We reviewed the cases of acute pelvic pain in pregnant and puerperal women presented in our hospital between 2007 and 2017 and selected the 10 most representative pathologies:
OBSTETRIC
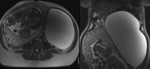
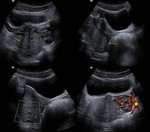
CORPUS LUTEAL CYST Fig. 1
Corpus luteal cysts (CLC) represent the most common pelvic masses in the first trimester of pregnancy.
CLC are a type of functional ovarian cysts that result when a corpus luteum fails to regress following the release of the ovum.
Instead,
it enlarges with or without hemorrhage,
forming a cyst that tends to involute at the end of the second trimester.
IMAGING FINDINGS
- US:
Thick walled cyst,
that when complicated,
can have lace shaped echoes within.
Doppler shows peripheral hypervascularity forming the "ring of fire" sign.
- MRI:
Cystic ovarian lesion homogeneously hypointense in T1,
typically hyperintense on T2 with intense wall enhancement.
The main differential diagnosis in pregnant women is an ectopic pregnancy.
Free fluid might be asociated.
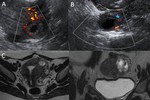
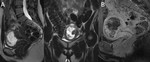
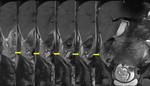
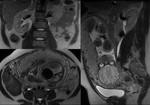
DECIDUALIZED ENDOMETRIOMA Fig. 2
During pregnancy,
increased progesterone levels promote hypertrophy of the endometrial stromal cells and formation of the vascular decidual lining of the uterus.
Endometrial stromal cells within endometriomas may also respond to the hormonal changes of pregnancy by forming vascular mural nodules.
- US:
An endometrioma that has undergone decidualization increases in size and is more complex in appearance,
with solid mural nodules or papillary excrescences that may show vascularity on Doppler imaging.
- MRI:
Similar changes might be seen on MRI.
An imaging feature that may be specific for decidualized endometriosis is the T2 signal hyperintensity of the mural nodules,
which are isointense relative to the thickened decidualized endometrium.
After childbirth or termination of a pregnancy,
decidualized endometriosis has been reported to either resolve or regress to uncomplicated endometriomas.
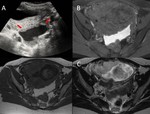
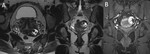
ECTOPIC PREGNANCY Fig. 3
Ectopic pregnancy is the most common cause of pregnancy-related mortality in the first trimester.
The main risk factors include a history of ectopic pregnancy,
tubal surgery and pelvic inflammatory disease.
Most patients present with a 5-9 week history of amenorrhea,
mild pelvic pain and vaginal spotting
IMAGING FINDINGS
- US:
o Tubal Pregnancy: Represent 95% of ectopic pregnancies and most of them occur in the ampulla.
Common findings include the presence of a complex adnexial mass with the "tubal ring" sign,
an hyperechoic ring surrounding an extrauterine gestational sac.
On Doppler imaging we can see the "ring of fire" sing that translates the peripheral hypervasculatity.
Intrauterine findings include a normal endometrium and the presence of a pseudogestational sac,
represented by a thick decidual reaction surrounding intrauterine fluid with no embryo.
o Interstitial Pregnancy: Uncommon condition that counts for 2-4% of ectopic pregnancies.
Interstitial pregnancies occur when the gestational sac implants in the intramyometrial segment of the fallopian tube.
US findings include an eccentrically located gestation sac surrounded by a thin layer of myometrium of less than 5mm.
Because of it's location,
on proximity to the uterine artery,
the rupture of an interstitial pregnancy can lead to life-threatening hemorrhage.
- MRI:
o Tubal pregnancy has been described as a saclike cystic tubal structure with a thick wall.
The wall typically demonstrates high signal intensity on T2w.i.,
and frequently there is associated hemorrhage.
The cystic gestational sac–like component may contain foci of acute hemorrhage characterized as regions of intermediate or high signal intensity on T1w.i.
o Interstitial pregnancies can manifest as heterogeneous masses with predominantly high T2 signal intensity located just lateral to the uterine cornua.
The lesion is contiguous with the uterine myometrium owing to the implantation within the intramural portion of the fallopian tube.
o Aditional findings often include hemoperitoneum and in the cases of tubal pregnancy hematosalpinx.
In most cases a true gestational sac is missing.
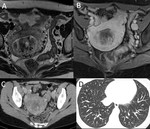
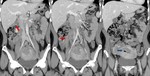
GESTATIONAL THROPHOBLASTIC DISEASE Fig. 4
Gestational trophoblastic disease (GTD) is a spectrum of both benign and malignant gestational tumors,
including hydatidiform mole (complete and partial),
invasive mole,
choriocarcinoma,
placental site trophoblastic tumor,
and epithelioid trophoblastic tumor.
The latter four entities are referred to as gestational trophoblastic neoplasia (GTN).
The beta-hCG level is a useful serologic marker for diagnosis,
assessment of response to treatment,
and surveillance for recurrence.
MOLAR PREGNANCY
Hydatiform mole can be complete (CHM) or partial (PHM).
Because of routine use of sonography and β-hCG testing,
patients with CHM are often diagnosed early in gestation and are often asymptomatic at the time of diagnosis.
Common presenting symptoms include vaginal bleeding large-for date uterine size,
and hyperemesis.
Patients with PHM are less likely to be diagnosed before uterine evacuation,
and the diagnosis is usually made with histologic analysis of curettage specimens after incomplete or missed abortion.
IMAGING FINDINGS
- US:
The most common finding of CHM during the first trimester is an enlarged uterus filled with a heterogeneous echogenic mass with several hypoechoic foci,
resulting in the so-called "snowstorm appearance".
In addition to the small cystic spaces,
larger irregular fluid collections may be seen in the endometrial mass. With advancing pregnancy (particularly 2nd trimester),
the small cystic spaces become larger and more numerous at imaging.
The fetus or fetal parts are absent,
except in the rare event of a CHM with a coexisting diploid twin.
In some cases we can see multiple large,
bilateral,
functional ovarian cysts called theca lutein cysts that result from ovarian stimulation by the high level of β-hCG.
US findings suggestive of PHM include:
o Empty gestational sac or one containing amorphous echoes representing fetal parts.
o Elongated or ovoid gestational sac.
o Fetal demise,
anomalies,
or growth restriction.
o Oligohydramnios.
o Enlarged placenta relative to the size of the uterus with internal cystic change producing a “Swiss cheese pattern”.
Differentiating between PHM and CHM carries prognostic significance because of the higher rate of postmolar GTN in CHM (15%–20%) compared with PHM (<5%).
- MRI:
Pelvic magnetic resonance (MR) imaging has a limited role in assessment of molar pregnancies and is usually performed when US doesn't show clear findings or is inadequate.
In CHM and PHM early in the first trimester,
little or no abnormality may be visible.
When visible the tumor might be shown as an expansile heterogeneous mass distending the uterine cavity with high signal intensity on T2-w.i.
and low signal intensity on T1-w.i.
relative to the normal myometrium.
With advancing pregnancy,
numerous small internal cysts can be seen within the endometrial mass on T2-w.i.
with a thin rim of hypointense myometrium surrounding the mass.
The interface between the myometrium and the molar mass is typically sharp and smooth.
Numerous signal voids can be seen in the myometrium and adnexa,
representing dilated vessels due to intratumoral arteriovenous shunting and tumor neovascularity.
After administration of gadolinium contrast,
moles typically demonstrate enhancing heterogeneous tissue containing multiple small cystic spaces within the distended endometrial cavity.
GESTATIONAL TROPHOBLASTIC NEOPLASIA
GTN refers to the malignant entities in the spectrum of GTD and includes invasive mole,
choriocarcinoma,
placental site trophoblastic tumor (PSTT),
and epithelioid trophoblastic tumor (ETT),
being the last two fairly rare.
Represents the presence of molar villi beyond the site of initial implantation in the myometrium or in a distant site.
Clinically it presents as persistent vaginal bleeding,
uterine subinvolution or asymmetric enlargement.
Choriocarcinoma is a malignant trophoblastic tumor that presents with regional invasion and distant metastases to lungs (80%),
vagina,
liver and brain through hematogenous dissemination.
Half of the choriocarcinomas present any time after term pregnancy and 25% after molar pregnancy.
IMAGING FINDINGS
- US:
The sonographic appearance of GTN is not specific for any particular variant and may be difficult to differentiate from those of benign uterine processes,
including fibroids,
adenomyomas,
retained products of conception,
or primary and secondary pelvic malignancies.
Accurate diagnosis depends on correlation with clinical findings and β-hCG levels.
- CT:
While CT is useful in evaluation and staging of metastatic disease,
it has a limited role in evaluation of the primary tumor.
Nevertheless,
the primary tumor may be seen as a focal low-attenuation mass within an enlarged uterus that typically involves the myometrium
- MRI:
The MR imaging appearance of GTN is nonspecific,
and differentiation between the various types of GTN is limited.
Accurate differentiation between GTN and benign processes such as retained products of conception is difficult.
MR imaging features include a sharply emarginated or ill-defined mass centered within the myometrium that distorts or displaces the junctional zone.
Such a mass is usually isointense on T1-w.i. and hyperintense on T2-w.i.,
relative to the normal myometrium,
with avid enhancement after intravenous administration of gadolinium contrast material.
Areas of increased signal intensity on T1-w.i.
may be seen due to hemorrhage.
Numerous prominent vessels are typically seen within the myometrium surrounding the tumor due to increased vascularity.
GYNECOLOGIC
OVARIAN TORSION Fig. 5
Ovarian torsion is defined as the total or partial rotation of the adnexa around its vascular axis or pedicle.
The most common trigger is an adnexal or paraadnexal mass that favors the mobility of pelvic structures.
The risk of ovarian torsion rises (x5) during pregnancy.
Its most common cause in pregnancy is a corpus luteum cyst,
which usually regresses spontaneously by the second trimester.
Ovarian torsion,
therefore,
occurs most frequently in the first trimester,
occasionally in the second,
and rarely in the third.
However,
it can also ocur in the absence of a cyst,
due to the normal increase of size and engorgement of the adnexa that takes place during pregnancy.
IMAGING FINDINGS
- US:
The main finding is an increase in the size of the ovary to >10 cc.
The ovary is usually displaced toward the midline and above the fundus of uterus.
We can also find the “pearl necklace sign”,
which corresponds to the ovarian follicles displaced peripherally. Doppler is useful for prognosis because arterial flow is a sign for viability.
In the second and third trimesters of pregnancy,
the ovaries are sometimes difficult to visualize ultrasonographically,
because they are displaced from the pelvis by the enlarging uterus.
- MRI:
If the ovaries are not clearly visualized with vaginal or abdominal ultrasound,
MRI can be used.
Findings are non-specific.
The most common finding is an enlarged ovary that is displaced toward the midline with a thick edematous pedicle.
The uterus can be displaced towards the contralateral side.
There can be some T1 hyperintense foci consistent with hemorrhage and some free pelvic fluid.
MYXOID DEGENERATION OF LEIOMYOMA
Leiomyoma are generally firm and rubbery solid tumors.
Sometimes they can undergo different types of degeneration including hyaline,
myxoid and cystic degeneration,
dystrophic calcification and red degeneration.
Hyalinization is the most common type,
occurring in up to 60% of cases.
Myxoid leiomyomas are histologically a subtype composed mainly of smooth muscle cells,
with significant accumulation of a cellular material rich in mucin.
- US:
In ultrasonography,
degenerative leiomyoma is commonly hypoechogenous and excessive degeneration may be recognized as a cystic pattern.
- MRI:
On pelvic MRI,
the myxoid material usually demonstrates T1 low signal intensity,
T2 very high signal intensity and minimal or no enhancement.
VASCULAR
UTERINE ARTERIOVENOUS MALFORMATION Fig. 7 Fig. 8
Arteriovenous malformations (AVM) are abnormal communications between the arteries and veins.
The veins receive blood directly from the arteries without the intervening capillary beds and channels so they operate and receive blood at higher pressures.
Events that predispose a uterus to AVM include uterine surgery,
endometrial evacuation and infective processes like endometritis,
septic abortions and infected retained products of conception.
The normal artery-vein channels are disrupted and re-anastomosis occurs in a suboptimal/abnormal tissue.
Hormonal changes,
mainly pregnancy,
menstruation and high dose estrogen-progestin trigger bleeding episodes.
However the exact mechanism is still unknown.
IMAGING FINDINGS
- US :
Sonographic appearances can be non-specific and can have a range of manifestations including: areas of subtle myometrial inhomogeneity; tubular spaces within the myometrium,
enlarged parametrial vessels; or an intramural,
endometrial or cervical mass like-region.
Doppler usually shows a low resistance and high velocity flow pattern.
- MRI:
Multiple serpentine flow-related signal voids are seen in the uterine wall,
endometrial cavity and parametrium on T1- and T2-w.i.
Contrast-enhanced dynamic MR angiography can depict complex serpentine abnormal vessels that enhance as intensely as normal vessels,
show early venous return,
and demonstrate the extent of the malformation.
OVARIAN VEIN THROMBOSIS Fig. 9
Ovarian vein thrombosis is a rare condition occurring in the early postpartum setting.
It is also known to be associated with other conditions such as malignancy,
pelvic inflammatory disease,
inflammatory bowel disease,
sepsis and recent pelvic or abdominal surgery.
The clinical manifestations may be variable,
from asymptomatic or vague abdominal pain to sever complications such as pulmonary embolism or sepsis.
The differential diagnosis includes most conditions that affect the abdominal lower quadrant such as acute appendicitis and inflammatory bowel diseases.
IMAGING FINDINGS
The diagnosis is most commonly made with contrast-enhanced CT,
but CT and magnetic resonance imaging (MRI) are equally sensitive for detecting this disorder,
and both are more sensitive than ultrasound.
- CT:
The presence of a filling defect in a tubular structure anterior to the psoas muscle with a central round low-attenuation center and peripheral higher attenuation rim is the classic imaging finding .
There is often perivascular edema and venous tortuosity.
- MRI:
On MRI,
the venous thrombus may appear as a hyperintense filling defect on T1-w.i.
and may appear isointense to hypointense to the surrounding blood on T2-w.i.
The lack of filling of a large,
tortuous puerperal ovarian vein can be seen on time-of-flight MR venography.
NON-OBSTETRIC FREQUENT CONDITIONS
ACUTE APPENDICITIS Fig. 10
Acute appendicitis is the most common non-obstetric emergency requiring surgery during pregnancy.
Normal physiologic and anatomic changes in pregnancy limit the use of clinical signs that suggest a diagnosis of appendicitis (eg,
absence of right lower quadrant pain and the presence of nausea,
vomiting,
and leukocytosis in normal pregnancy) and therefore diagnosis can be delayed.
Appendicitis in pregnancy is associated with premature labor,
fetal morbidity and mortality,
and a higher rate of perforation.
IMAGING FINDINGS
- US:
Ultrasound is the first-line test showing good sensitivity,
specificity and accuracy without radiation exposure. The ability to image the appendix was greater in the first and early second trimesters.
Later visualization improvesin left lateral decubitus position.
There is superior migration and rotation of the appendix as pregnancy progresses.
This decreases the sensitivity of US in late pregnancy.
Therefore,
if US results are negative or indeterminate for appendicitis and a definitive alternative diagnosis is not identified,
further imaging is required to diagnose or exclude appendicitis and other diagnoses.
- MRI:
Common findings of appendicitis include an appendix with a fluid-filled lumen,
edema in the appendix's wall and nflammatory changes in the surrounding fat.
- CT:
If MR imaging cannot be performed (contraindicated or not available),
CT of the abdomen and pelvis should be used as a second-line test.
Intravenous and oral contrast agents are preferred to improve visualization of the appendix.
HYDRONEPHROSIS Fig. 11
It is estimated that up to 90 percent of women have some degree of asymptomatic dilatation of the renal calyces,
the renal pelves and the upper two-thirds of the ureters during pregnancy.
This limits accurate diagnosis between physiological hydronephrosis and true obstructive hydronephrosis.
Urolithiasis is the most common painful non-obstetric condition and non-obstetric cause for hospitalization in pregnant patients. Fortunately most ureteral calculi in pregnant patients have been reported to pass spontaneously.
However,
if misdiagnosed or inadequately treated,
urolithiasis can be complicated by pyelonephritis and premature labor induced by renal colic,
with or without coexisting infection.
IMAGING FINDINGS
- US:
A frequently encountered diagnostic challenge is the difficulty in distinguishing obstructive hydronephrosis from physiologic dilatation.
Absence of a ureteral jet on the suspected side of obstruction has been reported to have a good sensitivity and a specificity.
Patients should be imaged in the contralateral decubitus position to decrease false positive results .
US is somewhat time-consuming and requires hydration,
however it's suggested as a first-line test because it does not involve the use of ionizing radiation or iodinated contrast material,
is noninvasive,
and is relatively cost-effective.
A normal sonogram may obviate the use of further imaging if there is no continuing clinical concern about a significant alternative diagnosis.
- MRI:
MR urography should be considered as a second line test when use of US fails to establish a diagnosis and there are continued symptoms despite conservative management.
Renal enlargement and perirenal fluid suggestive of obstruction were absent in physiologic dilatation.
In addition,
physiologic dilatation demonstrated a characteristic tapering due to extrinsic obstruction of the middle third of the ureter by the uterus.
Physiologic renal and ureteral dilatation is more common on the right.
- CT:
The high accuracy of the technique for detection of calculi in the general population together with the new low-dose multidetector CT have lowered the threshold for use of abdominal and pelvic nonenhanced CT as a second-line test in pregnancy.