The main non-osseous pathologies of the knee are explained by showing their correlation with the findings of the images.
Protocol MRI
The knee to explore is placed in the middle of the antenna in the extended position to optimize the study of the anterior cruciate ligament (ACL).
The typical parameters include a field of view of 14 -16cm,
and a section thickness of 3–4mm.
The sequences includes in our standard protocol are:
-
Saggital: T1 TSE (GE® / Phillips®)
-
Saggital: T1 SPIR (Phillips®) o FSE PD FS (GE®)
-
Coronal: PD SPIR (Phillips®) o FSE PD FS (GE®)
-
Axial: PD SPIR (Phillips®) o PD FS (GE®)
T1: T1 weighted images.
TSE: Turbo Spin-Echo.
SPIR: Spectral Presaturation with Inversion Recovery.
FSE: Fast Spin-Echo.
PD: Proton Density.
FS: Fat Saturation.
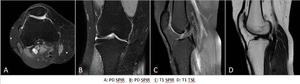
Fig. 1: Protocol MRI
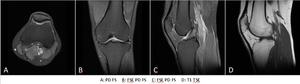
Fig. 2: Protocol MRI
Systematic reading
The knee is composed for multiple structures,
each with its own directional and spatial features.
The reading of MRI is better when these structures are analysed individually and with a particular order.
Our proposal for a systematic reading is:
1.
Meniscus.
2.
Ligaments.
3.
Bone.
4.
Articular space / soft tissue.
5.
Tendons.
6.
Second look.
More common image findings in knee MRI:
1. Menisci
The knee menisci are interposed between the articular surfaces of the distal femur and the proximal tibia.
Can be subdivided into the anterior horn,
body and posterior horn.
The medial meniscus (MM) is semilunar and larger than the more circular C-shaped lateral meniscus (LM).
On sagittal images,
the anterior and posterior horns of the LM are nearly equal in size,
whereas the posterior horn of the MM is nearly twice the size of the anterior horn.
On coronal images,
the menisci appear either triangular or wedge-shaped,
depending on whether the imaging plane is through the body or horn,
respectively.
1.1 Anatomic variants
• Discoid meniscus: It is an abnormally wide body and is seen in 3% -5% of the knees,
being most common in the lateral meniscus with a ratio of 10-20:1.
Is diagnosed when the body of the meniscus measures 15mm or more on a midline coronal image,
or in the sagittal plane,
the meniscus is seen with a continuous connection between the anterior and posterior horns,
in more than three consecutive images (usually,
the body of the LM is only seen on two adjacent sagittal slices).
Tears are more common with the complete discoid meniscus variant and often display horizontal or longitudinal tear patterns.
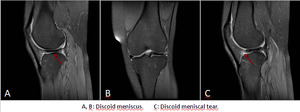
Fig. 3: Discoid meniscus
1.2 Pitfalls
Normal anatomic structures that can mimic a tear include the:
• Transverse meniscal ligament.
• Meniscofemoral ligaments.
• Popliteomeniscal fascicles.
• Oblique meniscomeniscal ligament.
1.3 Meniscal Tears
The prevalence of meniscal tears are associated with degenerative joint disease.
Are more common in the posterior horn of MM,
however,
in younger patients with an acute injury,
LM tears are more common.
Normal menisci have low signal intensity at MR imaging; however,
globular or linear increased intrameniscal signal intensity can be seen in children (because of normal vascularity),
in adults with internal mucinous degeneration,
and after trauma due to acute contusion.
Criteria for diagnosing a tear include:
- Meniscal distortion in the absence of prior surgery.
- Increased intrasubstance signal intensity unequivocally contacting the articular surface.
The findings must be identified in two coronal images,
two sagittal images,
or one coronal and one sagittal image.
In contrast,
the increase in intrasubstance signal intensity without extension to the articular surface is often not associated with a rupture in surgery and generally does not progress to a break.
• Basic shapes:
a) Horizontal Tear: It is the most common type.
It runs parallel to the tibial plateau and extends to the periphery,
dividing the meniscus into superior and inferior halves.
It usually occurs in patients older than 40 years without previous trauma and is more common in degenerative joint disease.
b) Longitudinal Tear: Run perpendicular to the tibial plateau and divide the meniscus into central and peripheral halves.
Often occur in younger patients after significant knee trauma and are more frequent in posterior horns.
The typical appearance is a vertically oriented line that contacts one or both articular surfaces.
c) Radial Tear: Extends from the inner free edge of the meniscus and runs perpendicular to the long axis of the meniscus.
Commonly involve the posterior horn of the MM or the junction of the anterior horn and body of the LM.
On axial MR images,
these tears appear as clefts oriented perpendicular to the free edge.
d) Complex Tear: includes a combination of radial,
horizontal,
and longitudinal components (any two or all three).
It is generally defined as unstable.
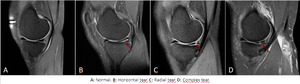
Fig. 4: Meniscal tears
• Displaced shapes:
a) Bucket-Handle Tear (displaced longitudinal tear):is a longitudinal tear with central migration of the inner “handle” fragment.
Occurs seven times more frequently in the MM and has at least five different MR imaging signs:
- Absent bow tie.
- Fragment within the intercondylar notch.
- Double PCL.
- Double anterior horn or flipped meniscus.
- Disproportionally small posterior horn.
It is defined as unstable.
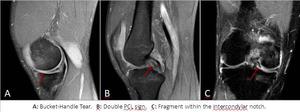
Fig. 5: Bucket-Handle Tear
b) Flap tear (displaced horizontal tear).
c) Parrot beak (displaced radial tear).
1.4 Indirect Signs of Meniscal Tear
These signs are MRI findings that can accompany meniscal tears.
• Parameniscal Cyst: represent the peripheral escape of joint fluid through a meniscal tear,
which typically contains a horizontal component.
Lateral meniscal cysts are more common.
Most meniscal cysts contain septations and present a lobulated appearance.
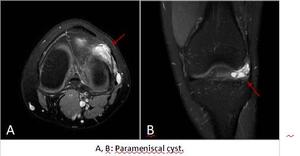
Fig. 6: Parameniscal Cyst
• Meniscal Extrusion: It is present when the peripheral margin of the meniscus extends 3mm or more beyond the edge of the tibial plateau.
• Subchondral Marrow Edema: Linear subchondral bone marrow edema is a superficial edema that is adjacent to the meniscal attachment site,
parallels the articular surface,
and is less than 5mm deep.
2.
Ligaments
2.1 Anterior Cruciate Ligament (ACL)
It is the frequently injured knee ligament.
Originates from posterior medial surface of the lateral femoral condyle and runs parallel to the roof of the intercondylar notch and inserts on medial and anterior aspect of the tibial plateau.
Forms an approximately 45º angle to the long axis of the tibia and has a straight inferior margin.
Intact ACL has hypointense signal on all MR sequences but may contain some high signal within it,
especially at its insertion on the tibia,
also it may contain high signal if there is mucoid degeneration within it.
Most ACL tears involve the middle substance of the ligament (90%).
Specific signs of ACL injury include:
-
Irregular contour,
discontinuity,
focal or diffusely increased intrasubstance signal intensity,
or poor visualization.
-
T2-weighted MRI allow high-signal-intensity joint fluid to be distinguished from a normal ligament.
Areas of interstitial edema or haemorrhage are also manifested as increased signal intensity.
-
A sprain or partial tear of the ACL is mentioned when some fibers are intact and focal or diffuse high signal or laxity of the ACL is present.
However caution should be exercised in reporting partial tear of ACL,
and mucoid degeneration should be excluded.
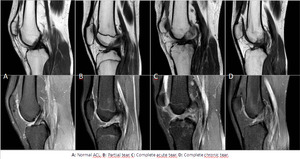
Fig. 7: Anterior Cruciate Ligament
2.2 Posterior Cruciate ligament (PCL)
Originates from the anterolateral aspect of the medial femoral condyle and inserts over the back of tibial plateau.
It is much thicker than ACL,
being a complete interruption of the LCP less common and associated with severe injuries.
On MRI the normal PCL appears as a well-defined band of very low signal intensity that courses between the medial femoral condyle and the posterior tibia.
PCL rupture is easily identified and we can see this signs:
-
Failure to identify the PCL.
-
Amorphous high signal intensity in the region of the PCL on T1 and T2-weighted images without definable ligamentous fibers.
-
Visualization of PCL fibers with focal discrete disruption of all visible fibbers.
A partial tear or intrasubstance injury are much more common and manifest as T2 or STIR intra substance hyperintensity with often laxity and thickening of the ligament,
or has some fibers that appear intact and some that appear discontinuous.
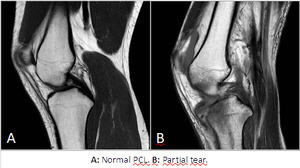
Fig. 8: Posterior Cruciate Ligament
2.3 Medial collateral ligament (MCL)
Originates on the medial aspect of the distal femur and inserts on medial aspect of the proximal tibia.
Three grades of MCL injury have been described:
-
Grade 1: is a sprain with high signal in the soft tissues medial to the MCL.
-
Grade 2: a severe sprain or partial tear,
with high signal in the soft tissues medial to the MCL with partial disruption of the MCL.
-
Grade 3: complete tear,
shows disruption of the MCL and disruption of medial patellar retinaculum.
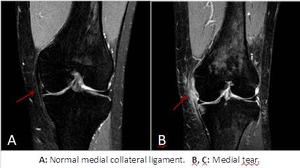
Fig. 9: Medial collateral ligament
2.4 Lateral collateral ligaments (LCL)
Originates from external tuberosity of the lateral condyle of femur anterior to the origin lateral head of the gastrocnemius muscle.
Periligamentous soft tissue edema is often present in all injuries range from partial intra substance tear to complete disruption and avulsion from bony attachment from fibular head.
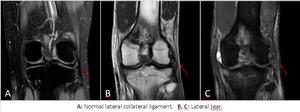
Fig. 10: Lateral collateral ligaments
3. Extensor mechanism
3.1 Quadriceps tendon
Most ruptures occur at the tendon-osseous junction at the superior pole of the patella.
Other potential areas of rupture include the muscle belly,
the musculotendinous junction,
and the tendon itself.
Transection of all layers is diagnostic of a complete tendon rupture and may be associated with a mass of edematous tissue and haemorrhage that manifests as an area of increased signal intensity on T2- weighted images.
The position of the patella may be a helpful secondary finding.
3.2 Patellar tendon
It is a less common cause of extensor mechanism dysfunction.
The absence of distinct margins and increased signal intensity on T2-weighted images within the tendon,
allow confirmation of acute inflammation.
Haemorrhage and edema may extend to the region of the Hoffa fat pad.
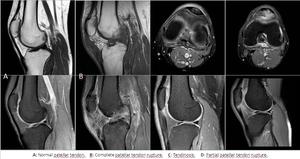
Fig. 11: Patellar tendon
3.3 Patella
Chondromalacia patellae refers to softening and degeneration of the articular hyaline cartilage of the patella.
Tends to occur in young adults and there is a recognised female predilection.
This is the classification of patellar cartilage for the diagnosis:
-
Grade 1: areas of signal increase in the cartilage,
but with intact architecture (smooth surface).
-
Grade 2: superficial partial or focal defects involving less than 50% of cartilage thickness.
-
Grade 3: deep partial-thickness defects involving more than 50% of cartilage,
without bone edema.
-
Grade 4: full-thickness cartilage defect with associated bone marrow edema.
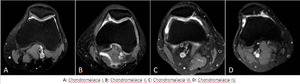
Fig. 12: Chondromalacia
3.4 Suprapatellar and infrapatellar fat pad
There are several well-defined fat pads within the knee joint,
interposed between the joint capsule and the joint cavity with synovial lining,
and therefore intracapsular but extrasinovial.
The three anterior fat pads include:
- Anterior suprapatellar (quadriceps).
- Posterior suprapatellar (prefemoral or supratrochlear).
- Infrapatellar (Hoffa).
The infrapatellar fat pad of Hoffa is bordered by the inferior pole of the patella (superiorly),
the joint capsule and patellar tendon (anteriorly),
the proximal tibia and deep infrapatellar bursa (inferiorly),
and the synovium-lined joint cavity (posteriorly).
The transverse (geniculate) ligament courses within the posterior aspect of the fat pad.
• Hoffa disease: is a syndrome of impingement.
Acute or repetitive trauma causes hemorrhage.
The inflamed fat pad then becomes hypertrophied,
which predisposes it to crushing or impingement between the femur and tibia and to further injury and inflammation.
Fat pad impingement may also occur in the absence of prior injury (Hoffa syndrome).
Acute edema and hemorrhage manifest as areas of increased signal intensity on T2-weighted MRI.
In the subacute and chronic phases,
fibrin and hemosiderin have low signal intensity on both T1 and T2-weighted MRI.
Also,
this fat pad may be involved secondarily from extrinsic processes,
including: articular disorders,
synovial abnormalities and anterior extracapsular abnormalities.
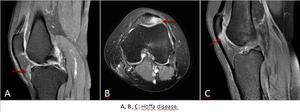
Fig. 13: Hoffa disease
4. Bursae
Bursae around the knee are numerous and act to reduce friction between adjacent moving structures.
They are synovium-lined structures,
usually collapsed but often containing a small amount of synovial fluid.
Inflammation from local and systemic processes (overuse,
trauma,
infection,
haemorrhage,
internal joint derangement,
inflammatory arthropathy,
and collagen vascular disease),
may cause thickening of the synovial lining and accumulation of fluid within the bursa,
allowing visualization on MRI.
On MRI,
bursae appear as fluid collections with low signal on T1-weighted images and high signal on T2-weighted images.
In chronic cases,
the signal may be heterogeneous,
and complicated by haemorrhage and calcification.
4.1 Popliteal (Baker's) cysts
Popliteal cysts are not true cysts and represent the semimembranosus-medial gastrocnemius bursa.
They are the most frequently encountered cystic masses around the knee.
Their incidence on MRI reported in the literature ranges from 4.7% to 19%.
They are formed by a communication between the posterior joint capsule and gastrocnemius-semimembranosus bursa.
Increased intra-articular pressure due to joint effusion or other factors (meniscal tears or degenerative joint disease) causes the extravasation of joint fluid through the posteromedial joint capsule between the medial head of the gastrocnemius and the semimembranosus tendon into the gastrocnemius-semimembranosus bursa.
Popliteal cysts have been associated with various intra-articular disorders such as inflammatory and degenerative arthritis,
meniscal or ACL tears,
infectious arthritis,
lymphoma,
and sarcoidosis.
4.2 Suprapatellar bursitis
It is located between the quadriceps tendon and the femur.
It normally communicates with the synovial cavity of the knee but may be isolated if the suprapatellar plica fails to involute (the suprapatellar plica is a normal embryonic septum between the bursa and the joint that usually perforates and involutes; it is present in approximately 20% of adult knees).
4.3 Prepatellar bursitis
It is located anteriorly between the patella and the subcutaneous tissues adjacent to the proximal patellar tendon.
4.4 Superficial infrapatellar bursitis
It is located between the tibial tubercle and the overlying skin.
4.5 Deep infrapatellar bursitis
It is located between the posterior margin of the distal patellar tendon and the proximal tibia,
beneath Hoffa's fat pad.
4.6 Anserine bursitis
It is located along the medial aspect of the tibia separating the pes anserinus from the tibial insertion of the medial collateral ligament and the bony surface of the medial tibial condyle.
4.7 Medial collateral ligament bursitis
It is located along the middle third of the medial aspect of the knee between the superficial and deep layers of the MCL.
4.8 Semimembranosus-medial collateral ligament bursitis
It is located between the semimembranosus tendon and the MCL.
4.9 Iliotibial bursitis
It is located between the distal part of the iliotibial band and the adjacent tibial surface.
4.10 Lateral collateral ligament-biceps femoris bursitis
It is located superficially to the distal lateral collateral ligament and deep in the anterior arm of the long head of the biceps femoris muscle as it crosses the LCL.
5. Cystic lesions
Most cystic lesions around the knee represent encapsulated fluid collections and exhibit low signal intensity on T1-weighted images and high signal intensity on T2-weighted images.
5.1 Ganglion Cyst
Arise from the joint capsule,
ligaments,
bursae,
tendon sheaths,
or subchondral bone,
perhaps from synovial herniation or tissue degeneration.
They usually are associated with the cruciate ligaments and may be multiocular or lobulated.
Are not associated with meniscal tears.
5.2 Subchondral cysts (geode)
Often associated with osteoarthritis.
On MRI,
are multiple,
segmental in distribution,
and present with surrounding sclerosis.
An adjacent abnormal joint is usually associated.
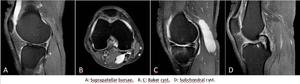
Fig. 14: Bursae and Cysts















