The approach to a patient with a mass in SCF requires a thorough knowledge of their anatomy,
the pathologies that may arise there and their demographic specifications.
Due to its complex constitution,
the detection of a SCF lesion of unknown etiology requires adequate clinical,
laboratorial and imaging correlations in order to reduce the differential diagnosis.
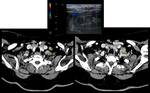
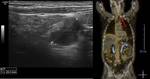
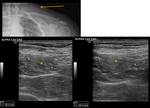
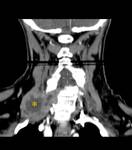
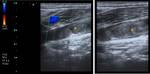
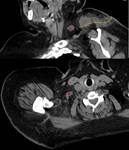
The most frequent cause of SCF lesions are lymphadenomegaly,
of inflammatory (Fig. 5 and Fig. 6) or neoplastic etiology.
However,
the differential diagnosis of a SCF lesion or mass should also include the following etiologies: invasion/direct extension by other tumors,
primary tumors,
lymphatic,
vascular,
nervous,
musculoskeletal,
congenital and traumatic.
The most common lesion in SCF is lymphadenomegaly,
more specifically metastatic lymphadenopathies.
A SCF lymphadenomegaly may represent the first detectable metastasis of an occult tumor,
a new metastasis from an already known neoplastic disease or a relapse.
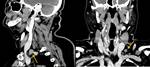
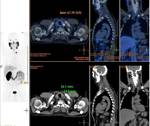
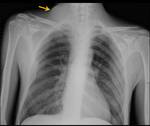
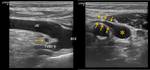
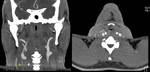
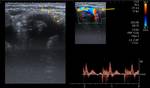
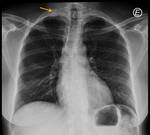
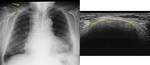
Tumors that metastasize most to the SCF are lung (Fig. 7 and Fig. 8),
esophagus and breast carcinomas,
but metastases of tumors of the stomach,
pancreas,
colon,
kidney,
bladder,
ovary,
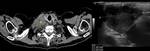
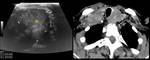
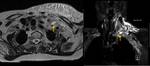
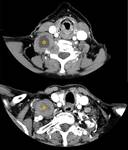
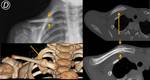
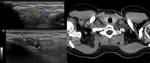
testis and prostate (Fig. 9 and Fig. 10) are described in the literature.
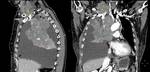
The SCF may also be the site of manifestation of a regional/local tumor with invasion or direct extension to the structures contained there,
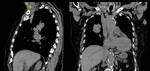
such as tumors of the lung (Fig. 11 and Fig. 12),
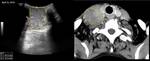
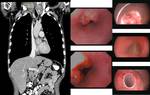
esophagus (Fig. 13,
Fig. 14,
Fig. 15 and Fig. 16) or thyroid and parathyroid glands (Fig. 17 and Fig. 18).
Lipomas can be found almost anywhere in the body.
In the neck,
they are more common in the posterior cervical space.
They are composed of mature adipose cells and surrounded by a fine fibrous capsule,
manifesting itself as a homogeneous mass with regular and well defined borders (Fig. 19).
Virtually all of them are benign,
but liposarcomatous transformation may occur.
One of the structures that passes through the SCF is the terminal portion of the thoracic duct,
the largest lymphatic trunk in the human body.
It drains the lymph from the lower half of the body and the gastrointestinal tract into the large cervical veins.
Its location,
branches and trajectory in the mediastinum and cervical region can present with multiple variants.
The most common anatomical configuration is the thoracic duct passing behind the carotid artery and between the vertebral and internal jugular veins,
leading to the venous circulation of the left side (95%) in the jugular-subclavian confluent or in its vicinity.
It can also drain to the right side (2%) or even bilaterally (3%).
The terminal portion of the thoracic duct can be imaged by CT,
MRI or high resolution US,
with the US having the highest detection rate of the cervical portion of the thoracic duct.
Although CT and MRI are superior in assessing the full extent of the thoracic duct,
the excellent resolution of the current US,
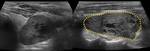
the possibility of functional evaluation and its dynamic component make it an important diagnostic tool in the investigation of chylothorax,
chylous ascites and cysts/lymphoceles (Fig. 20 and Fig. 21).
The main abnormalities of this structure and affecting the lymphatic flow may be caused by obstruction, trauma or tumor infiltration.
The normal mean diameter of the terminal portion of the thoracic duct is about 2.5 mm.
Diseases that increase the volume of lymphatic flow,
such as congestive heart failure,
liver cirrhosis and inflammatory bowel diseases,
induce dilatation of the thoracic duct,
which in this segment can reach 13 mm.
One of the characteristics of the SCF is its complex vascular-nervous content.
Due to being crossed by multiple vascular structures and by the brachial plexus,
various vascular or nervous (Fig. 22 and Fig. 23) pathologies may appear.
The most common vascular condition is thrombosis of the distal portion of the internal jugular vein (Fig. 24 and Fig. 25),
but aneurysms,
pseudoaneurysms,
post-surgical changes (Fig. 26) or even anatomical variants may also be observed.
Among the musculoskeletal changes that can occur in the SCF,
the most frequent are of congenital [alterations of the 1st rib,
cervical rib (Fig. 27),
scoliosis],
degenerative and traumatic (Fig. 28 and Fig. 29) origins.
Although it is less common,
when there is a SCF lesion it is also important to consider congenital pathologies (Fig. 30) of the various structures that constitute or cross the SCF as well as traumatic lesions (Fig. 31,
Fig. 32,
Fig. 33 and Fig. 34).