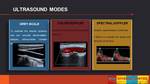
ULTRASOUND MODALITIES (Fig. 1)
- Gray scale or B-mode: it is use to evaluate the arteries anatomy and non vascular anormalities (plaques morphology,
intima-media thicknes…).
- Color Doppler: assessment of vascular flow and direction.
It enables rapid identification of abnormal blood flow,
but has low sensitivity.
- Spectral Doppler: graphic representation of the flow.
It allows to evaluate the speed and direction of the flow.
MAIN TECHNICAL PARAMETERS
- Doppler angle: ideally it should be a 45o-60o angle,
in wich range a linear relation exists between velocity and the Doppler shifts.
- Sample volumen box: it is the region of the US beam.
sensitive to the presence of echoes in the change of Doppler frequencies.
The optimal box size is 2-3 mm ant it should be placed in the center of the vessel and parallel to the direction of flow.
- Color box: its size must be adjusted and its orientation angled so that the angle of incidence on the blood flow is less than 60o.
- Color velocity scale control: it is the range of detected speeds.
In a normal carotid US study it should be adjusted by 30-40 cm/sec and if suboclusions exists,
the color velocity scale should be shifted down (<15 cm/sec).
- Color gain: increasing the gain amplifies adquired Doppler signal,
but also increases the noise.
Color gain should be set so that color reaches the intimal surface of the vessel.
HOW TO DO THE STUDY
The patient may lie down in thwe supine or semisupine position with the head hyperextended and tilted about 45o away from the artery being examined.
The study should be performed with a high-frequency linear array (7.5-10 mHz),
assessing the common carotid artery (CCA),
the bulb,
the carotid bifurcation and the internal carotid artery (ICA).
In certain short or muscular necks and with deep or high bifurcations,
the 5 mHz convex array may be useful.
A transverse and longitudinal planes basal B-mode study should be done to asses the presence and appearance of atheromatous plaques.
Color Doppler and spectral Doppler are use to evaluate the areas of turbulent flow and detect any stenotic segment in the vessel.
IMAGING FINDINGS
Diagnostic ultrasound offers the possibility of using both morphological and hemodynamic criteria. It is recommended to measure,
in addition to the hemodynamic parameters,
the thickness and length of the plaque as well as the residual lumen.
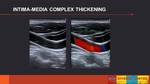
The intima-media thickness is consider an early sign of atherosclerosis and a risk factor to stroke and ischemic cardiopathy.
It should be measured on gray-scale image and a intima-media thick >1 cm is considered pathologic.
It should be take into account that a normal intimal thickening is releated to aging. (Fig. 2)
The plaque location,
morphology,
echogenicity and texture have to be described to predict possible future complications.
- Homogeneous plaque: uniform echogenity and texture.
This pattern is seen in a fibrous lesion,
often in the CCA. (Fig. 3)
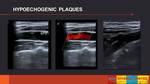
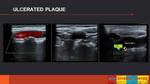
- Heterogeneous plaque: it has mixed areas of different echogenity and it may present ulcerated surface (depression >2 mm).
They are also called unstable or friable plaques. (Fig. 4 Fig. 5)
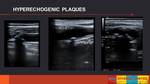
The most brightly echogenic areas are usually associated with calcium,
and hypoechoic content may represent lipid or intraplaque hemorrahge.
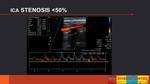
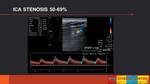
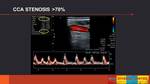
- INTERNAL CAROTID ARTERY (ICA) AND COMMON CAROTID ARTERY (CCA) STENOSIS (Fig. 6)
The typical ICA flow pattern is of low resistance,
with end-diastolic flow velocity well above the zero baseline.
To evaluate a ICA/CCA stenosis,
we have to determine the picosystolic velocity (PSV) in the area of greater stenosis and the morphological appearance of the atherosclerotic plaque in the B-mode image and with color Doppler.
The use of accessory criteria such as the PSV ICA/CCA ratio or end-diastolic velocity should only be reserved for isolated cases in which the main parameters were inconclusive (borderline values of PSV),
or in special clinical conditions that may condition the appearance of pitfalls (contralateral stenosis and tandem stenosis).
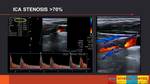
Severe ICA/CCA stenoses (> 70%) are hemodynamically significant,
so surgical treatment will be indicated (endartectomy or angioplasty).
The sonographic findings are: PSV >230cm/sec,
reduction of vessel lumen >50%, spectral broadening,
postestenosis tubulence at color/power Doppler imaging,
color aliasing despite high color velocity scale setting (>100 cm/sec),
end diastolic velocity >100 cm/sec and PSV ICA/CCA ratio >0.4.
The differentiation between a near occlusion and a total ICA occlussion is often a difficult task.
In this clinical situation,
velocity parameters may not apply and the color or power Doppler technique should be used in order to demonstrate a markedly narrowed lumen. (Fig. 7 Fig. 8 Fig. 9 Fig. 10)
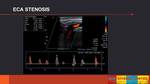
- EXTERNAL CAROTID ARTERY (ECA) STENOSIS
ECA supplies the face and the scalp and,
in general,
it is not a source of emboli to the brain.
The ECA Doppler spectrum has a high resistance waveform,the PSV is normally higher than the ICA because it is smaller peripheral vessel.
Disease in the ECA is often seen,
but is usually not of clinical import,
unless the ECA is serving as a collateral source of and occluded ICA. (Fig. 11)
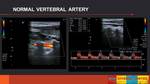
- VERTEBRAL ARTERY AND SUBCLAVIAN STEAL
The normal vertebral artery Doppler spectrum has a low resistance waveform,
similar to the ICA,
and antegrade flow direction. (Fig. 12)
Carotid US is not accurate for identification of a focal stenosis in the vertebral artery,
because it usually appear at the origin.
In case of subclavian steal sydrome,
the flow direction may be reversed.
There are three types of subclavian steals: occult steal (minimal hemodynamic changes),
partial subclavian steal (partially reversed flow) and complete subclavian steal (flow completely reversed). (Fig. 13)