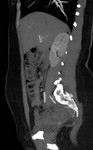
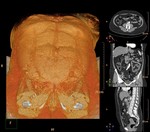
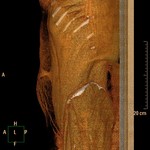
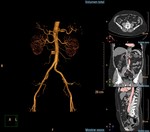
The evaluation of the perforating arteries can be done with different imaging techniques that can greatly improve the efficiency of the selection process,
being the most useful:
• Doppler ultrasonography (US),
is the most frequently used modality for vascular mapping,
but the results are mixed because most perforating arteries have a diameter of less than 15 mm,
the threshold for reliable visualization with US.
• A computed tomographic angiography (CTA) evaluation performed with the use of specific postprocessing and display techniques may be more accurate for identifying the most suitable vessel.
It is considered current gold standard.
• Magnetic resonance angiography (MRA) has the advantages of not ionizing radiation and allows the acquisition of arterial and venous images in a single examination,
but has the disadvantages of a longer exploration time and contraindications such as the implantable defibrillator,
bodies strange metallic and claustrophobic.
In our center we opted for CTA that allows excellent spatial resolution in a short time and it is more comfortable for the patient.
Is a technique able to characterize perforants with a sensitivity around 96-100% and a specificity of 95-100%.
1) Patient selection
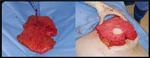
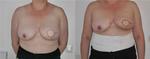
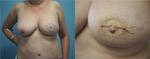
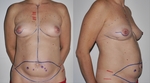
Most patients with breast cancer that have undergone a mastectomy are candidates for DIEP flap reconstruction.
This technique can also be used in patients with breast defects as well as in breast augmentation surgery.
The absolute contraindications for the DIEP flap are: previous abdominoplasty,
liposuction or active smoking.
Also exists relative contraindications like: presence of previous large cross-section or oblique incisions with DIEP pedicle affected.
If the patient is under radiotherapy,
it is preferable to be finished before surgery.
Of course,
for the realization of CTA is necessary that the patient don´t had nephropathy with a compromised renal function or allergy to intravenous iodinated contrast material.
2) Abdominal CTA
2.1 Image acquisition
Before the realization of CTA a creatinine measurement must be done,
the patient can´t eat at least 4 hours before the study and we must obtain a written informed consent.
The vascular study planning starts with:
• CT scanner helical of 64 detector rows (Philips Brilliance 64®).
• The patient,
with all undergarments removed,
is positioned supine on the CT table.
• 2 orthogonal topograms to locate the pubic symphysis in the anteroposterior plane and the umbilicus silhouette in the lateral one,
selecting the volume included between the inferior border of pubic symphysis and a horizontal line located five centimeters above the navel.
• Use of 120 kVp tube voltage and 180-200 mAs tube current,
results in high-quality images and acceptable effective dose estimates for the limited scanning range of abdominal wall CTA.
• Contiguous isometric acquisition data obtained with thin collimation helical are ideal for quality CTA.
• Administration of 150 ml of a contrast agent (Omnipaque 350®),
injected intravenously at a rate of 4 ml/sec.
• We employed the bolus tracking technique,
with the ROI (region of interest) in the abdominal aorta at the level of the L1 vertebra.
The exact time at which acquisition starts may be automatically programmed (over 100 U.H.) or manually.
• Images are acquired with a slice thickness of 2mm and an interval of 1mm reconstruction.
2.2 Postprocessing techniques
With the correct use of post-processing techniques we can obtain an exact location of the perforating arterial branches in all planes with descriptive information for the surgeon that provides the specific characteristics of each vessel.
The post-processing stage is carried out using work stations (Philips ®) to perform MPR,
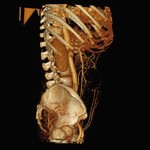
MIP and 3D,
with and without soft tissue removal.
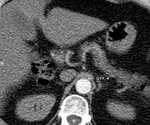
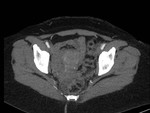
• We start with a global vision of the DIEA,
its course and its relations with the rectus abdominis muscle.
Also we studied the anastomosis with branches from the superficial inferior epigastric artery.
• After studying the relationships and general features,
we analyze the intrinsic characteristics of the perforating branches such as caliber,
numbers and course,
selecting and pointing the branches that show the most favourable characteristics,
in the axial,
MPR (multiplanar reconstruction) and 3D reconstructions.
• The MIP reconstruction (maximum intensity projection) can be used in an axial plane to study subcutaneous and intramuscular segments of the perforators.
• Then we measure the distance of the perforating arteries to the umbilicus.
It can be performed radial,
clockwise or measuring the distance at midline below the umbilicus and the lateral separation at this level.
With these post-processing techniques we can provide the simultaneous location of each perforator in the axial,
coronal and sagittal planes.
The radiology report should include findings relevant to the surgeon,
such as number,
location,
distance,
size,
and length of the bilateral perforating arteries,
with indication of the most favourable arteries.
Before the operation,
the surgeon marks the skin using the CTA references,
and then makes the incisions centered in the perforating artery that shows the best features.
3) Selection of favourable DIEP
The vessel selected depends on multiple anatomic and surgical considerations,
and the decision-making process can be exceptionally time-consuming,
in part because of the wide variation that occurs in vascular anatomy.
When setting out to evaluate the deep inferior epigastric perforating arteries,
the key anatomic variables to consider are the vessel size,
location (relative to the umbilicus),
course (intramuscular,
subcutaneous),
and length.
In cases in which the perforator shows long subfascial or intramuscular trajectories,
this must be indicated as both require a wide and careful dissection.
This is not a desirable procedure as it increases the morbidity of the abdominal wall.
Those perforators which origins coincide with a musculotendinous intersection are preferred by many surgeons as they usually present short or even absent intramuscular or subfascial segments.
Types I and II ramifications are more frequent and present shorter intramuscular trajectories than those originated from a type III pattern.
Considering that the rectus abdominis muscles are laterally innervated,
a more medial perforator is preferred because the surgical dissection is less likely to denerve the muscle.
Favorable characteristics are considered:
• Infraumbilical medial location.
• Caliber > 2 mm in MPR.
• Short distance < 3 cm.
• Less intramuscular trajectory.
• Low tortuosity.
• Branches types I and II.
Unfavorable characteristics are considered:
• Substantial subfascial segment.
• Long intramuscular segment.
• Tortuous intramuscular segment.
• Lateral course.
• Branches type III.
Selection of the most favourable perforator reduces the risk of intraoperative and postoperative complications,
reduces operating time avoiding unnecessary dissections.