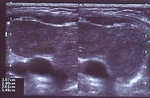
1st- We refused x-ray examinations for thymus hyperplasia (Fig.2) used previously as the standard (more than 600 each year) and limited the number of multiple x-ray follow-up examinations (more than 700 each year).
2nd- We widely used ultrasound for emergency (about 3000 procedures each year).
Ultrasound also used in the operation room during neurosurgery.
Intraoperative navigated neuro ultrasound in elective and urgent infant,
and pediatric neurosurgery was performed for patients from one month to twelve years old with sector & linear probes,
CD & PD.
It used in the different steps: after craniotomy,
before cortex incision,
during needle insertion,
before and after abscess removal,
after abscess drainage and hemostasis.
Ultrasound practiced on the different times after abscess drainage during the surgery,
and different days after neurosurgery for the follow-up.
Elective and urgent infants and pediatric intraoperative navigated neuro ultrasound allow to: implement the precise needle insertion,
puncture,
and drainage,
update the site and the size of the skull trephine zone,
control the area of dissection of the cerebral cortex,
minimize the trauma of normal brain structures,
monitor the abscess removal or drainage,
reduce the total time of the surgery,
improve the patient’s recovery.
We used ultrasound also in thoracic surgery,
as guidance for precise FNA of mediastinal lesions,
soft tissue masses or fluid collection (more than 300 procedures a year),
follow up after brain,
head,
and neck,
thoracic and abdominal surgery (more than 1500 procedures a year).
We performed ultrasound-guided mediastinum mass biopsies under general anesthesia with 5-7 MHz linear probes,
real-time gray scale ultrasound.
Color Doppler and Power Doppler permitted us to avoid vessels trauma in the mass and the nearby structures of the anterior mediastinum.
We used 22-25 Gauge needles for performing FNA.
In all cases,
we have had sufficient materials for qualify cytological analysis.
We did not have any complication including emphysema,
infection,
and bleeding after ultrasound-guided mediastinal mass biopsies.
The method permitted us to avoid big vessels trauma in the mass and the nearby structures of the mediastinum.
There were no hospitalization needs for outpatients.
The meddle duration of the procedures ranges from 35 to 120 minutes.
We performed ultrasound-guided FNA after careful patient’s selections.
Direct ultrasound visualization of the thorax masses was obligate for choosing children undergoing FNA using general or local anesthesia.
We did not have any complication after thorax masses ultrasound-guided fine needle aspiration.
Children with destructive pneumonia underwent the ultrasound many times: at the beginning of their admission,
during the treatment (including fine needle aspiration for fluid evacuation,
drainage,
bacterial analysis),
and multiple follow-ups.
Application of ultrasound examination in children thorax pathology practice with its other benefits can minimize additional children radiation.
In some cases,
(a hiatal hernia,
polyps - about 100 procedures a year),
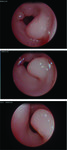
we used endoscopy instead of barium contrast x-ray (Fig.3).
MRI was used in some brain and trauma pathology instead of CT scan or for the follow-up.
3rd- In the hospital,
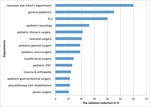
we changed conventional x-ray machines to digital x-ray machines and implemented the last generation of low doses CT-scan for the pediatric practice.
Such an approach allows decreasing children radiation in the different departments of the pediatric hospital (Fig.4).