Although it fulfills an essential function such as the irrigation of the small intestine and part of the large intestine,
the SMA is a forgotten vessel in the abdominal ultrasonographic study,
both on duty,
routine or in the abdominal Doppler evaluation.
However,
this vessel may be affected by various pathologies,
both stenotic/occlusive (atherosclerosis or fibromuscular dysplasia and non-atherosclerotic cause) or by its own disposition,
cause extrinsic compressive pathology such as Nutcracker syndrome or Wilkie syndrome,
may also present anatomical variations.
Hence the importance of its evaluation by a non-invasive and highly available method such as Doppler ultrasound.
Knowing a methodical study procedure will allow to recognize the SMA and its neighboring structures as well as to determine its permeability and peak systolic velocity.
All this will allow a non-invasive and low-cost method to obtain information to make a correct diagnosis with a greater optimization of the exploration time in operators´ hands not yet fully trained.
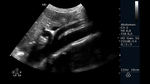
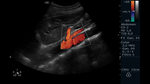
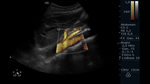
The SMA is identifiable in the abdominal ultrasound scan in B-mode as an anterior branch of the abdominal aortic artery,
immediately below the celiac arterial trunk,
this easily identifiable in the transverse view by its classic presentation in the T-form or also called "sign" of the seagull¨; distal to the same immediately or between 1-2cm it is possible to evaluate the SMA in transversal and/or longitudinal view.
Once identified it will be important to recognize possible anomalies of the SMA and its neighboring structures.(Fig.
5,6,7)
Stenosis of SMA can be a cause of chronic intestinal ischemia,
which is a rare condition although it is associated with high morbidity and mortality.
The most common cause is atherosclerosis and patients present clinically localized abdominal pain in the epigastrium that appears post-prandial.
Generally,
the pain is increasing,
so the patient reduces the daily intake of food or avoid eating,
with the consequent weight loss.
We consider important in the exploration with abdominal Doppler ultrasound,
to identify the SMA in order to rule out signs of parietal atheromatosis,
peak systolic velocity (PSV) and the ratio of the same with the aorta.
Acute occlusion of SMA usually occurs in elderly patients and is the cause of extensive intestinal necrosis with high morbidity and mortality rates.
The clinical picture may not be entirely specific,
but the patient usually presents abdominal pain,
vomiting and blood in the stool.
Early diagnosis and treatment will allow a better survival.
Although abdominal Doppler ultrasound allows evaluation of the proximal third,
as well as the PSV and SMA/Aorta ratio,
it fails to evaluate the distal portions and the collateral branches of the SMA.
Fibromuscular dysplasia can generate stenosis of the SMA of non-atherosclerotic cause.
This entity usually occurs in young women and is characterized as an idiopathic,
non-inflammatory angiopathy of small and medium arteries,
mainly of renal,
subclavian,
vertebral and carotid arteries.
Although the involvement of SMA is extremely rare,
it will be a differential diagnosis to take into account.
Another consideration to be evaluated is the importance of SMA not only for its irrigation to the intestine but also for its incidence on neighboring structures that are related to the aorto-mesenteric compass,
such as the left renal vein (LRV),
the third portion of the duodenum or the uncinate process of the pancreas.
In the Nutcracker syndrome the decrease in the mesenteric aortic compass angle can compress the LRV extrinsically,
and generate a stenosis of the same.
In this work what is evaluated is the distance between the anterior wall from the aorta to the posterior wall of the SMA,
and not so the angle formed between Aorta-SMA,
in order to demonstrate the usual distance existing.
Said distance may be modified by the pressure of the operator when performing the study,
even more taking into account that many times it is essential to turn and compress in order to move the intestinal air,
a factor that hinders the optimization of the study and which can bias the real value.
This distance may be modified in patients who undergo an abdominal CT with contrast in which the pressure of the operator is logically not present.
It should be borne in mind that this syndrome can also occur when the LRV has a retro aortic arrangement in which it is compressed between the posterior wall of the aorta and the anterior aspect of the spine.
In the cases that there is really a compression of the LRV in the aortic-mesenteric compass,
a dilation of the same and its refinement towards the medial is observed just at the compass.
The patient may or may not have signs of persistent hematuria,
low back pain and varicose dilation of the left gonadal vein.
Also another rare but not less important pathology to rule out is Wilkie syndrome or also called superior mesenteric artery syndrome.
In this there is an extrinsic compression of the third portion of the duodenum that causes high intestinal obstruction,
diagnosis that is performed late once other diagnostic possibilities have been ruled out.
Symptoms include nausea,
vomiting,
weight loss,
early satiety,
abdominal distention,
and epigastric pain.
A correct assessment of the aorto-mesenteric compass allows evaluation:
- SMA ostium gauge
- Distance between the anterior wall of the aorta and the posterior wall of the SMA at 2cm ostium
- Discard stenosis/occlusion of the origin and proximal path of the SMA
- Quantify the PSV of the abdominal aortic artery and the SMA
- Quantify the PSV ratio SMA/Aorta
- Identify anatomical variants
Although some authors suggest abdominal CT with contrast as an initial evaluation to rule out an intrinsic stenosis of the SMA due to signs of artherosclerosis/fibromuscular dysplasia,
Nutcracker syndrome or Wilkie syndrome,
this diagnostic method uses radiation,
is more expensive and less available than abdominal ultrasound in B-mode/color/power/spectral Doppler,
which would be a good option as a start of the study in case of diagnostic suspicion.