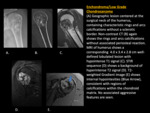
Enchondroma
Enchondroma is a common benign medullary cartilaginous neoplasm.
These benign lesions are most frequently incidental findings and diagnosed in childhood to early adulthood with a peak incidence at 10 to 30 years.
They account for 3-10% of all bone tumor and 12-24% of benign bone lesions.
Enchondromas can occur in any bone formed from cartilage and are typically located centrally within the medullary cavity of tubular bones,
such as bones of hands and feet,
femur,
tibia and humerus. They arise from the chondrocytes in the growth plate cartilage,
thus the majority of arise in the metaphyseal region.
Enchondromas are usually small lytic lesions <3 cm with well-defined scalloped margins and mild endosteal scalloping.
The phalanges are the only locations where enchondromas do not contain calcified chondroid matrix and appear expansile and purely lytic.
In other locations,
enchondromas have the “rings and arcs” calcification typical of chondroid matrix.
Multiple enchondromas are associated with Ollier Disease and Maffucci Syndrome.
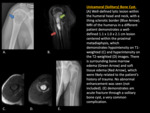
Unicameral Bone Cyst
Unicameral bone cysts,
also called simple bone cysts or solitary bone cysts,
are common benign neoplastic lesions that are always central in location.
Unicameral bone cysts occur usually in young patients in the first and second decade of life; and are more common in male with a M:F ration of 2-3:1.
These defects begin at the physeal plate in long bones and are filled with a serous fluid.
The defects eventually grow into the diaphysis and expand and thin out the overlying bone.
Approximately two thirds to three fourths of unicameral bone cysts occur in the proximal humerus and proximal femur.
These lucent lesions can occur in the calcaneus,
where there have atypical location adjacent to the inferior surface of the calcaneus.
Unicameral bone cysts are characterized as a well-defined lytic lesion with a narrow zone of transition,
a central location,
and no periosteal reaction or soft tissue component.
A fallen fragment sign is when a fragment of the fractured cortical bone is seen in the dependent portion of the lesion.
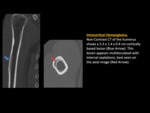
Intercortical Hemangioma
Intracortical hemangiomas are extremely rare,
accounting for <1% of all primary bone lesions,
with a female predilection.
Intracortical hemangiomas are often comprised of capillaries,
arteriovenous,
or cavernous hemangioma located without an associated soft tissue mass.
They are usually documented to occur in long bones such as femur,
tibia and humerus,
while other locations such as ribs and mandibles have been reported.
Radiographically,
intracortical hemangiomas are characterized as small well-defined osteolytic lesion that may be associated with cortical thickening,
sclerosis or periostitis.
Furthermore,
there have been cases of intracortical hemangiomas associated with internal lattice-like trabeculae and/or vertically oriented striations.
Osteoid Osteoma
Osteoid osteomas are benign bone-forming tumors that occur mainly in males ranging in age from 7 to 25.
Classically,
the pain is worse at night and resolves with aspirin or other salicylates.
The tumor is characterized by a small radiolucent nidus that is usually less than 1.5 cm in diameter and accounts for approximately 12% of benign bone tumors.
Any bone may be involved,
but they are most commonly found in the shaft of long bones in the femur and tibia.
They can also be found in the phalanges and the vertebra.
The lesions are usually cortical,
but can be subperiosteal,
intramedullary,
or intracapsular.
On imaging,
there is an intracortical nidus with variable amounts of mineralization,
cortical thickening,
and reactive sclerosis surrounding the nidus.
The “double density” sign is a highly specific finding that can be seen on nuclear imaging.
It shows intense activity at the nidus surrounded by less activity of the reactive bone.
The tumor typically resolves on its own over the course of several years,
but the nidus may be removed if pain cannot be managed.
Incomplete removal may lead to recurrence of the tumor.
Langerhans Cell Histiocytosis/Eosinophilic Granuloma
Eosinophilic granuloma is the most common manifestation of Langerhans cell histiocytosis in the skeletal system.
Eosinophilc granulomas occurs almost exclusively in children and adults younger than 30 years with a male predilection 2:1.
These lesions are formed from medullary bone resorption due to the granulomatous proliferation of Langerhans cells,
along with eosinophils,
neutrophils and lymphocytes.
The most common locations are the skull,
pelvis and long bones,
while the most common location in adults is the ribs.
Radiographically,
eosinophilic granulomas have many appearances.
In the skull,
they can appear as a single or multiple lytic lesions without sclerotic rim.
They are can manifest as a well-defined lytic lesion in the pelvis.
Moreover,
eosinophilic granulomas can involve the diaphysis and metadiaphysis in long bones,
may elicit a periosteal response,
and could be associated with a soft tissue mass. The majority of eosinophilic granulomas spontaneously resolve and become fibrotic within one to two years.
Other treatment options include excision,
radiofrequency ablation,
and steroid injections.
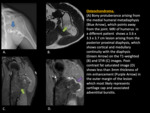
Osteochondroma
Osteochondromas are the most common benign bone tumor.
The lesions are composed of both cortical and medullary components and they have a hyaline cap.
The pathognomonic feature is the continuity of tumor with the underlying bone cortex and medullary canal.
These bone tumors occur more commonly in males and typically present during childhood and adolescence.
They generally occur spontaneously and are found incidentally,
but can also be associated with hereditary multiple osteochondromas.
These benign tumors usually occur in the knee region (i.e.
distal femur or proximal tibia),
but they can also occur in the upper limb especially the proximal humerus,
and can involve the vertebra.
Plain radiographs are often diagnostic and show the lesion with cortical and medullary components with an overlying cartilaginous cap.
Most cases of osteochondromas can be observed without treatment,
but excision may be indicated if patient develops pain,
irritation,
increase in tumor size,
or any acute symptoms.
Prognosis is good and tumor growth generally stops after the growth plates close,
but there is also a small potential for malignant transformation mainly for patients who have hereditary multiple osteochondromas.
If the cartilaginous cap is thicker than 1.5 cm,
malignant transformation should be suspected.
Ewing Sarcoma
Ewing sarcoma is the second most common primary malignant bone tumor in childhood; they typically occur in children and adolescents,
although a significant number occur in patients in their 20s.
Approximately,
95% of Ewing sarcoma cases occur between 4 and 25 years of age,
with a male to female ratio of 1.5:1.
Ewing Sarcoma arises from primitive small round blue cells in the medullary cavity.
These malignant tumors occur in the diaphysis and metaphysis of long bones in the limbs,
with the femur being the most common location; and flat bones such as the pelvis,
scapula and ribs.
Ewing sarcomas have various appearances on plain films and CTs.
They are most often permeative,
appearing as moth-eaten destructive lytic lesions.
They could also have an onion skin appearance of laminated periosteal reactions or sunburst appearance of periostitis.
In addition,
the can stimulate reactive new bone that give lesions a sclerotic appearance. Systemic chemotherapy with surgical resection and/or radiotherapy is the mainstay treatment of Ewing sarcoma.
The 5-year survival rate for patients with local Ewing sarcomas is approximately 70%,
however,
the 5-year survival rate is about 15- 30% in those with metastases at the time of diagnosis.
Multiple Myeloma
Multiple myeloma is the most common primary malignant bone tumor in adults; the patient age is typically over 40,
with the majority of the cases diagnosed in between ages 50 to 70.
The male-to-female ratio is approximately 2:1.
These lesions are formed from monoclonal proliferation of malignant plasma cells which produce immunoglobulins.
Multiple myeloma occurs in hematopoietic locations with red marrows; most common locations include the vertebrae,
ribs,
skull,
pelvis and proximal long bones.
Radiographically,
multiple myeloma typically has a diffuse permeative appearance with sharp margins (punched out and/or moth-eaten lesions),
with occasional endosteal scalloping when the cortex is involved. Additonally,
multiple myeloma can rarely present with multiple sclerotic foci resembling diffuse metastatic disease,
occurring in approximately 3% of the patients.
One of the characteristic appearances of multiple myeloma is “raindrop skull” which is defined by multiple punched out lesions of various sizes scattered throughout the calvarium.
Multiple myeloma remains an incurable disease.
Osteosarcoma
Osteosarcomas are osteoid-producing malignant tumors.
They are the 2nd most common primary bone malignancy and usually occur in children and adolescents less than 20 years of age,
but they can occur at any age.
There is a bimodal distribution with a peak between 12 and 16 years of age and the other at 65 years.
Risk factors depend on the age of the patient.
Paget disease of the bone and prior chemotherapy/radiation are risk factors for older patients whereas,
osteosarcomas tend to develop sporadically or due to hereditary disorders in children.
The tumors involve the metaphyseal areas of long bones.
The distal femur is the most common,
but they are also found in the proximal tibia,
and humerus.
The hip,
shoulder,
and maxilla are also potential locations.
Classic imaging features are a sunburst appearance,
periosteal lifting,
and formation of Codman’s triangle.
Bone destruction and new bone formation in soft tissues are also features that are seen.
Treatment involves chemotherapy and surgical resection.
Osteomyelitis
Osteomyelitis is the inflammation of bone marrow due to infection.
It has bimodal distribution with children under 5 and adults over 50 being affected most.
Patients with impaired wound healing,
and those with indwelling intravascular devices are particularly at high risk.
Prognosis is favorable if identified early,
but treatment must be initiated promptly in order to prevent complications.
Typically,
the long bones of extremities are most often involved in children and the vertebrae,
hips,
and feet are most common in adults.
In neonates and children,
the metaphysis is usually involved.
In adults,
the epiphysis and subchondral areas are most commonly affected.
On imaging,
blurring of fat planes,
cortical destruction,
periosteal reactions,
sequestra,
cloaca,
sinus tract formation can be seen.
In some cases of subacute osteomyelitis,
a Brodie abscess may be seen.
These can be single or multiple and are described as well-circumscribed intraosseous abscesses.
The mainstay of treatment is intravenous antibiotics.
Depending on the severity,
surgical debridement and drainage,
or amputation may be required.
Osteonecrosis
Avascular necrosis is ischemic destruction of bone that can be due to a variety of conditions.
Damage to the blood supply of the bone leads to increased intraosseous pressure,
which ultimately causes trabecular thinning,
demineralization,
and collapse.
The most common areas of involvement are the humeral head,
femoral head,
and knee.
Ficat classification and Steinberg staging are systems that are used to describe avascular necrosis based on the radiologic findings.
Early on,
MRI is the most sensitive modality and it shows the early manifestations of osteomyelitis that may not be present on a plain radiograph.
Findings such as the crescent sign,
rim sign,
or double-line sign may be seen on imaging.
The crescent sign shows subchondral radiolucency and is an indication that the bone will collapse.
The rim sign is another indication of bone instability seen on MRI.
The double-line sign shows a low-intensity signal in the outer rim representing sclerosis and a high-intensity signal in the inner rim.
This sign is seen on T2WI and is diagnostic of avascular necrosis.
The treatment options can be broken down into 3 major categories: non-operative,
joint-preserving (i.e.
core decompression),
and joint replacement.
Optimal treatment involves a multidisciplinary approach and attempts to preserve the native joint as much as possible,
ranging from core decompression to complete joint replacement.