The cases presented in this study were selected from our institution’s teaching filesat an University Hospital (Instituto de Medicina Integral Prof.
Fernando Figueira - IMIP) and show CT images of bezoars in the gastrointestinal tract.
INTRODUTION
The presence of bezoar in the gastrointestinal tract is rare and its true incidence is not known,
but they must be properly diagnosed and treated.
Bezoar consists of a compaction of exogenous material that can be found especially in the gastrointestinal tract1,2,3.
It corresponds to an accumulation of material that is not absorbed and digested,
forming an intraluminal mass that can produce several clinical manifestations4,5.
Bezoars are classified depending on their main composition.
Phytobezoars,
which account for almost half of all bezoar and are usually associated with foods containing high amounts of cellulose,
such as persimmons which is very difficult to dissolve or break up.
Another common type of bezoar is made of hair,
called trichobezoar associated with psychiatric pathology and trichophagia and frequently located in the stomach.
A particularly infrequent and complex condition is the Rapunzel's syndrome4,5 that occurs when the trichobezoar extends from the stomach through the small intestine.
Other kinds are pharmacobezoars,
lactobezoars and polibezoars.
Drug bezoars have been described in association with activated charcoal,
aluminum hydroxide,
sucralfate,
cholestyramine and nifedipine.
In its pathogenesis,
medications that alter gastrointestinal motility,
such as opioids and neuromuscular blockers,
and those that decrease gastric acidity are considered.
Lactobezoars are secondary to the use of milk formulas and are observed in newborns and preterm infants.
The polybezoars can be formed from a wide range of ingested materials,
such as metals and plastics3,4,5.
PREDISPOSING FACTORS
In the formation of bezoars numerous factors can cause influence,
including those that transform the anatomy and gastric emptying.
From postoperative situations such as gastrectomies,
intestinal tumors,
even emotional and behavioral disorders that may influence ingestion5,7,8.
Among the predisposing factors,
the formation of bezoar can occur in fiber-rich diets,
mastication disorders and previous surgeries in the gastrointestinal tract.
Cases of trichobezoars are often associated with psychiatric pathology and trichophagia.
CLINICAL PRESENTATION
Although a bezoar patient may remain asymptomatic for a long period of time or have only an abdominal discomfort,
the presence of a gastrointestinal bezoar may cause abdominal pain,
bleeding,
anorexia,
vomiting,
weight loss,
dysphagia,
palpable mass,
diarrhea,
or constipation,
intestinal obstruction and even perforation of the digestive tract3.
The clinical status of the patients is variable and depends on the location and size of the bezoar.
They may produce symptoms resulting from mechanical obstructive processes,
parietal compression and,
more rarely,
perforation of the gastric wall.
Also,
can cause nonspecific dyspeptic symptoms such as nausea and vomiting,
halitosis,
gastrointestinal bleeding,
anemia and malnutrition.
Diagnosis can be made based on clinical history and symptoms.
Any imaging method can assist this process,
be it a simple radiography with or without contrast,
ultrasonography,
computed tomography and even by means of magnetic resonance8,9.
Digestive endoscopy is the exam of choice,
providing in many cases the possibility of treatment,
either by fragmentation,
as a single therapy or in combination with other methods,
and may be valid in the case of phytobezoar.
IMAGING FEATURES
Different imaging studies can be used in the evaluation of bezoars.
Conventional abdominal radiographs usually indicate signs of obstruction on the gastrointestinal tract.
The image of a bezoar itself in this method is difficult to identify,
however if so a bezoar can be seen its image is not characteristic and can be shown as abdominal mass surrounded with gas,
and can be mistaken by abscess or even feces in the colon.
In these cases,
after the use of the oral contrast can be perceived a filling defect in the gastrointestinal tract,
allowing a better characterization of the bezoar. The sonography method of imaging can also reveal signs of bowel obstruction and in some cases it can demonstrate the presence of an intraluminal mass,
hyperecoic with a marked acoustic shadow.
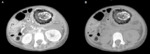
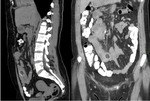
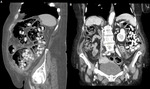
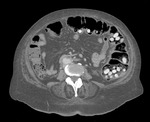
CT imaging is a sensitive method to determine the presence of a bezoar and other types of foreign body inside the gastrointestinal tract,
it can be useful in case to determinate its location,
and complications that can be associated.
It appears as a mass,
ovoid or round,
sometimes heterogeneous,
can show density lower than food particles,
with gas in between.
The following are clinical cases of bezoars:
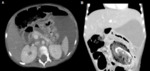
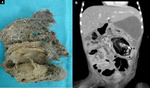
1) CASE 01 – Female,
05 years old,
admitted with acute abdomen,
diarrhea,
lowering of consciousness level and sepsis.
History of anorectal anomaly corrected and with colostomy on the left flank.
(Fig.
1) (Fig.
2) (Fig.
3)
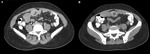
2) CASE 02 - Female,
40 years old,
presenting midline pain in the lower abdominal region associated with vomiting. Past of pancreatic cyst drainage with Roux-en-Y reconstruction.
(Fig.
4) (Fig.
5)
3) CASE 03 – Female,
56 years old,
presenting abdominal pain.
Clinical history of olive ingestion.
(Fig.
6) (Fig.
7)
DIFFERENTIAL DIAGNOSIS
Several conditions are part of the differential diagnosis bezoar,
some of the will be listed below:
1) Feces
An important differential diagnosis is the presence of feces in the small bowel that can cause obstruction in some cases.
The CT can demonstrate feces with ab amorphous shape and affect longer segments of the intestinal tract.
2) Foreign body accidentally or not accidentally ingested
The presence of a foreign body inside the abdominal cavity is an important differential diagnosis.
In these cases the image characteristics are variable,
depending on the type of material that was ingested,
including coins,
keys,
bones and batteries.
3) Retained surgical materials
Despite the care taken in the intraoperative act,
it is still a recurrent presentation.
This can lead to complications including adhesions,
perforation,
and abscess or fistula formation.Surgical retention materials is seen as a soft-tissue-attenuation mass and may show a whorled texture or a spongiform pattern containing gas,
and can show the presence of a radiopaque marker.
TREATMENT AND PROGNOSISIn those cases that bezoars appear with small dimensions an endoscopic treatment can be effective,
either by fragmentation,
as a single therapy or in combination with other methods,
and may be valid in the case of phytobezoar.
Endoscopic and combined drug therapy is successful in more than 90% of gastric bezoars and surgery is usually reserved when failure or complication occurs.
Therefore,
the treatment of a bezoar will depend significantly on location and cause,
in addition to the condition of presentation3. In bezoars with large dimensions the surgical treatment has the highest success rates,
removing it effectively as well manage a few of the complications that may appear.