Between November 2016 and October 2017 we performed 73 CT guided transthoracic biopsies aquiring scans with 16-slice CT.
All patients have been recruited by clinicians according to previously taken CT or PET-CT exam,
they were hospitalized and observed at least 24 hours after biopsy.
All patients signed informed consent for the procedure.
Patients were 30-84 years old and male to female ratio was M:F=41:32.
Undetermined lesions of lung parenchyma,
mediastinal and pleural lesions were included in this retrospective study.
Contraindications
Absolute contraindications for transthoracic biopsies were platelet count < 50,000/mL and a PT < 0,5 due to bleeding tendency.
Relative contraindications were large pleural effusions,
very small and unreachable lesions and very anxious and noncompliant patients.
Planing biopsy
Previously taken CT exam was used to carefully plan biopsy.
We were evaluating:
- lesion size and location
- depth od the lesion,
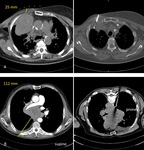
Fig.
2.
- safe access/pathway
- patient position (supine,
prone,
decubitus or oblique)
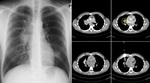
- relation of the lesion to bones,
adjacent organs,
blood vessels,
Fig.
5.
- vascularity/enhancement of the lesion
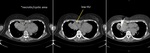
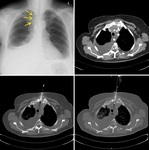
- lesion morphology (to avoid possible necrotic/cystic areas),
Fig.
1.
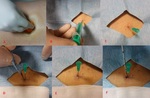
- angulation of the needle (to avoid bones and vital structures,
to reduce incidence of pneumothorax),
Fig.
4.
- need to apply i.v.
contrast during biopsy procedure,
Fig.
3.
We have noticed much better patient compliance when in prone position,
probably because not visualizing the procedure reduces patient anxiety and sudden movements.
Biopsy procedure
Non-contrast CT scans were mostly aquired during biopsy procedure if enough information was provided with previous ones.
If not,
the i.v.
contrast was applied in order to better differentiate blood vessels and proximity of other adjacent organs.
We were using mostly 16G cutting needle (10,
15 and 20 cm lenght) deployed with co-axial technique through the introducer needle.
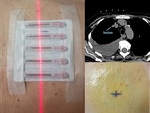
The set of connected needles was used as radiopaque marker to precisely determine the puncture site (Fig.
7.).
The puncture site was first carefully washed,
then the local anesthetic was applied.
The syringe was detached and the needle was left in the skin for guiding purpose.
The small incision was made with scalpel and the introducer needle was advanced through skin incision.
A 16G cutting needle was advanced through the guide needle.
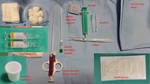
Collected tissue samples were deployed on the sponge embedded cassette,
put in the formalin container and sent to pathology department (Fig.
6-9.)
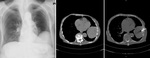
At least two tissue specimens were collected whenever possible,
and even more when complicated further immunohistochemical or molecular analysis was expected.
Control CT scan was performed immediately after the procedure to rule out possible complications (pneumothorax and/or hemorrhage) and afterwards (following hours or days) the control chest X-rays were performed if necessary.