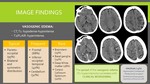
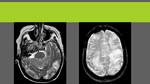
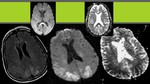
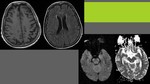
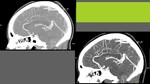
Hypoperfusion due to blood-brain barrier damage is demonstrated as vasogenic edema in MRI,
which is the main finding in PRES and can be demonstrated in morphologic sequences (as hypointense on T1 and hyperintense on T2-weighted).
On unenhanced CT it’s hypoattenuated but can be very subtle and confused with grey-White matter interface.
Fig. 8
Its distribution is variable,
but generally temporal and occipital lobes are affected in the subcortical white matter,
tipically in a bilateral and symmetric way.
Less frequent is involvement of frontal,
inferior occipital or temporal lobes,
and the cerebellum.
Affectation of other locations such as brainstem,
basal ganglia,
deep white matter or corpus callosum is rare; also there’s seldom partial or asymmetric affectation (<5%).
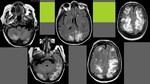
Images show typical case: bilateral,
symmetric,
hemispheric,
white matter affectation with vasogenic edema.
Fig. 9
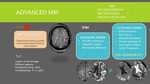
Apart from morphologic sequences,
MRI is useful to characterize PRES due to the ability to perform multiple advanced techniques: Fig. 10
T1+C (CONTRAST ENHANCEMENT) Fig. 11
Enhacement pattern is NOT USEFUL,
as it does not correlate with any variable (severity,
clinical history or any other).
There might be enhancement in up to 50% of the patients,
with different patterns (leptomeningeal,
cortical,
nodular or combinations of them).
May represent a brain-blood barrier ruptura or increase of permeability (due to endotelial disfunction).
Contrast should only be useful when distinguishing from other entities,
but is not useful in follow-up.
T2* (HAEMORRHAGES) Fig. 12
Normally there’s no bleeding,
but up to 15% of PRES show haemorrhages in different patterns (intraparenchymal,
SAH or microbleedings).
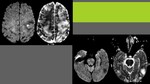
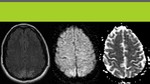
DWI
This is the most useful advanced sequence in setting of PRES,
because it allow differenciation of vasogenic and cytotoxic edema (which are not distinguishable on T2).
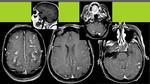
- Vasogenic edema: it’s the most common,
and,
as indicates increased permeability,
so there’s no real DWI restriction,
and we’ll obtain high ADC values (facilitated diffusion). Fig. 13
- Cytotoxic edema: indicates tisular damage and is represented as real restricted diffusion (hypointense on DWI).
ADC will be low (hypointense),
but in some cases or in early follow up it can pseudonormalize (isointense).
We have to now that cytotoxic edema indicates ischemia and may lead to stroke (25%),
and correlates with poorer prognosis,
but IT IS STILL REVERSIBLE.
We can have cytotoxic edema that resolve on follow-up. Fig. 14 Fig. 15 Fig. 16
ANGIOGRAPHY and ANGIO-CT Fig. 17
Usually there are signs of vasculopathy:
- Vasculary irregularity,
with string of pearls appearance (vasodilatation and vasoconstriction).
- Vasospasm-like lesions.
- Usually mild hypertension (<150 mmHg,
with no autoregulation failure).
PERFUSION
Although some authors described hyperperfusion,
according to new theory we should see hypoperfusion with CBF-CBV reduction,
without significant change in MTT.
Remember that it’s still reversible.
We should perform differential diagnosis with acute stroke in an emergency scenario. Fig. 18