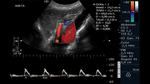
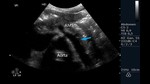
The evaluation of the SMA should be performed with the patient fasting and in the supine position using a low frequency convex transducer of 2.5-3.5MHz.
The exploration is started in the sub xiphoid transverse section identifying the abdominal aorta artery,
using in many cases the left hepatic lobe and the pancreas as an acoustic window for a correct visualization.
Once the aorta is identified,
the anterior wall of the aorta should be explored in search of the celiac trunk easily distinguishable by its typical presentation in the T-form (sign of the seagull) (Fig.9,10).
The SMA is immediately distal to the celiac trunk or 1-2cm below and is identifiable by a peripheral echogenic halo that is due to the intra-abdominal fat that surrounds it.
It should be taken into account that sometimes the SMA may have a common origin with the celiac trunk or present a minimally lateralized exit generally to the left.
To make sure that it is the SMA that is being evaluated,
it is important to continue descending until meeting both renal arteries about one centimeter below.
Once the SMA is identified,
the transducer must be turned 90° to obtain a longitudinal view of it.
In this section,
color,
power and spectral Doppler are used at an angle of less than 60°-65°,
manually angulating the transducer to find the correct angle,
given the difficulty that can arise for the operator.
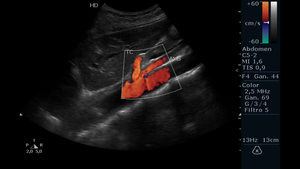
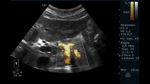
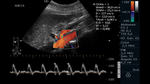
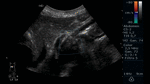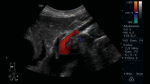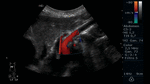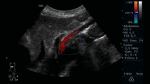
Fig. 6: Abdominal ultrasound with color Doppler evaluation. Longitudinal section showing the celiac trunk and superior mesenteric artery (TC and AMS for its acronym in Spanish, respectively). Behind them, the aorta is observed.
This window in longitudinal section allows to easily assess the permeability of the arteries under study,
the caliber of the exit ostium,
presence of atheromatous/non-atheromatous stenosis,
distance from the anterior wall of the aorta to the posterior wall of the SMA at 2 cm of the ostium (Fig.11) (as a cause of extrinsic compressive pathology of neighboring structures),
the wave flow,
and the PSV of the SMA/aorta with the subsequent calculation of the SMA/Aorta ratio (Fig.12,13).
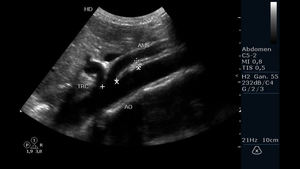
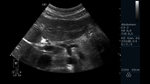
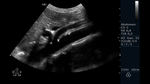
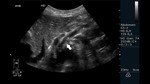
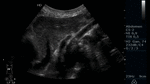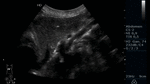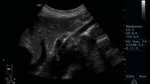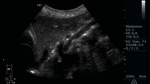
Fig. 11: Abdominal ultrasound B-mode. Longitudinal section. Measurement of the exit ostium of the AMS (for its acronym in Spanish) and the distance between the anterior wall of the aorta to the posterior wall of the SMA two centimeters from the ostium. Abdominal aorta is observed.
It is important to remember that the wave flow of the SMA is of high resistance in fasted patients and of low resistance post-intake of food.
Common findings in B-mode and Doppler ultrasound (Fig.14):
• Caliber of the ostium of the SMA:
- 8.5mm +/- 1.5mm
• Distance between the anterior wall of the aorta and the posterior wall of the SMA at 2cm from the ostium:
-Mean: 9.1mm
-Registered minimum values: 2.5mm
-Registered maximum values: 35mm
• PSV of the SMA with fasting high-strength wave flow:
-Mean: 158cm/sec +/- 39cm/sec
• PSV of the aorta with high resistance wave flow:
-Mean: 87cm/sec +/- 23cm/sec
• SMA/Aorta ratio:
-Mean: 2.22 +/- 0.66
Findings in SMA (anatomical/pathological variants)(Fig.15):
• Anatomical variants:
-Common origin with the celiac trunk.
-Right hepatic artery originating in the SMA.
-Lateralization of the origin.
-Retro aortic left renal vein.
• Stenosis/Occlusion:
-Atheromatous cause (+ frequent)
-Non-atheromatous cause (- frequent: fibromuscular dysplasia)
• SMA as a factor of extrinsic compressive pathology:
-Nutcracker syndrome
-Wilkie syndrome
• SMA aneurysms
• Isolated elevated SMA PSV indicating possible significant stenosis:
-Greater than 300cm/sec
• SMA/Aorta ratio that indicates possible signs of significant stenosis:
-Greater than or equal to 3
STENOSIS/OCCLUSION
The pathology that most frequently appears in the SMA is stenosis of atheromatous origin,
where hypo/hyperechoic atheromatous plaques can be identified in B-mode with narrowing of the color/power column before the Doppler evaluation (Fig.16,17,18,19,20).
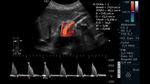
Other findings that usually appear is the increase in the PSV of the SMA (Fig.21).
It will be important to relate it to the PSV of the abdominal aorta (Fig.22),
to rule out whether it is a hyperdynamic state or a hemodynamically significant stenosis.
An SMA/Aorta Ratio greater than 3.0 will have more support to confirm this pathology.
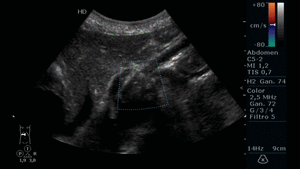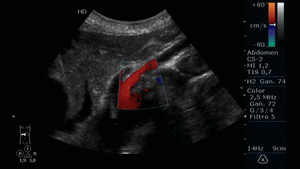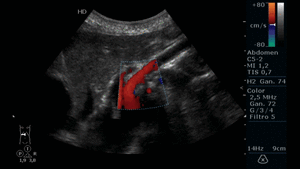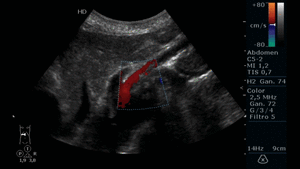
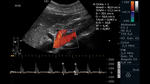
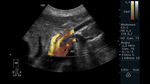
Fig. 19: Abdominal ultrasound in color Doppler mode. Longitudinal section showing the atherosclerotic plaque in the proximal third of the SMA, which causes vessel stenosis and turbulent color Doppler flow.
The occlusion of SMA is frequently observed in elderly patients and is a cause of intestinal necrosis with high mortality rates.
An early diagnosis will allow a better survival.
In this case,
the ultrasound will be limited to evaluating the proximal portion in B mode and color/power and spectral Doppler,
and distal occlusion of the vessel cannot be ruled out.
If there is a firm suspicion of this pathology,
a CT scan of the abdomen with contrast and an interventional study should be completed.
Fibromuscular dysplasia as a cause of non-atheromatous stenosis is extremely infrequent (an approximate incidence of 1% is estimated).
This entity is seen mainly in young women and affects the arteries of medium and small caliber.
SMA compromise is extremely infrequent,
however evaluation with abdominal Doppler ultrasound may show a significant increase in PSV that have been proven to exceed 400cm/sec with an SMA/Aorta Ratio greater than 4.
ANEURYSM
Although aneurysms are extremely infrequent with a slight dominance towards males,
they are important to diagnose since they require timely treatment to avoid future catastrophic events.
The measurement of the exit ostium and proximal third of the SMA should be made in a longitudinal section and will allow to evaluate if the vessel is increased 1.5 times its normal value,
confirming this pathology.
ANATOMICAL VARIANTS
Regarding anatomical variations,
it will be important to rule out if a right hepatic artery with origin in the SMA is observed,
especially in patients that require a liver transplant; to plan and perform a correct surgical preparation,
however,
given the limitations of the method it will be necessary to complete the evaluation with other methods of greater complexity.
COMPRESSIVE PATHOLOGY EXTRINSIC
In Nutcracker syndrome,
Doppler abdominal ultrasound is used as one of the initial methods of study.
The left renal vein can be identifiable at the level of the aortic-mesenteric compass (Fig.23) or retro aortic level.
In the cases in which the left renal vein passes through the aortic-mesenteric compass,
it can be assessed if it is tuned medially with a more marked dilation of the renal hilum and if there are signs of ipsilateral varicocele.
In Wilkie syndrome or SMA syndrome,
something similar happens,
but what is compressed is the third portion of the duodenum.
Its prevalence varies between 0.013% and 0.3%.
In both cases,
although its frequency is extremely low,
it is convenient to know the usual distance between the anterior wall of the aorta and the posterior wall of the SMA,
two centimeters from the ostium,
as well as the body mass index as possible causal factors.
As an initial method of study,
ultrasound could be a good option.
Continuing with the diagnostic suspicion,
both CT and MRI with contrast would be methods of choice.
In the case of Nutcracker Syndrome,
phlebography should be used as a confirmatory method.