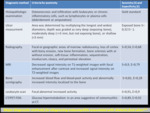
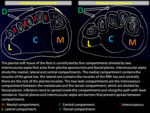
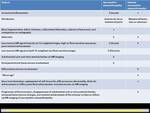
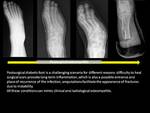
What the surgeons wants to know in our center is defined below:
1.
Existence and extension of osteomyelitis in presurgical,
postsurgical contexts and discrimination with Charcot neuro-osteoarthropathy (CN).
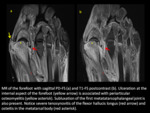
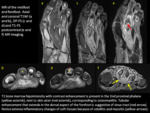
Fig. 1
2.
Which kind of involvement is existing in the soft tissue (cellulitis,
phlegmon,
gangrene or abscess),
its extension and differences from inflammatory soft tissue affection.
3.
Use of advanced MRI techniques to confirm and best delimitatate of the features in convetional MRI sequences.
4.
To delimitatate and assess the routes of spread and inform about the arterial and venous blood-pool with a MRI vascularization map.
1.
Osteomyelitis
Most common locations of osteomyelitis are the pressure points of the forefoot (metatarsal heads,
interphalangeal joints) and the plantar aspect of the posterior calcaneus at the hindfoot.
The diagnosis and difference from CN,
is important to avoid unnecessary amputations and to best delimitate the infection borders to avoid recurrences after treatment.
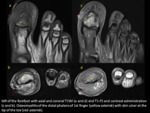
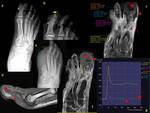
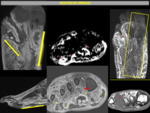
Radiologist must know the different techniques to diagnose osteomyelitis and their reliability.Fig. 2
The choice of the imaging modality can be different in every treating center; the election must be made depending on the patient’s clinical presentation,
availability of equipments and expertise of physicians at the treating center.(3)(4)
MRI is the modality of choice because provides the best delimitation of the soft tissues affection and allows differentiation between osteomyelitis and CN.
We use this technique when results of X-Ray are positive for osteomyelitis,
when X-Ray is negative for osteomyelitis with high clinical suspicion of infection or as a guide to perform a biopsy.
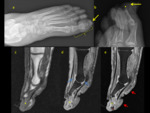
It is important to know that on conventional radiology and CT,
bone infection may not show up on the first 7-10 days(5) in the form of demineralization,
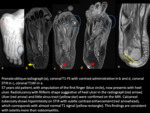
destruction and periosteal reaction.Fig. 3
1.1MRI features
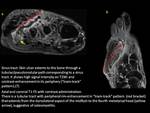
The easiest method to determine if osteomyelitis is present,
is following a skin defect or sinus tract to bone and check the bone marrow signal.
Clear hypointensity on T1WI associated with avid enhancement in the bone marrow is a primary sign of osteomyelitis.
T1 should be used to assess the spread of bone infection.(6)
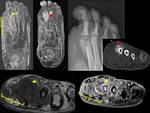
Periosteal reaction and cortical interruption are another reliable signs of osteomyelitis.Periosteal reaction appears as a linear hipointensity and hiperintensity on T1WI/T2WI,
around the cortical with avid contrast-enhancement.(7)(8)Fig. 22
Ghost sign is a specific sign of osteomyelitis.(9) It consists in a difficulty to identify the shape of the bone with an ill-defined margins on T1WI that reappears after contrast injection.
Fig. 14 Fig. 22.
There are multiple secondary signs like ulcers,
sinus tract,
cellulitis,
abscess,
gangrene and septic arthritis that must be reviewed to make a correct diagnosis and not confuse with (CN).Fig. 22,Fig. 23.
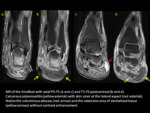
Osteitis is a reactive change to soft-tissue or cortical infection,
not to be confused with osteomyelitis.
Bone marrow edema in osteitis shows hyperintensity on T2WI and fairly normal signal in T1,
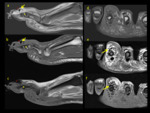
although contrast-enhancement may be present.Fig. 4,Fig. 5,Fig. 6,Fig. 7.
2.
Soft tissue disease
2.1 Skin callus
Redistribution of fat and formation of skin callus appears as an area of low signal intensity on T1WI and T2WI with variable contrast-enhancement that may mimic soft-tissue infection.
The absence of surrounding soft-tissue signal alteration is typical in calluses.
Typical locations are below the first and fifth metatarsal heads and at the tip of the great toe,
in patients with rocker-bottom deformity appear under the cuboid bone.
2.2 Skin ulcer
Skin ulcer is almost mandatory in the diagnosis of osteomyelitis.
In general,
location of skin ulcers are similar to those of calluses.
In non ambulatory patients can be located in the calcaneus or lateral malleolus.
These skin ulcers facilitate direct inoculation of the bacterial agents in soft-tissue and bone.
Skin ulcers appear as focal skin discontinuities with elevated margins,
high signal intensity on T2WI,
with rim-like contrast enhancement of the granulation tissue located at the periphery of the ulcer.Fig. 8,Fig. 9.
2.3 Sinus tract(7)Fig. 10
2.4 Cellulitis
It is an acute non-necrotizing inflammatory process involving the skin and subcutaneous tissues.
Clinically,
it presents with pain,
erythema,
edema and warmth.
Nevertheless,
similar symptoms are observed in diabetic patients without infection due to ischemia and venous insufficiency or in patients with early phases of neuropathic disease.
On MR,
cellulitis appears as a skin thickening and reticulation of subcutaneous fat,
with intermediate signal intensity on T1WI and high signal intensity on T2WI.
Contrast-enhancement appears in cases of cellulitis but not in edema presented in diabetic patients without infection.Fig. 4
2.5 Phlegmon
As the infection progresses,
areas of cellulitis are replaced by areas of phlegmon.
On MR,
phlegmon appears as ill-defined areas with mass effect and without the characteristic trabeculation of the subcutaneous fat.
They show low signal intensity on T1WI,
variable signal intensity on T2WI depending of the grade of liquefaction and homogeneous contrast-enhancement.Fig. 11
2.6 Abscess
Abscesses are uncommon in patients with diabetes and they are usually located close to the skin and sinus tracts.
On MR,
abscesses appear as collections of fluid signal intensity (pus),
surrounded by peripheral an irregular rim of contrast enhancement and T2WI hiperintensity.
Caution must be taken when interpreting the peripheral rim enhancement of fluid collections,
because it is constant in abscess but is also common in fluid collections next to non infected neuropathic joints.(10)Fig. 12,
Fig. 13
2.7 Septic arthritis
It is usually located in interphalangeal and metatarsophalangeal joints in cases of lateral ulceration,
or in ankle and subtalar joints in cases of malleolus or calcaneal ulceration.
On MR,
it appears as a complex joint effusion with thickened and avid contrast-enhancement of the synovial.
The most specific findings of septic arthritis are bony erosions; bone marrow edema and cartilage destruction.
Presence of soft tissue defects also elevates the suspicion and allow distinction with joint effusion.
It is important to take in account that adjacent bony surfaces may demonstrate edematous changes,
seen as increased T2WI signal,
which can be seen in either septic arthritis or osteomyielitis.
The bone marrow hipointensity in T1 will discriminate osteomyelitis from osteitis next to an infected joint.Fig. 14
2.8 Septic tenosynovitis
It usually affects peroneal tendons when lateral malleolus ulcer is present,
Achilles tendon from calcaneal ulcer and flexor tendons from plantar forefoot ulceration.
On MR,
it appears as a thickened and avid contrast-enhancement around the tendon.
Presence of complex fluid and even gas in the tendon sheath can be seen.
Partial or complete rupture of posterior tibial and Achilles tendon may be present in these patients because of deformities and angiopathy.
Fig. 14
2.9 Myositis
On MR,
it appears as diffuse muscle enlargement,
high signal intensity on T2WI and avid contrast-enhancement.Fig. 15
2.10 Gangrene
Devitalized tissue appears as wedge-shaped and non-enhancing areas due to absence of vascularization,
sometimes surrounded by reactive granulation tissue that enhances.
Superimposed infection (wet gangrene) may show intralesional gas that may spread along the fascial planes,
not to be confused to the gas entered in soft-tissues from the skin ulcer.
Fig. 12,
Fig. 13
3.
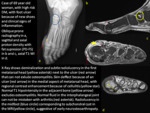
Advanced MRI techniques
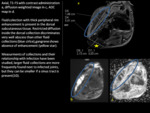
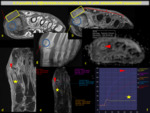
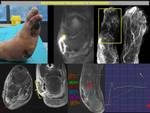
Diffusion and dynamic contrast enhancement MRI (DCE-MRI) can be used to differentiate osteomyelitis from CN.
Described cut-off values are 0,98-1.04 x10-3 mm2/s for diffusion.
Ktrans value of 0.11 ml/min and Ve value of 0.19 ml/min are defined as possible cut-off values to discriminate CN from osteomyelitis in DCE-MRI.(11)(12)Fig. 16,Fig. 17,Fig. 18
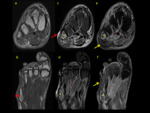
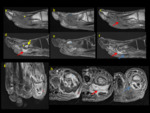
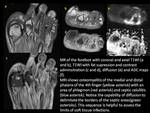
4.Routes of spread and vascular map
Involvement of different bone and soft tissue structures have demonstrated different patterns of spread,
assessing possible routes of spread like septic arthritis,
compartments involvement and presence of tenosynovitis is primordial.
Different compartments are partial barriers that prevent the spread of the infection,
but spread can occur between them.
Joint spaces are poor obstructions to the spread of infections and periarticular osteomyelitis.
Interestingly,
tendons and their sheaths are not a common pathway for the spread of infections but they can be commonly local infected.
(13)(6).Fig. 19,Fig. 20 Fig. 21,Fig. 22