Bronchioles are small airways that do not contain cartilage in their walls located at the center of the secondary pulmonary lobule,
has an internal diameter less of 2 mm,
therefore,
they are not visible when are normal.
The thickening of its walls and the variable intraluminal exudate reflecting an inflammatory process or fibrosis named bronchiolitis,
term that encompasses a broad number of diseases [1,
2]
Bronchiolitis or small airway disease is a radiological finding very frequent in daily practice that requires an adequate anatomical knowledge for its correct identification.
There is currently no radiological consensus for its classification generating confusion among clinicians,
radiologists,
and pathologists.
However,
we consider bronchiolar classification as a practical and complete way of remembering small air disease.
Anatomy of the secondary pulmonary lobule
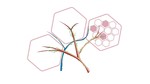
The secondary pulmonary lobule is the smallest functional anatomic unit of the lung.
It has a polyhedral morphology,
bounded by interlobular septa which contain pulmonary venules and lymphatic channels and its center has an arteriole pulmonary,
bronchiole and lymphatics.
(Figure 1)
The lung is supported by a network of connective tissue called the lung interstitium,
that could be visible on high-resolution computed tomography only if is thickening and has three components: the peribronchovascular interstitium that invests the pulmonary artery and bronchi,
continuing with the centrilobular interstitium that envelops the bronchiole and centrilobular arteries,
the subpleural interstitium locates in the visceral pleura and the intralobular interstitium a fine connective tissue between the center of the secondary pulmonary lobule and the interlobular septa.
[3]
The structures of the secondary pulmonary lobule identified on high-resolution computed tomography are only the arteriole pulmonary because the normal bronchiole it’s no visualized.
Nevertheless exist computed findings suggestive of bronchiolar disorder: Ground-Glass centrilobular nodules,
branching or Y-shaped centrilobular opacities (“tree-in-bud”),
bronchiolectasis,
mosaic attenuation,
air trapping and bronchiolar wall thickening.
[4]
Direct and indirect signs of small airway disease
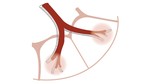
The ground-glass centrilobular nodules of bronchiolitis are airspace nodules ill-defined with less dense than vessels and distribution limited to centrilobular regions,
finding them usually centered 5 to 10 mm from the pleural surface,
spared the fissures and interlobular septa.
(Figure 2) [5]
The centrilobular nodules are not present only in airway disease,
they can also be present in interstitial and vascular diseases,
been important take into account the clinical history and the context of this patients.
For example,
when finding centrilobular peribronchovascular interstitial thickening and a lymphatic distribution of disease that include nodules in other locations like subpleural regions or interlobular septa think in interstitial disease but if the patient has a history of abusing pain medications and a new onset of pulmonary hypertension take in consideration Talcosis.
[5,
6]
Centrilobular nodules are seen in acute bronchiolitis,
diffuse panbronchiolitis,
respiratory bronchiolitis,
bronchiolitis related to toxic,
gases,
fumes,
follicular bronchiolitis and hypersensitivity pneumonitis.
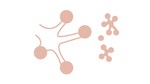
Another direct sign is branching or Y-shaped centrilobular opacities also named tree-in-bud opacities,
consists of nodules centrilobular with soft tissue attenuation connected to multiple linear structures that originate a single stalk and represent impaction with mucus,
pus or fluid of the centrilobular bronchioles.
Tree-in-bud is indicative of small airway disease and its most frequently recognized in patients with endobronchial spread of tuberculosis,
infectious bronchiolitis and noninfectious bronchiolitis (aspiration).
(Figure 3) [5,
7]
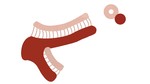
Two less common direct signs are the bronchiolectasis and wall thickening.
Bronchiolectasis is defined as dilatation of bronchioles by inflammatory airway disease or fibrosis and is considered dilated if the broncoarterial ratio exceed one (signet ring sign) and it is localized to 1 cm of the pleural surface.
(Figure 4,
5) [8,
9]
The mosaic attenuation pattern appears as a patchwork of regions of different attenuation and may represent: interstitial disease,
airway disease or vascular disease.
In a patient with airway disease,
the inflamed bronchioles or mucus impaction leads a partial or complete obstruction with air trapping secondarily and poor ventilation of lung parenchyma.
This area of less ventilation is poorly perfused because of reflex of vasoconstriction,
then the pulmonary vessels appear smaller in the areas of decreased opacity with air trapping in comparison with the areas of more density,
findings that are better visualized in expiratory high-resolution computed tomography.
(Figure 6) [6,
8,
10]
The differentiation with vascular mosaic attenuation is not easy,
but the dilated or thick-walled airway suggest the diagnostic of airway disease and the enlargement of the main pulmonary arteries a vascular etiology.