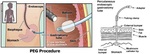
Percutaneous endoscopic gastrostomy (PEG) provides a possibility of long-term enteral feeding to patients with neurologic deficits,
swallowing disorders,
patology of upper gastrointestinal/respiratory tract (oropharyngeal or esophageal tumors) and various hypercatabolic states (burns,
short bowel syndrome,
major traumas).
There are actually two main indications – feeding access and gut decompression in patients with advanced abdominal malignancies causing chronic obstruction/ileus.
There are few contraindications to PEG placement.
Absolute contraindications include pharyngeal or esophageal obstruction,
active coagulopathy and any other general contraindication to endoscopy.
Relative contraindications are: the presence of oropharyngeal or esophageal cancer due to the potential seeding of the PEG tract with cancer cells,
abdominal wall abnormalities (the presence of prior abdominal surgery,
the presence of abdominal wall metastases,
open abdominal wounds,
or ventral hernia defects),
hepatomegaly,
splenomegaly,
moderate or severe ascites,
portal hypertension with gastric varices,
recent myocardial infarction,
hemodynamic instability and sepsis.
PEG was first introduced in 1980.
by Gauderer et al.
The procedure is considered to be simple,
safe and rapid.
The fiberoptic gastroscope is inserted through the patient´s mouth and advanced into the stomach.
Inflated air distends stomach and mobilizes the liver,
spleen and colon away from the gastrostomy site,
bringing the anterior gastric wall in close contact with the abdominal wall.
Then,
smoothly tapered intravenous cannula is introduced across the abdominal and gastric walls with a quick motion to pierce all the layers without pushing the stomach away.
A wire snare passed through the gastroscope is looped around the cannula after proper positioning has been assured.
With the plastic sheath in place,
the metallic needle is removed and a long silk thread is inserted.
The thread is grasped with the snare of the endoscope as it exits from the plastic cannula.
The string is brought out through the mouth together with the endoscope.
A specially prepared 16 French de Pezzer (Mushroom) catheter is lubricated and pulled in a retrograde fashion through the patient's mouth,
esophagus and across the gastric and abdominal walls.
Tension is applied on the catheter outside untile judged that the gastric and abdominal walls are in loose contact.
.
The catheter is anchored to the abdominal wall with 2 sutures of a strong synthetic material.
A cross bar of heavy rubber tubing aids in the immobilization.
The procedure has the advantages that general anesthesia is not usually required,
abdominal wall relaxation is not essential,
it can be done in patients with severe musculoskeletal deformities,
and there is minimal discomfort in the postoperative period.
The patients are observed for 24 hours and then fed.