Typical radiographic findings:
In plain radiographs the lesion is characterized by a small nidus surrounded by dense bone; the nidus is mostly seen as a radiolucent area significantly or mildly calcified depending on the disease duration (1).
At CT,
the nidus is well defined and round or oval with low attenuation.
An area of hypoattenuation may be seen centrally with a peripheral reactive sclerosis (3).
At MRI,
the nidus has low to intermediate signal intensity on T1-weighted images and variable signal intensity on T2-weighted images (2).
Radionuclide scans are helpful in identifying the lesion.
Osteoid osteoma can involve any bone of the skeletal system,
but is mostly reported in long bones of the lower extremity.
Atypical radiographic findings:
Osteoid osteoma is most common in the femur and tibia.
Uncommon locations are the spine,
hands,
or feet.
Very rare sites are the skull,
scapula,
ribs,
pelvis,
mandible and patella.
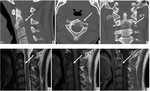
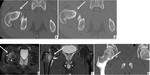
It’s difficult to diagnose spinal osteoid osteoma (Fig 1) on the basis of radiographic findings because of the complex¬ity of spinal anatomy and overlapping areas of soft tissue.
Spinal osteoid osteoma is usually localized in the neural arch and it’s usually associated with bone marrow edema in the involved pedicle and lamina that extends to the posterolateral vertebral body (2).
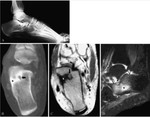
In the hands and feet,
cancellous osteoid os¬teoma occurs in the carpal and tarsal bones,
(Fig 3).
Carpal and tarsal osteoid osteoma may display less reactive sclerosis.
Because of the proximity of the bones in the hands and feet,
an inflamma¬tory reaction that originates from one carpal or tarsal lesion often spreads to adjacent bones and joints (4).
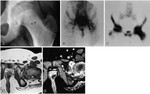
Intra-articular Osteoid Osteoma,
which occurs within or near a joint,
is uncommon,
accounting for approximately 12% of all osteoid osteomas and is considered a separate clinical entity.
Reactive cortical thickening is minimal or absent,
a finding believed to be due to a lack of cambium,
the inner layer of the periosteum.
The most commonly involved joint is the hip (5,
6)
The diagnosis of osteoid osteoma can be very challenging when clinical and radiological presentations are atypical.
This occurs especially when it’s accompanied by severe inflammatory changes such as a prominent peri-osteal reaction,
exaggerated synovial hypertrophy and joint effusion,
extensive bone marrow and soft-tissue edema.
Otherwise the dense sclerotic reaction is also can be absent or minimal.
When these confusing imaging findings are present the nidus is hard to identify and diagnosis is hard to be reach.
Conditions That Mimic Osteoid Osteoma:
• A stress fracture appears as an infraction in the center of an area of cortical thickening,
whereas osteoid osteoma appears as a round nidus (7).
Cross-sectional imag¬ing,
especially in the coronal and sagittal planes,
is useful for differentiating between the two conditions (8).
• At radiography,
an intracortical abscess and an osteoid osteoma often are indistinguishable.
At CT,
in osteoid osteoma,
the inner side of the nidus is smooth,
and a round calcifica¬tion is seen in the center of the nidus.
In an in¬tracortical abscess,
the inner margin is irregular,
and an irregularly shaped sequestrum is seen ec¬centrically (9).
• Intracortical hemangioma is an extremely uncommon primary bone tumor .
Histologically it consisted of a capillary,
arteriovenous,
or (more frequently) cavernous hemangioma located within the cortical bone without an adjacent soft-tissue mass (10) Radiographically,
intracortical hemangiomas demonstrate localized lytic lesion with or without cortical thickening and sclerosis with vertically aligned intralesional calcifications of the trabeculae.
At CT,
a hypoattenuating intracortical lesion with vascular channels and spotty internal calcifica¬tion,
or a so-called wire-netting appearance,
is seen.
• Chondroblastoma is a rare,
benign,
locally aggressive bone tumor that typically affects the epiphyses or apophyses of long bones.
Plain radiograph shows a characteristically lucent lesion and well-defined margins.
At CT,
Solid periosteal reaction,
internal calcification and cortical breach are appreciated.
When mineralized,
chondroblastoma demonstrates punctate calcification,
whereas osteoid osteoma displays a concentric pattern of mineralization (11,
12).
• Osteoblastoma is a rare primary neoplasm of bone,
categorized as a benign bone tumor that is closely related to osteoid osteoma.
It commonly affects the vertebral column,
with approximately 30% of these lesions arising within the posterior elements of the spine.
Pain does not respond to salicylates (13).
Moreover,
unlike osteoid osteoma,
osteoblastoma displays progressive growth and has malignant potential (14).
At imaging,
lesions are typically larger than 2 cm in size and have less reactive sclerosis surrounding the mass than osteoid osteoma (15).
• Compensatory hypertrophy of the pedicle may be mistaken for osteoid osteoma because spinal osteoid osteoma frequently occurs in the posterior neural arch and induces thicken¬ing and sclerosis of the pedicle.
Contralateral spondylolysis and lack of a typical nidus are indicative of compensatory hypertrophy of the pedicle (16).