Pulmonary venous and arterial tumors must be distinguished from other pulmonary vascular pathology,
and can be aided by the use of Dual Energy and Spectral CT.
Here we review imaging findings of pulmonary arterial and venous tumors:
Primary benign pulmonary arterial tumor
Papillary fibroelastomas are benign tumors that arise from cardiac valves.
These lesions can be complicated by pulmonary or systemic embolization depending on the primary site.
Treatment of these lesions depend on size,
associated comorbidities and symptoms.
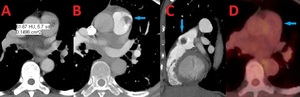
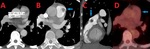
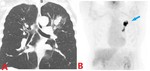
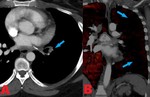
Fig. 1: 67 yo F with a pulmonary artery mass found to be a benign papillary fibroelastoma. (A-B). Contrast enhanced computed tomography (CT) axial image shows a hypodense 1.4 x 1 cm pulmonary arterial mass. (C). Contrast enhanced computed tomography (CT) sagittal image shows this hypodense lesion just distal to the pulmonic valve. (D). Axial image from FDG PET scan shows that the pulmonary artery mass is not significantly FDG avid.
Primary malignant pulmonary venous tumor
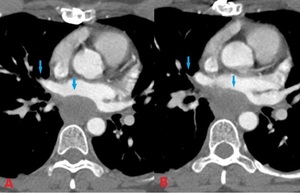
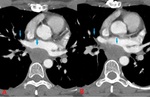
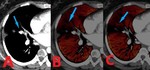
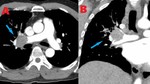
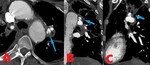
Fig. 2: 39 yo F with spindle cell sarcoma of the right superior pulmonary vein and left atrium. Contrast enhanced computed tomography (CT). (A). Axial image shows a 3.6cm transverse x 2.4 cm anteroposterior x 4 cm craniocaudad mass involving the right superior pulmonary vein and left atrium. (B). Axial image at a slightly lower level shows further extension of filling defect involving the right superior pulmonary vein (blue arrows).
Primary lung cancer with local invasion
Lung cancer is the second most common cancer in men and women,
and is the leading cause of cancer death. Lung cancers are the most common primary tumors to involve the pulmonary vasculature,
seen in up to 77-87% of resected lesions[3].
Most of these represent microscopic invasion,
with fewer cases of gross invasion.
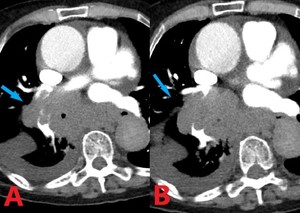
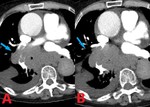
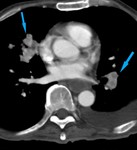
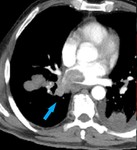
Fig. 3: 71 yo F with metastatic small cell lung cancer and invasion into right lower lobe branch pulmonary artery. Contrast enhanced computed tomography (CT). (A). Axial image demonstrates local invasion into the right lower lobe branch pulmonary artery (blue arrow). (B). Axial image at slightly lower level shows encasement and invasion into the branching pulmonary artery by the primary tumor.
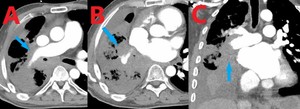
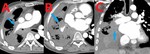
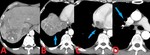
Fig. 4: 61 yo M with primary adenocarcinoma of the lung with invasion of the right middle and lower pulmonary arteries. Contrast enhanced computed tomography (CT). (A) Axial image demonstrates encasement and invasion of the right pulmonary artery. (B) Axial image at a slightly lower level shows further involvement of the right pulmonary artery branches. (C). Coronal image reveals local spread of primary adenocarcinoma into the right pulmonary arterial vasculature.
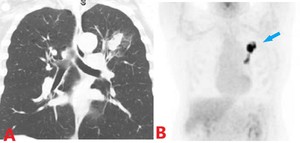
Fig. 5: 66 yo M with recent diagnosis of LUL mass, previously treated for pneumonia. (A) Coronal contrast enhanced CT image and (B) Coronal MIP from PET scan showing pulmonary venous extension of a LUL lung mass. Histopathology confirmed high grade sarcomatoid (spindle cell) carcinoma with necrosis and invasion into the pulmonary venous vasculature.
Pulmonary arterial tumor emboli
Pulmonary emboli are common imaging findings in patients with known malignancy. The relative risk of venous thromboembolic disease is seven times higher in patients with cancer,
as there is a significant association between malignancy and hypercoagulability [7]. Therefore,
pulmonary emboli from a bland thrombus is commonly seen,
and must be differentiated from a pulmonary embolus secondary to tumor emboli.
This distinction is critical for proper management. Differentiation through imaging is especially important as the clincial presentation of these tumors is identifical of that of a bland thrombus.
Patients often present with chest pain,
shortness of breath,
cough,
and depending on tumor size can present with cardiovascular instability[8].
Though any primary cancer may cause tumor emboli, examples of metastatic osteosarcoma,
hepatocellular carcinoma and renal cell carcinoma are described below.
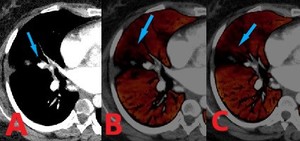
Fig. 6: 32 yo F with chest pain in patient with metastatic osteosarcoma. (A). Axial CT soft tissue window of the mid-lower lung shows cutoff of the lateral segmental bronchus of the right middle lobe and adjacent lateral subsegmental pulmonary artery branch from osteosarcoma metastasis (arrow) along with mucous/debris. (B and C). Corresponding section lung perfusion images from dual energy CT data reveal right middle lobe lateral subsegmental parenchymal perfusion defect (arrows).
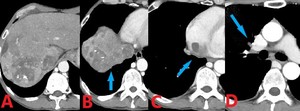
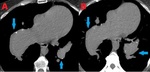
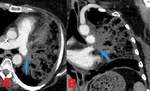
Fig. 7: 52 year old male with metastatic hepatocellular carcinoma invading the IVC and embolus to the right pulmonary artery. Contrast enhanced computed tomography (CT). (A-B). Axial images through the liver demonstrate a heterogeneously enhancing mass, consistent with known hepatocellular carcinoma. (C). Axial image reveals tumor invading the IVC at the junction of the right atrium. (D). Axial image shows a filling defect in the right pulmonary artery, representing a tumor embolus.
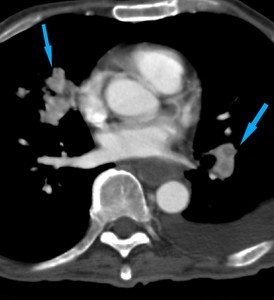
Fig. 8: 63 year old male with metastatic renal cell carcinoma. Contrast enhanced axial computed tomography (CT) image shows nodular heterogenoulsy enhancing serpiginous opacities within the bilateral pulmonary arterial vasculature consistent with endovascular RCC tumor emboli.
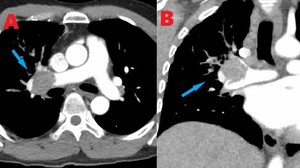
Fig. 9: 67 yo M with metastatic renal cell carcinoma and tumor emboli in the right pulmonary artery. Contrast enhanced computed tomography (CT). (A). Axial image shows tumor emboli in the distal right pulmonary artery. (B). Coronal image further demonstrates this finding with a filling defect seen in the right pulmonary artery.
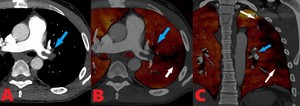
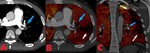
Fig. 10: 35 yo M with metastatic renal cell carcinoma with tumor emboli to the left pulmonary artery and distal perfusion defects. (A). Contrast enhanced axial computed tomography (CT) image shows tumor emboli in the left pulmonary artery. (B). Lung perfusion axial image acquired from Dual Energy scanner shows tumor emboli in the left pulmonary artery (blue arrow) and peripheral perfusion defect (white arrow). (C). Lung perfusion coronal image shows tumor embolus (blue arrow) and extensive peripheral perfusion defect (white arrows).
Pulmonary Venous Invasion
Metastatic disease to the lungs can lead to direct invasion into the pulmonary venous vasculature,
and occasionally invasion of the left atrium.
Identification and proper management of such lesions are important as this can lead to systemic tumor emboli.
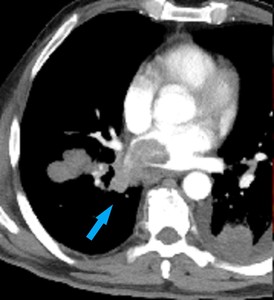
Fig. 11: 57 year old male with metastatic melanoma infiltrating right inferior pulmonary vein. Contrast enhanced axial computed tomography (CT) image demonstrates a filling defect and spread in the right inferior pulmonary vein (arrow).
Tumor Mimickers
Partial or complete filling defects within the pulmonary vasculature are not always secondary to bland thromboembolic disease or tumor emboli.
Several etiologies must remain in the differential for pulmonary tumor emboli such as aneurysms,
arteriovenous malformation,
infectious lesions and cement emboli.
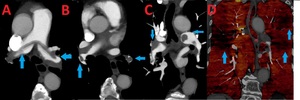
Fig. 12: 83 yo F with extensive bilateral pulmonary emboli including a saddle embolus. (A). Contrast enhanced computed tomography (CT) axial image shows a homogenous hypodense filling defect spanning the bifurcation of the pulmonary artery consistent with a saddle embolus. (B). Contrast enhanced computed tomography (CT) axial image shows thrombotic emboli into the branching pulmonary arteries. (C). Contrast enhanced computed tomography (CT) coronal image demonstrates hypodense emboli in the right and left pulmonary arteries (arrows). (D). Coronal lung perfusion image shows areas of decreased perfusion secondary to pulmonary emboli.
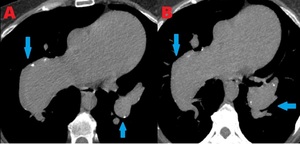
Fig. 13: 55 yo M with dilated pulmonary arteries secondary to chronic emboli. Contrast enhanced computed tomography (CT). (A-B). Axial MIP and soft tissue window images reveal marked dilated main, right and left central pulmonary arteries secondary to eccentric chronic thrombus in right pulmonary artery. Patchy bilateral pulmonary artery wall calcifications are seen due to pulmonary artery hypertension.
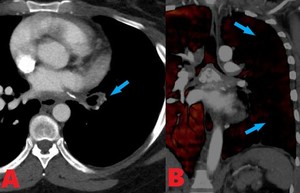
Fig. 14: 39 yo F with fibrosing mediastinitis. (A). Contrast enhanced computed tomography (CT) axial image shows marked attenuation of the left lower lobe pulmonary arteries. (B). Lung perfusion coronal image shows perfusion defects in the peripheral left lung (blue arrows), secondary to fibrosing mediastinitis.
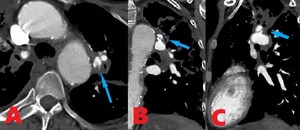
Fig. 15: 54 yo M with a pseudoaneurysm of the left main pulmonary artery. Contrast enhanced computed tomography (A). Axial image shows a pseudoaneurysm arising from the superior margin of the left main pulmonary artery sitting adjacent and medial to the apicoposterior pulmonary arteries feeding the left upper lobe. (B-C). Coronal images showing a pseudoaneurysm of the left main pulmonary artery.
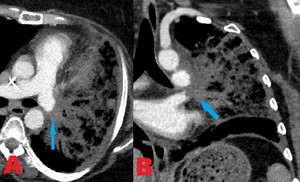
Fig. 16: 30 yo F with invasive rhizopus infection. Contrast enhanced computed tomography (CT). (A) Axial and (B) coronal images show filling defects and abrupt cut off of the left main pulmonary artery without opacification distally secondary to mucormycosis.
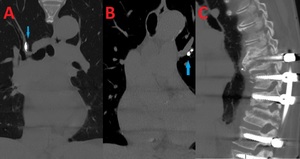
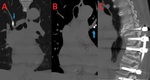
Fig. 17: 77 yo F with cement pulmonary emboli secondary to multiple prior surgeries including posterior spinal fusion from T9 through S2. Computed tomography (CT) images. (A-B). Coronal images show hyperdense lesions in the right (A) and left (B) branching pulmonary arteries representing embolized cement. (C). Sagittal image shows evidence of prior spinal surgery.
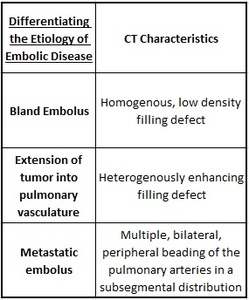
Table 1