Hypersensitivity pneumonitis is divided into three subtypes,
each with typical clinical,
laboratory and radiographic findings,
although there may be some interposition.
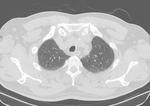
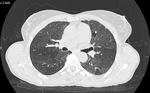
Acute hypersensitivity pneumonitis (Fig.
1):
The radiologic diagnosis of acute hypersensitivity pneumonitis may be difficult due to clinical non-specificity and rapid resolution of symptoms.
Often these patients are treated empirically for infections or asthma without proper diagnosis ever being made.
However,
even in the absence of a correct diagnosis clinical improvement of patients can occur by cessation of antigen exposure or administration of corticosteroids.
Typical acute CT findings consist of homogeneous ground-glass and alveolar opacities.
These changes are usually bilateral and symmetric and may have a lower lung zone predilection.
In short,
the acute phase is determined by diffuse airspace abnormality without fibrosis.
Subacute hypersensitivity pneumonitis:
Subacute hypersensitivity pneumonitis is often a progressive and insidious disease resulting from prolonged exposure to an antigen for weeks or months.
There may be some overlapping of the imaging findings between acute and subacute hypersensitivity pneumonitis.
Typical imaging findings consist of:
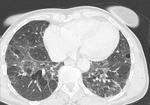
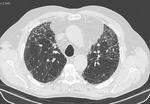
- Ground-glass opacities (GGO) (Fig.
2) - often bilateral and symmetrical and result from chronic interstitial inflammation
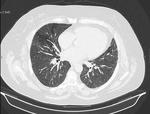
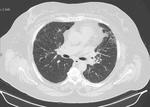
- Centrilobular nodules (Fig.
3)- often numerous,
small (<5mm),
evenly spaced and ill-defined.
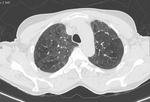
- Mosaic attenuation pattern (Fig.
4).
In HP this pattern is mainly caused by airway disease and correspond to air trapping areas,
especially visible in the expiratory CT.
Air trapping areas are visible as lobular
low attenuation regions.
- Headcheese sign (Fig.
5) results from the concomitant presence of ground-glass opacities,
normal lung areas,
and air trapping areas.
- Cysts (Fig.
2) are observed in about 13% of patients.
Chronic hypersensitivity pneumonitis (Fig.
6 and 7):
Chronic hypersensitivity pneumonitis takes months to years to develop and implies the presence of fibrosis that indicates irreversible nature of lung damage.
Interstitial fibrosis has usually a bilateral patchy pattern of distribution and translates by distortion of normal pulmonary architecture,
reticulation,
traction bronchiectasis,
and mild honeycombing.
There is often a middle or upper zone predominance with sparing of the lung bases.
Other imaging findings include superimposed findings of subacute HP (ground-glass opacities or micronodules - suggestive of active inflammation) and lobular areas of hyperlucency (mosaic attenuation pattern).