Helminthic Diseases
Helminthic diseases include ascariasis,
trichuriasis,
schistosomiasis,
strongyloidiasis and fasciola,
among others.
They are highly prevalent,
affect world wide,
and include flat,
tape and round worms.
These parasites are spread commonly by fecal – oral route,
skin penetration by larvae,
and vector arthropods (4,
5).
Helminthic diseases have high morbidity & mortality rates,
affecting around 2 billion people globally.
Children are among the most affected with malnutrition,
anaemia,
and bowel obstruction.
They cause complications such as iron deficiency anaemia,
seizures,
portal hypertension and chronic diarrhoea (5).
Ascariasis
It is the most common round worm parasite,
they may grow up to 40 cm,
and its larva develops in the lungs to then travel to the abdomen causing symptoms such as abdominal pain,
distension and weight loss (5).
Rarely,
this parasite may cause complete or partial obstruction [Fig.
3 and 4].
More frequently,
ascaris are seen incidentally on abdominal imaging studies [Fig.
5].
On computed tomography they are seen as elongated filling defects within the bowel lumen [Fig.
6 and 7] (5).
Just like on computed tomography,
ascaris can also be seen using ultrasound,
where they appear round and elongated,
with two echogenic internal lines that represent the worm’s digestive tract [Fig.
8].
High experience is required to find these worms inside a patient’s bowel.
Ultrasound advantages include lack of radiation,
particularly important for children,
and evaluation of worm’s movements in real time (5).
Ascaris can travel though any orifice in the digestive tract.
They can even ascend through the biliary tract and can be seen in the gallbladder [Fig.
9].
Therefore,
it is not strange either for these worms to migrate into the intrahepatic or extrahepatic bile ducts [Fig.
10 and 11].
Migrating ascaris may cause complications such as: biliary obstruction,
cholecystitis,
pancreatitis [Fig.
12-16],
liver abscess,
bowel obstruction and aspiration (5).
Trichuriasis
Trichuriasis is the third most common roundworm found in humans.
They are spread by fecal-oral route,
and they inhabit the colon,
attaching to the colonic mucosa,
and may produce massive infestation.
On CT they are seen as small and elongated filling defects [Fig.
17 and 18] (4,
5).
Schistosomiasis
Schistosomiasis is produced by flatworms,
between 8 – 15 mm in size,
infecting over 200 million people,
mainly in areas with poor sanitation.
They are composed by S.
mansoni,
S.
japonicum and S heamatobium [Fig.
19].
They are prevalent in South America,
Africa,
Asia and Middle East and snails are the intermediate hosts. Humans become infected by skin penetration of larva,
which then migrate to target organs causing fibrosis.
Worms are too small to be seen on imaging,
and their imaging manifestations depend on the fibrotic reaction within target organs (5,
6).
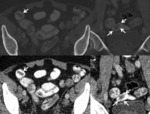
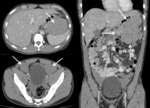
The most frequent target organ for S.
haemtobium is the lower urinary tract,
where eggs induce fibrosis and calcifications that can lead to obstruction and renal failure.
In the bladder,
the pathologic changes are seen as increased wall thickness and calcifications as in this case with diffuse bladder wall calcifications [Fig.
20].
Additionally,
urinary involvement is seen more frequently in children in endemic areas (5,
6).
In the liver,
schistosomiasis induces periportal fibrosis,
with portal vein occlusion and portal hypertension,
not distinguishable from other causes of chronic liver disease.
On ultrasound the infected liver shows an irregular surface pattern,
with echogenic septa outlining polygonal areas of relatively normal liver parenchyma.
There can also be septal and capsular calcifications [Fig.
21] (5,
6).
At advanced stages,
eggs migrate to various sites including the lungs,
kidneys,
brain and spinal cord,
and more frequently to muscles throughout the body.
They are seen as multiple soft tissue calcifications [Fig.
22] (6).
Strongyloidiasis
Mainly represented by S.
stercoralis,
these roundworms are less than 1mm in size,
infecting over 30 million people,
with increased incidence in immunocompromised patients.
Larva may infect humans via ingestion or by skin penetration,
reaching the intestinal mucosa,
where they mature and produce eggs,
invading the mucosa and inducing severe inflammatory reaction [Fig.
23] (5).
Strongyloidiasis infection manifests as abdominal pain,
nausea,
vomiting,
malabsorption and diarrhea.
They produce wall edema and fold thickening and can infect any portion of the gastrointestinal tract [Fig.
24] (5).
Protozoan
Amebiasis
Amebiasis is produced by entamoeba histolytica,
which is endemic worldwide.
It infects 10% of the world’s population,
and is prevalent in India,
Africa,
Far East,
and Central and South America,
being travellers,
immigrants from endemic areas and institutionalized patients at elevated risk (7-10).
Its main presentations are colitis with bloody diarrhoea,
amebomas,
and liver abscesses (7,
10,
11).
Colitis due to amebiasis is a transmural inflammatory colonic process with a variable and non-specific appearance; typically involving the cecum and rectum [Fig.
25],
usually with skip areas of involvement.
Ulcerations are usually present,
as well as moderate pericolonic fat stranding.
If left untreated they may result in ischemia and perforation [Fig.
26] (7,
9,
10).
Amebomas or amebic granulomas,
are an infrequent complication of amebiasis,
characterized by granulation tissue of the colonic wall surrounding infected amebic ulcerations.
Amebomas occur in up to 2% of cases of amebiasis,
they are most commonly solitary and in the right colon,
mainly involving the cecum [Fig.
27].
These lesions may mimic colonic tumours on computed tomography,
manifesting as concentric irregular wall thickening of colonic walls (12).
Amebic liver abscesses are produced by migration of colonic amebas via the portal vein,
and are the most common complication of invasive amebiasis.
The majority of amebic liver abscesses present on the right lobe (70-75%),
they’re usually smaller than 6 cm (50%),
and are multiple in up to 30% of patients.
Internal septations (30%) and adjacent liver perfusion abnormalities are commonly seen on imaging [Fig.
28,
29 and 30] (9,
11).
On ultrasound,
amebic abscesses have a variable echogenicity,
mainly hypoechoic with low-level internal echoes.
On CT they appear as oval or round low-density lesions,
with enhancing walls and adjacent edema.
They also demonstrate heterogeneous content,
with internal septations and fluid – debris levels.
Complications of liver abscesses include rupture into the pleural,
peritoneum,
or pericardium spaces [Fig.
29 and 30] (9).
Indications for drainage of hepatic abscesses include features that increase the risk of rupture,
such as: location in the left hepatic lobe,
size greater than 5 cm in diameter,
proximity to the diaphragm or pericardium and subcapsular location.
Other indications include poor response to treatment and for the purpose of differentiating from bacterial origin.
Because of haemorrhage into the cavities,
the abscess may be filled with a chocolate–colored,
pasty material,
known as “anchovy paste” [Fig.
31]. However,
most amebic abscesses may have bacterial secondary infections and purulent material is usually obtained on drainages.
Amebic identification on aspirated fluid is difficult,
because they tend to localize in the periphery of the lesion (9).
Mosquito borne infections / Virus
They are mainly transmited by the aedes Aegypti mosquito [Fig.
32].
Malaria
Malaria is a life threatening infection caused by plasmodium parasites,
which grow within red blood cells inducing hemolysis.
The mosquito globally distributes it and it is also endemic in South America,
Africa and Asia,
with a particular high mortality rate in Africa.
Its main symptom is an episodic fever (13).
On imaging,
the principal finding is splenomegaly,
usually with multiple wedge-shaped low attenuation areas that represent splenic infarcts.
Splenic rupture may occur,
producing subcapsular hematomas [Fig.
33].
Hepatomegaly,
gallbladder and periportal edema can also be seen as non-specific findings (13).
Dengue
Dengue is a mosquito-borne viral infection,
widely distributed and prevalent,
infecting up to 40% of global population,
with frequent outbreaks thoughout the world.
Its main symptom is fever with intense myalgia.
In its physiopathology,
this condition decreases platelets,
increasing a tendency to bleed (14).
Imaging findings are non-specific,
and include moderate hepatomegaly,
with gallbladder and periportal edema,
free fluid and pleural effusion [Fig.
34] (14,
15).
In some cases,
bleeding may be the presenting symptom [Fig.
35 and 36].
Chikungunya
Many other viral infections produce non-specific imaging findings in the abdomen,
including Hepatitis A – E,
yellow fever,
herpes and cytomegalovirus.
For instance,
Chikungunya virus may produce acute hepatitis,
with hepatomegaly and heterogeneous enhancement following contrast administration [Fig.
37 and 38].
Mild splenomegaly,
enlarged lymph nodes,
and joint effusion can also be seen (16).