42 patients with biopsy-proven deep DT were included in the study.
4 patients were referred for recurrent disease.
They were predominantly women (75 %) with a mean age of 36 ± 18.8 years-old,
range from 12 to 86 years-old.
DT were categorized by location in extraabdominal (35) and abdominal wall (7) The extraabdominal group was subdivided in those located at the shoulder girdle (5),
the pelvic girdle (3),
the trunk and thoracic wall (18) and extremities (8),
including one in the stump of a subcondylar amputation.
We also included 2 patients with DT in the masticatory and posterior cervical spaces.
No differences between groups were found by age or sex (Table 1)
Most of DT were solitary.
Only 2 patients (4.5%) had DT in two different locations simultaneously.
MR characteristics at diagnosis (Table 2)
The median tumor size was 6.9 cm in diameter (ranged from 1 to 32.5 cm) and median tumour volume,
45.6 cc (ranged from 0.1 to 1.4 mL).
Abdominal wall group included the largest tumours.
Most DT were ovoid (78%) with lobulated or irregular shape.
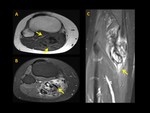
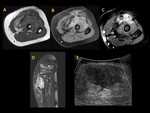
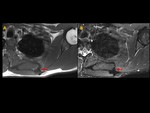
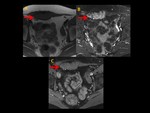
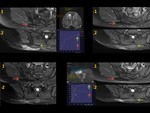
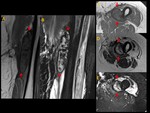
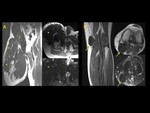
Most DT combined portions with well-defined margins with other portions characterized by tentacle-like spiculated extensions with infiltrative growth (Figure 1 to 5)
82% of DT were either isointense or slightly hyperintense to skeletal muscle in T1WI,
mostly homogeneous (80%).
High signal intensity on T2WI was observed in 85% of DT,
mostly heterogeneous (83%) because of the combination of collagen and fibroblast portions.
A specific sign of DT such as low signal bands of collagen across the tumour was present in 35% of patients (Fig. 1, Fig. 2, Fig. 3, Fig. 4, Fig. 5)
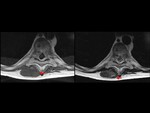
Bone marrow and periosteal signal was normal in every case,
despite the proximity of the DT to the bone.
All DT show moderate to avid contrast-enhancement and none of them present areas of necrosis in the post-contrast sequences.
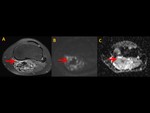
Facilitated diffusion was observed in all DT with mean values on ADC maps of 1.30 ± 0.1 (ranged from 1.15 to 1.42) (Fig. 6).
This characteristic is very helpful in differential diagnosis with other soft-tissue tumours,
especially sarcomas,
that show restricted diffusion in almost all cases,
exceptuating myxoid sarcomas.
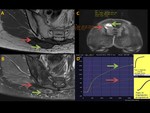
Dynamic contrast-enhanced (DCE) MR sequences were performed in 10 patients at diagnosis (23.8%) DCE sequences proved to be an useful tool in diagnosis because of they show two characteristical intensity/time curves (Fig. 7).
Type II curves (progressive) was observed predominantly in collagen-rich portions of DT and type V curves (washin and washout) was observed predominantly in fibroblast-rich portions of DT.
MR characteristics at response to treatment (Fig. 8)
Most patients were treated with surgery (80.9%) with adjuvant radiotherapy in selected cases with microscopic or macroscopic positive margins.
Medical treatments (chemotherapy or hormonal-therapy) were used in 7.1% of patients.
Only 12% of patients opted for a conservative approach of “watch and wait”.
Conclusions about effectiveness of treatments couldn't be drawn.
MR characteristics at progression or recurrence (Table 3)
Recurrence was observed in 10 patients (23.8%) with a median disease free survival of 19 months (ranged from 5 to 43 months)
Logistic regression analysis including age,
sex and tumour location,
size,
margins,
signal intensity and diffusion was performed.
None of the parameters showed a statistically major risk of recurrence.
However,
we observed a tendency to an earlier recurrence in larger tumours.
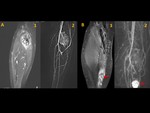
9 patients had local recurrence (Fig. 9, Fig. 10, Fig. 11).
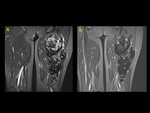
Only 1 patient had a distal recurrence in the left calf (Fig. 12),
caused probably by direct spread of the tumour through interfascial plane rather than distant metastasis.
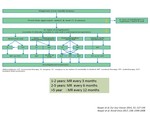
Role of MR in the consensus treatment algorithm proposed by EORTC and SPAEN (Fig. 13)
DT are slow-growing tumours that tend to progress in first 1-2 years followed by a long period of stability and a late phase of involution.
Multiple treatment alternatives have been proposed,
with variable results,
being surgery with or without radiotherapy the classical adopted option along with medical treatment such as tamoxifen,
NSAIDs...
New treatments based on cryoablation,
radiofrequency or immunotherapy have been proposed in recent years.
Several studies concluded that microscopic or macroscopic margins don't influence in the risk of recurrence,
so a more conservative approach based on functionality and cosmetic rather than radical surgery is proposed.
Several studies concluded that “watch and wait” strategy have no differences in risk of progression with classical medical treatments in selected cases.
Based on the natural history of the DT and absence of unified evidence-based approach for their management,
EORTC and SPAEN proposed a consensus treatments algorithm where imaging techniques,
especially MR,
has a pivotal role.
After biopsy-proven diagnosis,
they propose a follow-up period of 1-2 years for the asymptomatic DT,
which include a clinical evaluation and MR performed every 3 months in order to detect fast-growing or more aggressive DT.
If stability is proved,
“watch and wait” strategy may continue after 2 years,
increasing the time interval of MR (every 6 months between 2 to 5th year and every 12 months after 5th year)
Progression is defined as growth or changes in signal intensity in two consecutives MR.
No conclusions regarding the paper of DCE has been proposed,
although we found that it could be an useful tool to characterised better DT and select those with higher risk of progression.