We want to demonstrate through clinical cases that many of the hepatic subcapsular collections come from a problem in the pancreatic duct,
bile duct/gallbladder and gastro-duodenal region.
Inflammatory/infectious conditions (figures 4,
5,
6,
7,
8,
9,
10)
A wide spectrum of infectious and inflammatory diseases may involve the hepatic capsular and subcapsular regions by way of peritoneal,
hematogenous,
biliary and perihepatic ligamentous routes.
Although the liver capsule is not visible at CT,
it becomes visible in the presence of liver disease (1).
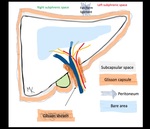
The gallbladder is closely apposed to the liver within the fossa.
Indeed,
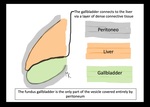
the liver's serosal covering (visceral peritoneum) extends over and completely covers the free surface of the gallbladder (fundus) and it connects to the liver via a layer of dense connective tissue (figure 4) (2).
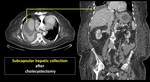
Cholecystitis is a frequent entity that does not often lead to subcapsular collections as in our cases (figure 5,
6,
7).
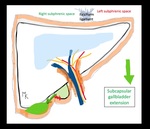
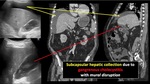
The vesicular bed itself is not covered with peritoneum but the free fundus gallbladder surface is,
so that any process that affects its mural integrity can be manifested through subcapsular collections as in the cases shown.
There are some inflammatory conditions where perihepatic abnormal findings (not specifically subcapsular findings) may be found,
like in Fitz-Hugh-Curtis syndrome (figure 8) and in a gastro-duodenal perforation (figure 9).
In the 1930s,
both Curtis and Fitz-Hugh described a syndrome characterized by right-sided abdominal pain and perihepatitis associated with pelvic inflammatory disease like in our case.
The CT can shows gallbladder wall thickening,
pericholecystic inflammation,
and transient hepatic perfusion anomalies in the context of pelvic inflammatory disease (6).
In the gastro-duodenal perforation air in the hepato-duodenal ligament is a finding that must make us think of perforation in this location (7).
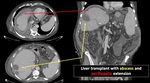
The last case shown in this section is a patient with a recent liver transplant patient with intrahepatic abscesses that show subcapsular extension (figure 10).
Traumatic injury (figures 11,
12,
13,
14,
15,
16)
Likewise,
a traumatic injury to the bile duct may lead to this type of collection since the extension route is the same in all cases.
Bile traumatic lesions,
subcapsular haematoma due to broken hepatocarcinoma and surgical pancreatic complications are shown in our cases.
Not always a subcapsular collection is a biloma (figure 10).
The pancreas is an organ often involved in this type of collections.
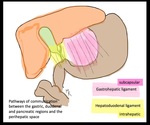
For hepatic extension of pseudocysts two basic patho-physiological mechanisms have been postulated (figure 2): the first is the accumulation of the pancreatic juices in the pre-renal space which erodes through the posterior layer of the parietal peritoneum into the lesser sac.
The collection from the lesser sac then tracks along the lesser omentum or gastrohepatic ligament toward the liver,
leading to subcapsular collection in the left lobe.
In the second mechanism the pancreatic juice tracks along the hepato-duodenal ligament from the head of the pancreas to the porta hepatis resulting in the formation of intra-parenchymal collections.
Both these collections have distinctive imaging characteristics; subcapsular pseudocysts are biconvex in shape and intra-parenchymal pseudocysts are located away from the liver capsule and are located near the porta hepatis branches (8).
Infiltrative-Neoplasic (figure 2,
17,
18)
The part of the Glisson capsule that surrounds the intrahepatic portion of the hepatic portal system is called the Glisson sheath (figure 1).
The Glisson capsule or sheath continues into the subperitoneal space of the gastrohepatic and hepatoduodenal ligaments (figure 2).
Infiltration by benign or malignant tumors or chronic inflammatory lesions can extend along the subperitoneum and progressively invade the subcapsular region of the liver (1).
Metastatic diseases (figure 17,
18) of the liver can occur at the capsular and subcapsular regions from seeded metastasis,
invasion via the perihepatic ligaments,
and direct invasion by malignancy from an adjacent organ.
These metastatic lesions are usually much less well defined than are true parenchymal metastases and are not surrounded by liver parenchyma (1).