frequently occurs in AIDS than in other immunosuppressive conditions (typically seen when CD4 cell count drops below 50/μL).
Some AIDS patients may develop PML during combined antiretroviral therapy or worsens pre-existing PML in the setting of immune reconstitution.
Patients treated with Natalizumab (a humanized monoclonal antibody against the cell adhesion molecule α4-integrin and is used in the treatment of multiple sclerosis and Crohn's disease) is the second largest group of patients associated with a risk of PML.
The symptoms associated with PML include visual deficits,
cognitive impairment,
motor weakness,
gait disturbance,
dysarthria,
dysphasia and seizure and reflect the location of pathologic brain lesions (typically spares the optic nerve and the spinal cord).
Definitive diagnosis of PML requires neuropathologic demonstration along with the techniques to demonstrate the presence of JC virus.
The presence of characteristic clinical and neuroradiologic imaging manifestations with exclusion of other disorders (like other opportunistic infections) with the demonstration of JC virus in CSF is also considered diagnostic.
The extent of disease can be seen on CT but should be determined by lesion load on MRI scan of the brain due to the higher sensitivity of the technique to the presence of the white matter lesions.
The lesions of PML may occur all over in the brain and can be monofocal but they are usually multifocal.
Is important distinguishing white matter lesions of PML from other diseases that may affect the white matter in a similar manner,
including AIDS dementia.
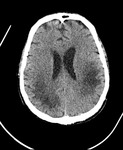
CT of the brain in PML expose hypodense bilateral asymmetric focal lesions of the affected periventricular and subcortical white matter and thalamus with mild or no mass effect and rarely contrast enhance (5%–10% of cases) Fig. 1 .
- Subcortical frontal and parietooccipital white matter are typically involved regions.
- Basal ganglia,
brain stem and cerebellum also can be affected usually secondary to extension from lesions of adjacent white matter.
- In late stages of disease grey matter involvement has also has been reported.
- A “scalloped” appearance underneath the cortex is described when there is involvement of the subcortical arcuate fibers.
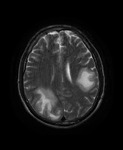
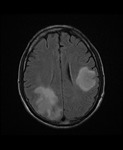
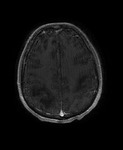
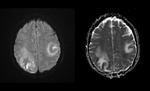
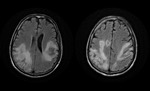
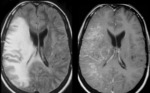
MRI shows hyperintense lesions with “ground glass” appearance on T2-weighted images and fluid-attenuated inversion recovery (FLAIR) images in the affected regions with mild or no mass effect and rarely gadolinium enhancement (15% of cases) Fig. 2 Fig. 3 Fig. 4 .
On T1-weighted images,
these lesions are hypointense.
On diffusion-weighted imaging (DWI) there is no diffusion restriction centrally but only peripherally at the active site of lesion expansion with cytotoxic edema Fig. 5 .
These lesions may be mistaken for an acute cerebrovascular insult.
Magnetic resonance spectroscopy reveals a decrease in N-acetylaspartate and creatine and increased choline products,
myo-inositol,
and lactate in the lesions of PML.
With the institution of highly active antiretroviral therapy HAART,
the prognosis for HIV-associated PML has been shown to improve however no effective therapy that directly targets the JC virus has been developed.
Clinical context and recognize the imaging findings of IRIS
IRIS is defined as a paradoxical clinical worsening of a known condition or the appearance of a new condition after initiating antiretroviral therapy in HIV-infected patients usually in the setting of low CD4 count/high viral load.
Forced immune reconstitution can lead to massive destruction of virus-infected cells.
IRIS is the result an exaggerated inflammatory response to an antigen of a dead or dying organism of an opportunistic infection.
It has been described in patients with various AIDS related illnesses,
including PML with an overall incidence between18%-50%.
It develops within weeks,
months (usually occurring within 1–2 months),
or,
rarely,
years after the initiation of HAART.
It must be considered in the context of new or progressive clinical symptoms and the appearance on CT and MRI studies the presence of neuroimaging abnormalities that are not classic for untreated PML,
despite medical therapy and despite improved laboratory data (evidence that the patient's immune system is reconstituting: higher CD4 counts and decreasing HIV-1 RNA levels).
PML-IRIS is characterized by the development of contrast enhancement of the PML lesions,
but in only 56% of patients,
(seen as contrast T1WI parenchymal and perivascular nodular enhancement),
mass effect due to interstitial edema (marked increased high FLAIR/T2 signal) and restricted diffusion Fig. 6 Fig. 7.
Even though IRIS in the setting of HIV infection is a diagnosis of exclusion,
the neuroradiologist has an important job in informing the clinician to the possibility of this syndrome.
This condition is usually self-limiting (resolve with continued HAART) but it can be also quickly fulminating or may lead to significant morbidity.