SPOF in cancer imaging reporting
Certain pathologies are more commonly found in patients with cancer and should never be missed.
We have called these pathologies SPOF.
No matter how advanced the imaging technique or the oncology treatment,
missing a SPOF can lead to failure in the care pathway of the patient.
SPOF has been derived from literature review and analysis of our errors and discrepancy data.
SPOFs are associated with morbidity and mortality and identifying them can help alleviate the suffering of many different types of patients - from the palliative patient in their last days of life,
through to young fit patients with localised incidental cancer.
There is a large increase in oncology scans which are becoming increasingly complex with more time pressures on the radiologist.
SPOF will allow a quick way to ensure that these things are not missed.
SPOF Overview

Fig. 1: Single Point of Failure
References: SPOF
>>>>>>> TEACHING CASES USING SPOF <<<<<<<<
S – Spine
Spinal cord compression
Invasion of the bony malignant disease into the spinal canal can often be seen on CT.
However,
this is often under-called or missed altogether.
Picking up the spinal metastasis is part of the observation,
careful inspection to check for neural involvement is key to expedite treatment to save neurological function even in patients with advanced metastatic disease.

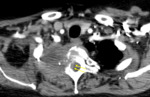
Fig. 2: Malignant spinal cord invasion not stated on initial report. This 75-year-old patient was diagnosed with a right Pancoast tumour with vertebral involvement (contrast enhanced CT axial). The initial report however did not appreciate the enhancing soft tissue component (arrows) in the right lateral aspect of the spinal canal causing malignant spinal cord compression (satisfaction of search). This was later picked up on a subsequent MRI following persistent right arm weakness and the spinal level was treated with radiotherapy.
References: NHS
Metastasis
Missed subtle bony spinal metastasis is one of the most common discrepancies that we have encountered.
Posterior elements and sacral disease can be easily missed at first glance and a dedicated survey should be incorporated.

Fig. 3: 74-year-old patient with history of localised bladder cancer without metastasis presented with right sciatic type pain. Review of previous CT showed a metastasis involving the right sacral posterior elements.
References: NHS

Fig. 4: Patient with history of breast cancer presented with lower back pain and cauda equina symptoms. MRI lumbar spine (A-T1W) showed a large malignant infiltrating area of abnormal signal in the lower sacrum. Review of MRI (B-T1W) performed 10 months before showed the same lesion to be much smaller and not causing any neural compromise.
References: NHS
P – Pulmonary embolism (and other vascular diseases)
Patients with malignancy are at an increased risk for vascular thrombosis and occlusion,
venous thromboembolism being the most common.
The increased risk is multi-factorial and includes carcinomatosis,
chemotherapy agents,
immobility,
co-morbidities,
post-surgical and altered anatomy.
Vascular thrombosis is commonly missed as it is usually subtle and there is often suboptimal vessel opacification.
Missed untreated pulmonary embolisms can propagate,
cause circulatory compromise or develop chronic thromboembolic pulmonary hypertension (CTEPH),
a factor associated with poor outcome.
Pulmonary embolism

Fig. 9: Pulmonary embolism (arrow) in a staging CT thorax of a 72-year-old male with oesophageal cancer which was not initially appreciated.
References: NHS
Deep vein thrombosis

Fig. 10: Left external iliac vein thrombosis post chemotherapy. Follow-up scan of a 59-years-old female patient with metastatic colorectal cancer and small volume peritoneal disease who had just completed chemotherapy in the FOCUS 4 trial.
References: NHS
Portal vein thrombosis

Fig. 11: Left portal vein thrombosis. 28-year-old male patient being treated for lymphoma presented with acute abdominal pain. The initial report by the night resident did not appreciate the left portal vein thrombosis (red ellipse). The right portal vein (green ellipse) and main portal vein were normal. Branch portal vein thrombosis is easily missed unless specifically looked for.
References: NHS
Splenic vein thrombosis

Fig. 12: Splenic vein thrombus (ellipse) and left atrial thrombus (arrows) in a 86-year-old patient with lung malignancy.
References: NHS
Venous sinus thrombosis

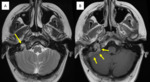
Fig. 7: Venous sinus thrombosis found on later review of imaging. This 50-year-old patient with known metastatic breast cancer presented with headaches and confusion. An MRI brain was performed to look for possible brain metastases; this was initially reported as normal. Review of imaging demonstrates, (A-T2 axial) lack of flow void (A - arrow) in the right jugular bulb and ( B-T1 post-contrast) a filling defect (B -arrows) in the right sigmoid sinus and right internal jugular vein consistent with venous sinus thrombosis.
References: NHS
Arterial occlusion
Arterial occlusion is uncommon but if present is easily missed unless specifically reviewed as most abdominal CT scans are performed in the portal venous phase.

Fig. 5: Aortic occlusion not appreciated on initial report. This 58-year-old male was on chemotherapy for rectal cancer and presented with vague abdominal pain. The sagittal CT in the portal venous phase shows complete occlusion (arrow) of the abdominal aorta (just distal to the SMA origin) – a recognised side effect of certain chemotherapeutic agents. The aortic occlusion was initially not reported but later picked up on review of the images.
References: NHS
O – Obstruction (or impending obstruction)
Gross luminal obstruction is easy to identify however it is imperative to look for early signs of obstruction or adjacent lesions which may lead to obstruction in the future due to invasion.
Urinary tract
Invasion of malignant lesions into the ureters can be anticipated if present on previous scans,
and the radiologist can preclude the patient presenting with acute obstruction needing emergency nephrostomies or stents.

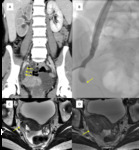
Fig. 6: Pelvic nodule causing ureteric obstruction. This 24-year-old patient with a history of surgically resected localised cervical cancer, presented acutely with right loin pain and sepsis. The coronal CT (A) shows an obstructed distal right ureter (arrow) due to an enhancing right pelvic mass, mild hydronephrosis and reduction in perfusion and corticomedullary differentiation of the right kidney. The patient urgently underwent a right nephrostomy and antegrade ureteric stent insertion (B), with nephroureterography demonstrating the malignant stricture (arrow). Review of the initial MRI pelvis 6 months earlier (C, axial T2) demonstrates an abnormal right pelvic nodule (arrow) which was missed at the time and a restaging MRI pelvis at the same level (D, axial T2) shows the nodule has significantly increased in size (arrow).
References: NHS
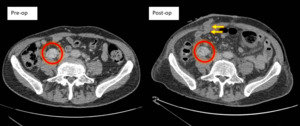
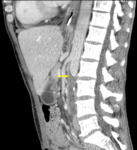
Fig. 13: Metastatic deposit adjacent to the right ureter. This 80-year-old patient had sigmoid colectomy and loop ileostomy (yellow arrows) for a T3 sigmoid carcinoma had a pre-op scan which did not appreciate the metastatic deposit (red circle) adjacent to the right ureter which may be an abnormal node or peritoneal disease. The post operative CT was done to look for an anastomotic leak. This patient would have likley presented in the near future with right ureteric obstruction.
References: NHS
Bowel
Colon cancer is common and a synchronous malignant lesion is often missed due to 'satisfaction of search' as the lesion may not be causing significant bowel obstruction.

Fig. 14: Sub-total obstruction with left colon cancer. Long segment of concentric left colon cancer causing sub-total obstruction not initially reported in a patient with an aggressive retroperitoneal lymphoma with left hydronephrosis.
References: NHS

Fig. 17: SMA syndrome causing duodenal obstruction. This 58-year-old patient with persistent weight loss which was initially attributed to his colonic cancer. Reviewing his CT abdomen (A-axial and B–oblique coronal) showed that the third part of the duodenum (red arrows) was obstructed between the Aorta (Ao) and the SMA (yellow arrow). In our experience, patients with sudden weight loss secondary to cancer can lose some retroperitoneal fat around the duodenum and in certain cases increase the risk of developing SMA syndrome.
References: NHS
Biliary tree
Periportal lymph nodes,
direct tumour invasion,
or subtle small cancers may obstruct the biliary tree.

Fig. 15: This subtle periampullary cancer (green arrows) lesion was not reported on this CT scan which was performed to investigate iron deficiency anaemia. The double duct sign - dilated common bile duct (red arrows) and pancreatic duct (yellow arrows) is present which is an important secondary sign.
References: NHS
Airway
Small endobronchial nodules which have not yet caused significant lung collapse are easily missed.

Fig. 16: Endobronchial nodule which subsequently caused segmental collapse. 58-year-old male presented with severe chest pain and a CT aorta (A and B) showed a type B dissection. A subsequent CT (C) showed left upper lobe segmental collapse (yellow arrows) secondary to an endobronchial lesion which was also present on the initial scan (B - red arrow). Histologically this was carconoid.
References: NHS

Fig. 19: Left main bronchus lesion not appreciated on initial report. The coronal CT images show abnormal soft tissue invading the left main bronchus, with the potential for luminal obstruction. This was subsequently proven to be a squamous cell carcinoma.
References: NHS
F – Fracture (pathological or impending)
The proximal femur and humerus should be carefully inspected for metastasis so save the patient from presenting with an acute pathological fracture.
Elective management includes embolisation and intramedullary nailing.
Proximal humerus

Fig. 18: Right proximal humeral metastasis which subsequently fractured. Patient with renal cell carcinoma presented with a proximal humeral fracture (B) following minimal trauma. Review of previous chest radiograph (A) performed 4 months earlier showed subtle cortical destruction (red arrows) which was not seen at the time.
References: NHS
Proximal femur

Fig. 8: Proximal femur metastasis at risk of fracture. This 60-year-old with a history of treated renal cell carcinoma presented acutely with right hip pain. Plain film (A) showed a large lytic lesion in the right proximal femur which is at high risk of fracture (A-arrow). CT of the abdomen and pelvis (B - coronal) and ( C- axial) performed four months earlier reported no recurrent malignancy, however, a small lytic lesion in the right proximal femur was present at that time (B and C arrow). The patient was subsequently managed with surgical nailing of the right femur.
References: NHS