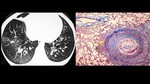
We performed a retrospective search of patients with radiologic manifestations compatible with bronchiolitis,
selecting the most representative cases,
most of them with pathological correlation
BRONCHIOLAR CLASSIFICATION
The bronchiolar classification of bronchiolitis classify the bronchiolar disorders into primary with the affectation of the bronchiole and another disease with secondarily involved in the bronchiole.
(Figure 7)
PRIMARY BRONCHIOLAR DISORDERS
Constrictive bronchiolitis
Also known as obliterative bronchiolitis is characterized histologically by peribronchiolar fibrosis secondary of a chronic inflammation and submucosal scarring with resulting bronchiolar narrowing and air trapping.
The most common causes are idiopathic,
infections (adenovirus,
measles,
pertussis,
mycoplasma,
and tuberculosis),
toxic fume inhalation,
connective tissue disease,
graft-versus-host disease,
lung transplantation and drug reactions.
(Figure 8,
9,
10,
11) [4,
11,
12]
On high resolution computed tomography mosaic attenuation it’s a characteristic finding and result from hypoventilation and decreased perfusion of the areas of less attenuation with redistribution of blood flow to areas with normal or increase attenuation; expiratory computed tomography and the use of minimum intensity projection reconstruction increase the contrast between the normal and abnormal lung and make evident air trapping.
Other findings on computed tomography in constrictive bronchiolitis are bronchiectasis,
bronchiolectasis and bronchial wall thickening.
[2,
4]
Swyer-James- MacLeod syndrome represent a long-term complication of post infectious constrictive bronchiolitis particularly by adenovirus in early childhood with radiographic manifestations seen in adulthood.
Asymmetric expiratory air trapping and a mosaic of attenuation are the typical features of this disease.
[2,
4,
6]
Acute Bronchiolitis
Is the most common type of bronchiolitis and can be classified as acute or chronic.
Acute infectious bronchiolitis is most often in infants and children with infection for respiratory syncytial virus,
adenovirus,
parainfluenza,
influenza and less commonly mycoplasma and chlamydia.
Chronic infections (Pseudomona aeruginosa,
Aspergillus) and mycobacterial infections cause chronic bronchiolitis.
[2,
4,
6,
13]
Histologically it is characterized by a severe process inflammatory in the walls of the bronchiole,
edema,
exudate,
and necrosis of bronchiolar epithelium.
These findings are seen on high resolution computed tomography like peribronchial areas of consolidation,
ground-glass centrilobular nodules,
tree-in-bud opacities and bronchial wall thickening.
(Figures 12,
13,
14)
Diffuse Panbronchiolitis
It is most common in Asiatic patients and represents an idiopathic chronic bronchiolitis with chronic inflammation of paranasal sinus.
Findings on histology evidence intraluminal exudate and chronic inflammatory cells in the walls.
High resolution computed tomography demonstrates findings nonspecific: tree-in-bud pattern,
centrilobular nodules,
bronchiectasis,
bronchiolectasis and mosaic of attenuation.
[2,
4]
Respiratory bronchiolitis
It is a condition seen mostly in asymptomatic cigarette smokers,
however,
may occur with other inhalation exposure,
is characterized by an accumulation of hemosiderin-like pigment-laden macrophages in peribronchiolar airspace and alveolar space, chronic inflammation and finally fibrosis of the bronchiolar walls.
On High resolution computed tomography,
respiratory bronchiolitis manifests as ground-glass opacities and centrilobular micronodules with ground-glass density predominantly on the upper lobules.
(Figures 15) [2,
4]
Bronchiolitis related to toxic,
gases,
fumes and dust
There are other agents can cause bronchiolitis: acute exposure to smoke,
nitrogen dioxide. Initially,
these organic and organic agents produce an inflammatory process in the bronchiole wall that occasionally progress to obliterative bronchiolitis,
represented histologically by fibrosis and chronic infiltrate of its walls.
The findings on high resolution computed tomography are bronchiectasis,
attenuation mosaic,
and expiratory air trapping.
(Figures 16,
17) [2]
Follicular bronchiolitis
Follicular bronchiolitis is part of a spectrum of lymphoproliferative disorders,
almost mostly in association with autoimmune diseases,
connective tissue diseases,
infection and hypersensitivity reactions.
On histology demonstrates lymphoid hyperplasia with the formation of nodular lymphoid aggregates.
These findings represent on high resolution computed tomography solid or ground-glass centrilobular nodules.
(Figures 18) [2,
4,
6]
BRONCHIOLAR INVOLVEMENT IN INTERSTITIAL LUNG DISEASE
Hypersensitivity Pneumonitis
Also known as allergic bronchiolitis or extrinsic allergic alveolitis is characterized by the inhalation of organic dust that causes an immune-mediated inflammatory process in the peribronchiolar alveoli.
For unknown causes,
the smokers have a protective effect against hypersensitivity pneumonitis.
Their findings in high-resolution tomography are similar to a respiratory bronchiolitis: bilateral ground-glass opacity,
ill-defined centrilobular nodules with mosaic attenuation and air trapping,
these last two findings present in their chronic evolution.
(Figures 19) [2,
14]
Respiratory bronchiolitis associated with interstitial disease
Is there a strong relationship between the smokers and respiratory bronchiolitis,
from this group of patients a little proportion may be seen associated with interstitial lung diseases.Histological features are pigmented macrophages intraluminal and intraalveolar with peribronchiolar interstitial fibrosis.
The findings on high resolution computed tomography are no specific,
however,
some features include centrilobular nodules,
ground-glass opacification,
thickening of the interlobular septa,
thickening of the bronchi walls,
emphysema,
and mosaic of attenuation.
(Figures 20) [13,
14]
Pneumonia cryptogenic of organization
Previously known erroneously as bronchiolitis obliterans with organizing pneumonia (BOOP),
it’s a pathology that no always is idiopathic,
can be associated with an infection,
inhalation injury,
connective tissue disease,
drugs,
radiation,
aspiration or autoimmune disease.
On histology feature for a proliferation of connective tissue and granulation tissue in alveolar space with lesser bronchiolar involvement.
On high resolution computed tomography is associated with the unilateral or bilateral consolidation that can migrate on serial images with a tendency of central bronchovascular and subpleural distribution,
another findings include ground glass opacity,
bronchial wall thickening and reversed halo sign.
(Figures 21) [6,
13,
14]
BRONCHIOLAR INVOLVEMENT IN LARGE AIRWAY DISEASE
Chronic bronchitis,
bronchiectasis,
asthma
Bronchial abnormalities affect the large airway and have histologically changed include smooth muscle hyperplasia,
air wall edema,
mucous gland hyperplasia and mucostasis.
High resolution computed tomography findings atelectasis,
centrilobular nodules with upper lobe predominance,
bronchiolar wall thickening and air trapping.
(Figures 22,23) [13]