Keywords:
Infection, Acute, Diagnostic procedure, Audit and standards, Ultrasound, CT, Emergency, Abdomen
Authors:
P. Sousa1, A. Ferreira2, L. Gargaté1; 1Loures/PT, 2Lisboa, Grande Lisboa/PT
DOI:
10.26044/ecr2019/C-0583
Results
In the period considered a total of 311 patients underwent appendectomy for suspected acute appendicitis.
Patients were aged between 3 and 96 years old,
with an average age of the cohort of 34 years.
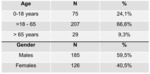
The sample was divided into 3 groups of age as shown in Table 1.
The majority of patients were adults (excluding senior adults),
with a slight predominate of males (59.5%).
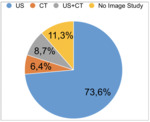
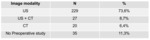
Preoperative imaging was solicited in 88.7% of the suspected cases of acute appendicitis,
with ultrasound as a first line request in 92.8% of those cases (vs 7.2% for first-line CT) - Table 2.
Only around 40% of patients with an inconclusive US report underwent complementary CT pre-operatively (12 cases in 29 inconclusive US reports).
Overall,
of the patients that had pre-operative imaging,
only 17.0% eventually did CT,
whether as a first line or complementary modality (47/276 imaging cases).
Histological results yielded 94.5% of acute appendicitis,
4.8% of negative appendicitis and 1 case of an inflamed appendix by contiguity with Crohn’s disease and another case of appendix’s cystadenoma.
The appendix was visualised in 80.9% of all the cases in which the US was used,
and in 81.6% of the histologically proven appendicitis,
with an average outer diameter of 9.5 mm.
The appendix was not visualised in 49 cases,
most of them “inconclusive” or “negative” to the US,
noticeably 62.1% of the inconclusive reports.
US reports yielded 7 false positives and 26 false negatives,
resulting in an estimated sensitivity and PPV of 87.9% and 96.4%,
respectively,
with a NAR after a positive ultrasound report of 3.6% - Table 3.
Including all patients that underwent an appendectomy,
the overall NAR was 5.5% (294 confirmed appendicitis/311 total cases).