Examination technique
Patient
- the patient is usually examined in a supine position,
but the other positions may be used depending on the clinical situation
- there are several scanning methods described in literature,
but maybe the most known and most used is the 3 points examination of each lung as it is fast and produces accurate results
Probes and frequency
- any transducer may be used to visualize the lung
- liner probes (7-12 MHZ) are great for the visualisation of superficial structures such as the pleura,
as their resolution is excelent,
providing important details
- curviliniar probes (3-5 MHz) on the other hand are useful for the assessment of larger lesions and fluid collections.
Normal US appearance of lung an pleura
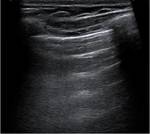
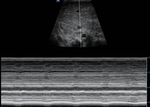
A lines
The air below the pleura will reflect most of the sound waves generated by the transducer causing some of them to go back and forth between the pleural and the probe.
This will cause artifacts called A lines.
A lines are horizontal lines,
parallel with the plane of the probe,
located below the pleura,
with the same distance between them as between the transducer and the pleura.
(Fig.
1)
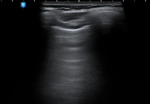
Lung sliding
Normally the parietal and visceral pleura are slightly opposed due to the presence of a minimum amount of fluid between them which causes them to slide one over the other.
On US this appears as back and forth movements of the pleura.
(Fig.
2)
Pathological findings
Lung US easily distinguishes between parenchymal consolidation and fluid collections and allows for the characterization of pleural effusions regardless of their volume,
appearance and content.
US is a great method to visualize even the smallest quantities of pleural effusion,
semi-quantify the volume of the effusions and detect complications such as empyema.
The folowing cases will demonstrate the US appearance of various types of pleural effusions depending on their quantity,
etiology and content.
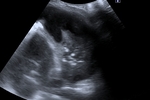
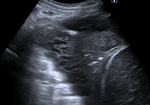
Consolidation - are characterized by high fluid content,
and most of them reach the pleural line and therefore become visible on US.
When the lung tissue is fluid filled its US appearance is similar to that of the liver (hepatization).
Within the consolidation area air bronchograms will be seen (echoic lines) and fluid bronchograms (hypoechoic).
When visualized in the long view they appear linear and if in transverse view will appear punctiforme.
This aspect is typical for consolidation.
(Fig.
3)
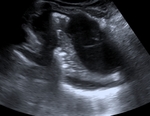
Fluid collections
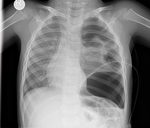
Small quantities of fluid may be missed on a chest radiograph,
while US is superior in detecting pleural effusions,
its sensitivity and specificity being close to 100%.
Effusions are gravity-dependent so they will be better visualized and evaluated caudally and posteriourly,
between the lung and the diafragm.
Pleural fluid effusions may be anechoic,
hypoechoic,
with internal septations or echoic,
depending on its etiology and content.
US will easily distinguish between consolidation and collection or diagnose a parapneumonic effusion (Fig.
3).
It is easier to use US for follow-up in these patients and avoid unnecessary radiation exposure.
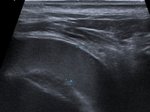
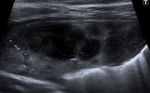
US may also help differentiate a simple fluid collection from a complicated one,
the visualization of internal septations helping to distinguish between transudate and exudate (Fig.
4).
In the case of an anechoic effusion it may not make a difference,
as it may be a transudate,
an exudate or an acute hemothorax.
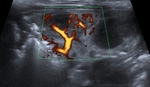
But an echoic collection,
with homogenenous internal echoes,
may be an exudate or subacute hemothorax (Fig.
5,
6,
7).
A pleural effusion with fine or thick septations inside is an exudate and is coused by infection and inflammation (Fig.
4,
5,
6).
Of course interpretations of these findings will be done in the clinical context.
The information provided by US are extremely important as they influence decisions regarding the course of the treatment (antibiotherapy,
thoracocentesis,
surgery).
One must be aware that there are fluid lesions inside the lung parenchyma (abscess,
necrosis) and that they have to be considered in the differential.
(Fig.
8,
9).
Another use of US is in the diagnosis of pneumothorax.
One way to do it is by using the M mode and the signs are represented by the barcode or stratosphere sign that appears on the M mode.
(Fig.
10,
11) This US application may extremely useful in emergency or intensive care units.