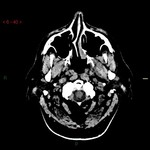
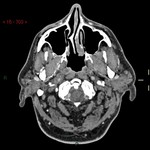
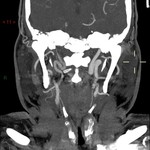
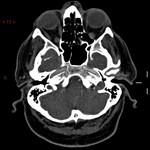
Traumatic neurovascular injuries are rare (0,1%-2% of severe trauma),
and are associated with high rates of morbidity (32%-67%) and mortality (17%-38%),
especially if not recognized and promptly treated.
Post traumatic dissections are the main cause of stroke in young people.
A good screening protocol can reduce injury-related strokes in patients without primary focal neurologic deficits.
(13)
PATHOPHYSIOLOGY
The central nervous system has a high sensitivity to the trauma,
and to neurovascular injuries,
that result in a diagnostic and therapeutic challenge.
Various parameters modification can break brain homeostasis inside the skull and lead to a permanent nervous tissue’s injury if not recognized.
Once a vascular injury is localized and identified,
the appropriate treatment may be initiated.
Treatment options depend on the need to strike a balance between the risks and the benefits,
upon the evaluation of the injury and the collateral circulation of the brain.
The crucial variable is the neurologic status of the patient.
It’s important to remember that many times there are concomitant post traumatic lesions,
sometime to be managed first.
Tab 1: Morbidity and mortality rate.
| Blunt vascular injuries |
Morbidity |
Mortality |
| ICA |
32-67% |
17-38% |
| VA |
14-24% |
8-18% |
Morbidity and mortality are therefore related to the extent of the trauma (Tab 1); for this reason,
selection criteria have been identified for applying patients to angiographic study.
(5)
Beyond the dynamics of the trauma,
it is important to consider the patients’ clinical condition (Glasgow coma scale GCS).
According to Wintermark,
traumatic neurovascular injuries should be suspected in patients with a high-velocity trauma,
low GCS,
high injury severity score,
and besides mandible fracture,
complex skull fractures,
(including carotid canal fractures),
scalp degloving,
any type of cervical spine injury,
and/or TBI with thoracic injuries,
and/or thoracic vascular imaging,
as well as in patients with penetrating neck injury (class I recommendation).
The absence of manifest clinical signs or symptoms of a clinically significant vascular injury does not mean that the injury is not present.
Based on Fogelman and Steenburg studies,
the frequencies of missed vascular injuries ranging from 23% to 43%.
Sometimes patient's neurological condition can be silent in the first hours.
Postraumatic neurovascular lesions are dynamic,
and especially the less severe (grade I-II of Denver) can evolve.
A follow up is needed,
so CTA/MRA are usually performed after 7-10 days.
MRI allows also to evaluate cerebral parenchyma.
CATEGORIES OF VASCULAR LESIONS
The types of endovascular lesions are two,
and are classified as "blunt" and "penetrating".
They can affect both the carotid and the vertebral arteries (18%-32% multivessel involvement),
with different incidence.
Vascular damage also affects the venous siystem,
and this occurs more frequently in penetrating traumas.
Crissey and Bernstein have identified four different mechanisms of blunt carotid injury,
related to the dynamic of the trauma.
Tab2 Internal carotid artery (ICA) injuries mechanism
|
Type
|
Mecanism
|
|
Type I
|
Direct blow to the neck
|
|
Type II
|
Hyperextension-contralateral rotation of the head and neck (most common)
|
|
Type III
|
Intraoral trauma
|
|
Type IV
|
Skull base fractures (sphenoid or petrous bones)
|
Regardless of the type of injury,
the mechanism is intimal destruction,
which exposes the thrombogenic subendothelial collagen surface,
resulting in platelet aggregation and distal embolization,
partial or complete thrombosis.
About vertebral artery injuries,
motion at the atlantoaxial joint,
cervical fractures,
and dislocations with bony impingements can lead to intimal and medial injuries.
The vascular lesions,
and resulting radiologic signs,
of penetrating traumas are generally similar,
but with a higher prevalence of arterial occlusion and transection because of the penetrating nature of the injury.
NEURORADIOLOGICAL CLASSIFICATION
The spectrum of imaging findings is wide.
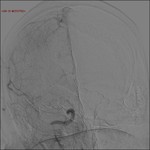
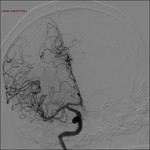
Digital subtraction angiography (DSA) is the gold standard in the detection of neurovascular lesion,
but it is not available in all hospital and it is an invasive procedure.
It can be performed,
when the patient is medically stable,
to establish a diagnosis and proceed with endovascular treatment,
if indicated.
Thanks to the DSA it is possible to evaluate at the same time the location of the injury and the collateral circulation of the brain,
to plan the best endovascular approach.
Retrospective studies and meta-analyses showed that multidetector CT angiography is a rapid,
noninvasive and accurate diagnostic technique for vascular injuries investigation.
CTA of the epiaortic vessels extended to include the circle of Willis has a sensitivity and specificity of almost 90%–100% for diagnosing vascular trauma in blunt vascular injury within the neck (evidence level II).
(12)
The Denver grading scale is a grading scheme,
composed of five entities,
graded according to angiographic appearance:
- Grade I: intimal irregularity <25% narrowing
- Grade II: dissection with intramural hematoma and 25% narrowing
- Grade III: pseudoaneurysm
- Grade IV: occlusion
- Grade V: transection with extravasation,
arteriovenous fistula (5)
The natural history and evolution of this lesions are different.
A prognostic correlation was determined between the grade of injury and the risk of postinjury stroke (12).
As showed in Tab 3,
the lack of linear increase of stroke risk with vertebral artery injuries may be due the presence of collateral vessels (protective facrtor).
Tab 3.
Grading scheme for blunt vascular injuries
|
Denver grading scale
|
DSA/CTA aspect
|
Risck of stroke ICA
|
Risck of stroke VA
|
|
I
|
intimal irregularity with < 25% narrowing
|
8%
|
/
|
|
II
|
dissection with intramural hematoma and >25% narrowing
|
14%
|
38%
|
|
III
|
pseudoaneurysm
|
26%
|
27%
|
|
IV
|
occlusion
|
50%
|
28%
|
|
V
|
transection with extravasation, artero-venous fistulas
|
Letal
Refractory to therapy
|
100%
|
MRA is a reliable alternative to CTA in vascular mapping,
(10) especially after injector-based contrast administration.
(1)
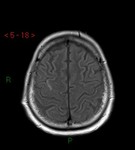
During a MRI-MRA exam are also performed axial fat-suppressed T1 weighted sequences,
that reveal intramural hematoma as hyperintensity around the vessel.
MRA identifies dissections in up to 99%.
(8)