Keywords:
Interventional vascular, Computer applications, Cardiovascular system, Experimental, Computer Applications-3D, Experimental investigations, Angioscopy, Image registration
Authors:
J. Salamon, D. Weller, C. Jung, A. Frölich, M. Möddel, G. Adam, T. Knopp, H. Ittrich, R. Werner; Hamburg/DE
DOI:
10.26044/ecr2019/C-0664
Results
Case one: Visualization of an internal carotid aneurysm ( Fig. 2 )
The shape of the aneurysm could be visualized.
The neck of the aneurysm is clearly visible in the 3D visualized roadmap but covered by overlaying structures in the standard 2D MIP anterior-posterior projection.
Case two: Visualization of the middle cerebral artery ( Fig. 3 )
Spatial and temporal assessment of the bolus was feasible and revealed uniform flow distribution in the depicted area.
The generated 3D roadmap permitted accurate characterization of the vessel geometry.
In the presented case the spatial distance between virtual guide wire tip and target point could not be esimated precisely using a standard viewing angle.
Therefore,
an optimized viewing angle was determined that displays the centerline between the two points at its maximum length.
The calculated values of the tested camera positions are plotted in Fig. 5 B.
In order to establish a consistent mechanism for the view selection process,
the camera position that captures the vessel geometry from a cranial view was preferred.
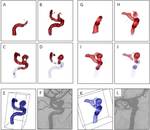
Case three: Visualization of the hepatic artery ( Fig. 4 )
The 3D visualization of the vascular branches of the hepatic artery clearly showed their spatial course and emphasized the arrangement of the arteries in the z-direction.
However an artifact occurred in the immediate vicinity of two nearby branches and led to the impression that the vessel boundaries are merged.
In this case,
observation of the temporally resolved bolus front in slow-motion could be used to reveal an actual spatial separation of the two vessel branches.
To demonstrate the benefit of the developed cutoff view routine,
a situation was considered were the sight of the virtual guide wire tip is obscured by superimposed vessels.
Restricting the view to the vessel branch that contains the catheter tip yields a clear sight of the targeted vessel area ( Fig. 4 I and J).
Catheter guidance at the vessel bifurcation was optimized by changing the viewing angle.
The automated camera adjustment procedure described above was applied to maximize the projected triangle area.
The sampled values are plotted in Fig. 5 E and G.