A - Diagnosis
Although IgG4-RD has been recognized as a new clinical entity worldwide,
uniform international criteria for diagnosing IgG4-RD have not yet been established.
The presence of many clinical mimics of IgG4-RD may result in over-diagnosis of this disease.
Histopathological examination of these lesions reveals both inflammatory elements in the form of a lymphoplasmacytic infiltrate,
often accompanied by a mild tissue eosinophilia,
and a fibrotic component characterized by “storiform” fibrosis.
Immunohistochemistry studies reveal a preponderance of IgG4-positive plasma cells [6].
Guidelines for diagnosis of IgG4-related disease were proposed by Umehara in 2011 ( Fig. 2 ).
Whether in general or subspecialty practice,
the radiologist has a critical role in suggesting the diagnosis of this multifocal disease.
Radiologists should be aware of the patterns of disease involvement and other inflammatory and neoplastic conditions,
which may exhibit similar imaging findings.
Computed tomography or magnetic resonance imaging will demonstrate enhancing focal mass lesions or diffuse infiltrative abnormalities; CT is optimal for assessing osseous involvement.
MRI,
with the advantage of superior soft-tissue characterization,
demonstrates intermediate to hypointense mass-like or infiltrative lesions on T2-weighted imaging.
Diffusion-weighted imaging (DWI) usually shows mild apparent diffusion coefficient (ADC) reduction,
the degree of which is dependent on tissue cellularity and fibrosis.
IgG4-RD lesions are FDG-PET avid,
which can be useful to identify asymptomatic multifocal disease,
facilitate planning for minimally invasive tissue sampling,
and to monitor treatment response [7].
B - DIVISION IN SEGMENTS
The involvement of salivary glands in IgG4-RD is termed IgG4-related sialadenitis.
Enlargement of major salivary glands is a common hallmark of this disease.
Sjögren Syndrome (SS) is the main differential diagnosis for salivary glands involvement in IgG4-RD.
Although the submandibular glands are most frequently involved in IgG4-RD,
the parotid,
sublingual,
and labial salivary glands may also be affected,
in contrast with SS in which the parotid enlargement is predominant.
Up to 40% of patients with IgG4-RD systemic disease presented with salivary gland involvement [8].
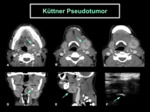
- Kuttner pseudotumor or chronic sclerosing sialadenitis
Küttners pseudotumor was first described by Küttner in 1896 as a hard tumor-like swelling of the submandibular gland.
Pathology shows lymphoplasmacytic infiltrate accompanied by prominent and progressive fibrosis.
Clinical symptoms are recurrent pain and/or swelling of the gland,
usually unilateral.
Ultrasound demonstrates a hypoechoic geographic area hypervascularized on color Doppler,
corresponding to the palpable mass.
CT and MR images are less specific showing post-contrast enhancement relative to the normal gland parenchyma and T2 sequence show a hypointense mass infiltrating the gland,
difficult to differentiate from lymphoma.
Sialoliths and mucous plugs were found in 29% to 83% of the lesions,
but remains unclear whether the sialolithiais is the cause or result of the underlying inflammatory process [9] ( Fig. 3 ).
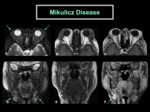
- Mikulicz disease (MD)
MD refers to idiopathic,
bilateral,
painless and symmetric swelling of the submandibular,
parotid and lacrimal glands. The enlargement of the affected glands is persistent and secretory dysfunction is either minor or not detectable,
with good response to corticosteroids.
The glands involvement does not need to be simultaneous and sequential involvement can occur over the years.
Sublingual glands can be involved in as many as 50% of cases ( Fig. 4 ).
There are clinical differences between MD and SS such as: female to male ratio is 2:1 in MD and about 20:1 in SS and salivary gland sialography is normal in MD.
Orbital involvement in systemic IgG4-RD (IgG4-ROD) is common among head and neck anatomical subsites,
second only to the salivary glands.
Conditions such as idiopathic orbital inflammatory syndrome (inflammatory pseudotumor) and lymphoid hyperplasia are now considered to be part of the IgG4-related disease spectrum [7].
There are 5 imaging patterns of orbital involvement in IgG4-RD ( Fig. 5 ):
- Lacrimal gland
The lacrimal glands are most commonly affected by IgG4-ROD and are often seen in association with salivary gland lesions,
as seen in Mikulicz disease,
and share similar imaging features.
Unilateral lacrimal gland lesions may occur and may be difficult to differentiate from infectious dacryoadenitis or lacrimal gland tumors with imaging alone.
Differential diagnosis includes extranodal marginal zone lymphoma (“MALT”) non-Hodgkin’s lymphoma,
Sjogren's syndrome and primary neoplasm ( Fig. 6 ).
- Extraocular muscle enlargement and diffuse orbital involvement
Extraocular muscles are often involved in IgG4-ROD and the most frequent presenting symptom are painless proptosis,
periorbital swelling and impaired extraocular muscle movement.
Concurrent lacrimal gland involvement and infiltration of orbital fat are common ( Fig. 7 ).
IgG4 typically spares the tendinous insertions of the extraocular muscles and the most commonly and most dramatically involved extraocular muscle is the lateral rectus.
Important differential diagnosis of extraocular muscle enlargement involvement include thyroid-associated orbitopathy and idiopathic inflammatory orbital pseudotumor.
Predilection for the inferior and medial recti involvement in thyroid-associated orbitopathy ( Fig. 8 ) with preserved tendon.
Enlargement of the entire muscle,
including the tendon in idiopathic inflammatory orbital pseudotumor,
are helpful findings to distinction this entities.
- Infraorbital nerve enlargement ( Fig. 7 )
Perineural spread has also been reported in orbital involvement,
often involving branches of the trigeminal nerve,
such as the frontal and especially,
infraorbital nerve.
The differential diagnosis includes perineural malignant spread from cutaneous malignancy tumour,
adenoid cystic,
carcinoma and lymphoma.
- Other ocular and orbital adnexal subsites
Eyelids,
lacrimal sac,
nasolacrimal duct,
uvea,
sclera and conjunctiva are other tissues may be involved in IgG4-ROD.
- Extraorbital IgG4-RD lesions with ophthalmic symptoms
IgG4-related soft tissue mass,
pachymeningitis and hypophysitis may involve cranial nerves within the orbital apex ( Fig. 9 ),
cavernous sinus and also the optic nerve on suprasellar region.
They may cause ophthalmoplegia or compressive optic neuropathy [10].
Pharyngeal and laryngeal manifestations of IgG4-RD are very rare and there are few scattered reports about this involvement,
such as subglottic and tracheal stenosis due to a dense fibrous enveloping mass and soft tissue thickening,
that can be asymmetric or circunferencial [11].
The described symptoms were hoarseness,
throat discomfort and cough,
usually with a long standing symptoms due to the difficulty in diagnosis ( Fig. 10 ,
Fig. 11 ).
So far,
four subcategories of IgG4-RD involving the thyroid gland have been identified ( Fig. 12 ):
- Riedel's thyroiditis is a chronic fibrosing disorder of unknown etiology that remains poorly understood,
long associated with systemic fibrosclerosing diseases,
many of which are now included within the spectrum of IgG4-RD.
- Hashimotos thyroiditis show a partial overlap with IgG4-related thyroiditis.
Patients with IgG4 related thyroiditis tend to be young men with a shorter disease duration,
higher anti-thyroglobulin and anti-thyroid peroxisomal leves,
and diffuse low echogenicity on ultrasound.
Other study demonstrated that more than 90% of cases classified as the fibrosing variant of Hashimoto's thyroiditis were associated with high IgG4 levels.
- Cases of Graves disease associated with IgG4-RD disease have also been reported,
with histologic examinations indicating no concomitant fibrosis or obliterative phlebitis,
only the diffuse lymphoplasmacytic infiltration of IgG4-positive plasma cells.
These disorders are frequently confused with malignancy due to the intense sclerosis of thyroid resulting in hard texture on palpation compounded by often-associated compressive symptoms.
Imaging demonstrates an enlargement of the thyroid gland and poorer contrast enhancement of the gland tissue compared with a normal thyroid tissue [9,
12].
Sinonasal involvement in IgG4-RD is rare and presents in imaging as a T2 hypointense mucosal thickening ( Fig. 13 ) or mass-like lesion ( Fig. 14 ) involving the sinus,
extending along the walls of contiguous structures and surrounding bone destruction.
It is important to understand that inflammatory disease is associated with an elevated number of IgG4 -positive plasma cells in tissue,
including rhinosinusitis,
so the diagnosis should be made carefully.
The differential diagnosis includes lymphoma,
Wegener granulomatosis and invasive fungal infection [13].
Lymphadenopathy associated with IgG4-related disease is typically painless,
either generalised or localised disease adjacent to an affected organ.
The location of lymphadenopathy often correlates with the presence of extranodal IgG4-RD [4].
- Temporal bone involvement
Temporal Bone involvement is very rare,
presenting with symptoms of chronic or recurrent otomastoiditis.
The low T2 signal intensity helps to differentiate the lesion from inflammatory process or other chondral lesions that present high T2 signal intensity ( Fig. 15 ).
Every effort should be made to exclude an infectious etiology,
prior to initiating immunosuppressive therapy [7].
Review of the literature suggests that 2 forms of large and medium-vessel disease may exist in IgG4-RD: a primary vasculitis (a condition in which the inflammation is centered on the vessel wall itself) and a secondary vasculopathy characterized by the compressive effect of the IgG4-RD tumefactive lesions.
Perugino et al.
[14] propose distinctive imaging patterns to differentiate primary and secondary IgG4-RD vascular involvement.
Primary IgG4-related vasculitis is defined by the presence of 1 or more of the following: vessel wall thickening; vessel wall enhancement on contrast study; or FDG avidity within the blood vessel wall on PET ( Fig. 16 ).
For the latter two features,
the intensity of these findings were required to exceed that of typical atherosclerotic disease.
Secondary IgG4-related vascular involvement was defined by abnormal perivascular soft tissue with minimal vascular wall findings.
The main radiologic findings were: enhancing soft tissue adjacent to or encasing the vessel; minimal vascular wall thickening or enhancement; FDG avidity in the perivascular region; and minimal arterial stenosis.
Whereas IgG4-related vasculitis predisposes to aneurysm formation and occasionally to dissection or perforation (marking an important contrast with other large-vessel vasculitides,
which usually leads to arterial stenosis),
secondary IgG4-related vasculopathy is more likely to cause luminal narrowing.
Clinical differences also exist between these two categories of vascular disease in IgG4-RD.
Patients with primary IgG4-related vasculitis have greater elevations in total serum IgG and are also much more likely to present with signs or symptoms directly attributable to the vascular involvement as opposed to those with secondary vasculopathy.
- Pachymeningitis,
skull base involvement and perineural spread
Pachymeningitis secondary to IgG4-RD is a form of hypertrophic pachymeningitis characterised by localised or diffuse inflammation and thickening of the meninges ( Fig. 17 ).
This type of involvement is more commonly seen in men.
Symptoms arise due to diffuse meningeal involvement leading to mechanical compression of cranial nerves or to more diffuse symptoms,
such as headache,
seizures and cognitive decline ( Fig. 18 ).
Parenchymal brain involvement is infrequently reported,
usually in association with pachymeningitis.
Perineural spread typically occurs in orbital,
trigeminal and paravertebral areas and the lesions are usually asymptomatic,
indolent and steroid responsive,
although they need differentiation from other potentially aggressive lesions.
Imaging findings are a perineural soft tissue mass or marked thickening and enhancement of the nerve ( Fig. 19 )[15].
IgG4-related hypophysitis is a rare disease that might be detected in 30% of hypophysitis cases and 4% of all hypopituitarism and/or diabetes insipidus cases.
Although the most important factor for the diagnosis of IgG4-related disease is histopathologic findings,
pituitary biopsy is a highly invasive procedure [16].
Imaging findings demonstrate thickening or mass formation within the pituitary stalk.
Swelling or mass formation within the pituitary gland is also noted ( Fig. 20 ).
MRI findings are nonspecific; however,
homogeneous enhancement is often seen on postcontrast T1-weighted images.
Associated pachymeningitis is occasionally seen [17].
Sarcoidosis,
germinoma,
Langerhans cell histiocytosis,
and tuberculosis are included in the differential diagnosis for sellar or suprasellar lesions in IgG4-related disease.
There is scarce reports of soft tissue involvement in IgG4-RD [18].
The image presents the typical imaging findings in MR images,
with an infiltrative pattern ( Fig. 21 ).