Findings and proceduredetails
Before learning the radiologic findings for each kind of presentation of pulmonary aspergillosis,
we need to know some basics about them:
- Who do they affect?
- What does the fungus do?
- How is the clinical presentation?
Then we will focus on their appearance using MDCT,
trying to perform differential diagnosis with other entities.
1.SAPROPHYTIC INFECTION (MYCETOMA OR ASPERGILLOMA) Fig. 3
Saprophytic infection (with no tissue invasion) leads to formation of conglomerates of fungal hyphae,
mucus and celullar debris in the airways,
normally onto a preexisting pulmonary cavity:
- WHO: commonly immunocompetents with underlying causes such as tuberculosis,
that leads to formation of lung cavities.
Also people with pulmonary sequestration,
bronchogenic cysts,
pneumatoceles,
bullae…
- WHAT: the saprophytic infection of these cavities will lead to occupation by fungal spores/hyphae,
mucus and debris,
but with NO invasive behaviour.
- HOW: patients normally remain asymptomatic unless cavities grow; at these point,
clinical manifestations can be weight loss and hemoptysis.
This hemoptysis can be severe and may even require surgery or embolization.
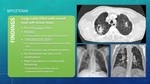
IMAGE FINDINGS Fig. 4
An aspergilloma consists in a pulmonary cavity filled with round/oval soft-tissue mass.
They tipically appear on the upper lobes and are usually MOBILE: content moves when patient changes position (from supine to prone scans).
Normally there’s air separation between mass and cavity wall; this is called the “AIR-CRESCENT SIGN”.
If not present,
it’s difficult to distinguish between aspergilloma and other soft-tissue solid masses,
such as neoplasms.
If present,
it’s also not specific: it might be seen in angioinvasive aspergillosis (indicates severity),
TBC with Rassmussen aneurysm,
pulmonary abscesses,
bronchogenic carcinoma,
hematoma…
Might associate thickening of cavity or pleural wall,
but this thickening is potentially reversible after treatment,
as it’s postulated to be an hypersensibility reaction.
Air-fluid levels and calcifications are rare.
Differential diagnosis includes hematomas,
neoplasms,
abscesses,
hydatid cysts…
2.
ALLERGIC BRONCHOPULMONARY ASPERGILLOSIS (ABPA) Fig. 5
ABPA is an hypersensitivity reaction to Aspergillus fungus by the organism.
- WHO: patients with chronic asthma.
Rarely as a complication of cystic fibrosis.
- WHAT: hypersensitivity reaction produced by inhalation of fungi.
- - Proliferation on the airways produces release of IgG and IgG
- - Immune complexes (Aspergillus + eosinophils) deposit on bronchial mucosa and produce necrosis and infiltrates in bronchial wall.
- -Bronchial wall damage leads to dilatation (bronchiectasis).
- HOW: mucus production leads to mucoid plugs and impaction in the airways,
which produces cough,
fever,
wheezing and can produce recurrent pneumonia if chronifies.
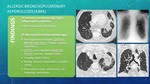
IMAGE FINDINGS Fig. 6 Fig. 7
The most important and common finding is presence of CENTRAL BRONCHIECTASIS that give the characteristic “finger in glove” appearance.
They tipically locate on the upper lobes.
Normally they associate bronchial wall thickening,
that,
in combination with mucoid plugs,
produce distal infiltrates that normally migrate.
This mucoid plugs may have high attenuation due to fungal hifae,
and may demonstrate calcification.
Chronic obstruction can lead to atelectasis,
air trapping,
cavitation and even fibrosis.
3.
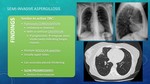
SEMI-INVASIVE ASPERGILLOSIS Fig. 8
Also known as chronic necrotizing aspergilosis,
it’s an infection affecting mild immunosuppresed patients in a more indolent way than invasive aspergillosis:
- WHO: Affected patients are those with mild immunosuppresion (chronic debilitating illnesses such as DM,
alcoholism,
malnutrition,
advanced age,
COPD…).
- WHAT: It’s a granulomatous reaction with tissue necrosis similar to that in TBC.
- HOW: the more important thing is CHRONICITY.
Symptoms develop over time,
and are usually non-specific (productive cough,
fever,
weight loss…).
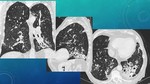
IMAGE FINDINGS Fig. 9 Fig. 10
Same as clinical symptoms,
imaging usually progresses slowly over time.
It mimics findings in active TBC and other granulomatous diseases,
such as unilateral or bilateral segmental consolidations that may cavitate.
If they do,
progression can be suspected when there are irregular intracavitary areas,
indicating the presence of fungal masses.
Usually predominance on upper lobes.
There may also be multiple centrolobular nodules of increased opacity.
4.
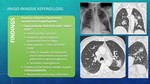
INVASIVE ASPERGILLOSIS Fig. 11
Invasive aspergillosis is the most severe form of pulmonary aspergillosis that occurs in severe immunosuppressed patients:
- WHO: neutropenic with <500 neutrophils due to AIDS,
post-transplant,
leukemia,
chemotherapy or corticosteroid for autoimmune diseases…
- WHAT: according to the site of invasion,
there are two types of diasase:
- - Airway invasion (20%): can show as bronchopneumonia (peribronchial consolidates with nodular opacities),
bronchiolitis (tree-in-bud pattern) or more rarely tracheobronchitis (irregular tracheal-bronchial wall thickening due to high-attenuation material).
- - Vessels (80%): the most common form is angioinvasive aspergillosis.
- HOW: non-specific ACUTE and RAPIDLY PROGRESSING symptoms (progressive,
dyspnea,
non-productive cough,
fever).
This allows distinction from semi-invasive form.
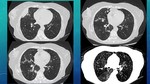
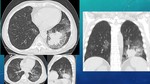
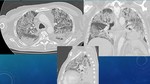
IMAGE FINDINGS Fig. 12 Fig. 13 Fig. 14
They are produced due to invasión from fungal hyphae into pulmonary vessels,
producing:
- FUNGAL THROMBOSIS: leads to centrolobular NODULES with “halo sign”,
with solid center representing necrosis and ground-glass periphery representing haemorrhage.
These nodules may cavitate after treatment (2-3 weeks),
giving the “air crescent sign” appearance; it’s a sign of treatment response and has to be differenciated from Aspergilloma.
They also appear in other conditions: haemorrhagic metastases,
Wegener granulomatosis,
herpes simplex,
candida,
Mucor…
- PULMONARY INFARCTION: leading to peripheral-subpleural wedge-shaped opacities.