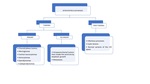
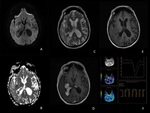
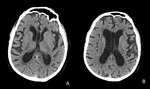
There is a great variety of intraventricular masses.
In this review,
we will classify them as tumoral (primary and secondary tumors) and non-tumoral masses (Fig.
1).
These lesions may be discovered as an incidental finding or for symptomps.
The symptoms that are present in these pathologies are very diverse and non-specific; they depend on the type,
location and age of the patient.
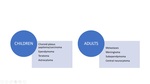
In childhood,
they can present irritability,
macrocephaly,
loss of appetite and psychomotor retardation; while in older children and adults cause headache,
vomiting,
neurological deficit and papilledema due to increased intracranial pressure.
Seizures and visual disturbances are rare.
Fever may accompany the symptoms described above in cases were an infection is cause.
A systematic approach using the location of mass (Fig.
2),
patient demographic characteristics like age (Fig.
3) and imaging appearances can often substantially narrow the differential,
and in most cases suggest the diagnosis.
Imaging techniques are part of the key to diagnosis,
with MRI being the choice to characterize them,
however,
transcranial ultrasound and Doppler can also be useful in the pediatric age.
We are going to decribe the most commun intraventricular masses and their imaging appearances.
1.
PRIMARY TUMOURS:
They are unique to the ventricle and attending to the epithelial layers and structures that form the ventricular system: ependyma and subependymal glia of the ventricular lining,
the epithelium of the choroid plexus,
and the arachnoid supporting tissue.
These include choroid plexus tumors,
meningiomas,
central neurocytomas,
astrocytomas,
ependymomas and subependymomas.
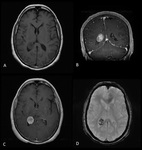
-CHOROID PLEXUS TUMORS (Fig.
4)
These tumors ventricle are more common in children (80% of cases) and represent between 2-4% of pediatric brain tumors (20% in the first year of infancy) and 0.5% of adults.
These include the choroid plexus papilloma and carcinoma.
The choroid plexus carcinoma,
occurs in younger patients (< 3 years old),
and can be indistinguishable on imaging from papillomas.
- CT: Choroid plexus papillomas are hyperdense on unenhanced CT,
and nearly 25% demonstrate calcification.
- MRI: These tumors are highly vascular,
and they may show flow voids or calcifications as areas of low signal intensity within the lesion,
frond-like borders,
avid contrast enhancement,
and their characteristic location is at the glomus of the lateral ventricle (80% of childhood choroid plexus papillomas) and hydrocephalus or hemorrhage.
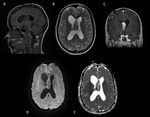
-MENINGIOMAS (Fig.
5)
Intraventricular meningiomas typically occur around the choroid plexus (80%) in the trigone of the lateral ventricle and have a distinct propensity for the left lateral ventricle.
Only 15% of intraventricular meningiomas
occur in the third ventricle,
and 5% occur in the fourth ventricle.
- CT: Hypo/isodense.
- MRI: Hypo/isointense on T1 and hyper/isointense on T2.
These calcify in 45-68% of cases, and usually have homogeneous enhancement.
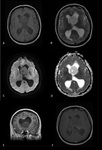
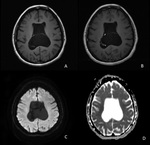
-CENTRAL NEUROCYTOMAS (Fig.
6)
Central neurocytomas are typically centered within one of the lateral ventricles along the septum pellucidum.
Their peak of presentation is usually in the third decade of life (mean age 29 years old).
They are well-defined,
lobulated lesions and often they have areas that look like cysts (a "bubbly" appearance).
- CT: iso/hyperdense.
- MRI: They are isointense to gray matter on all MR pulse sequences and show mild to moderate enhancement and calcifications sometimes.
Intraventricular neurocytomas hemorrhage more frequently than oligodendrogliomas (this is the main differencial diagnosis),
which may suggest that diagnosis.
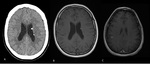
-SUBEPENDYMAL GIANT CELL ASTROCYTOMAS (Fig.
7 and Fig.
8)
This mass is the most frequent brain tumor in patients with tuberous sclerosis and it is considered pathognomonic condition.
Tuberous sclerosis is a neurocutaneous disorder that is characterized by the development of multiple benign tumors of the embryonic ectoderm (e.g.
skin,
eyes,
and nervous system).
There is a wide age range for the presentation,
from birth to the fifth decade.
It has been proposed that they arise from a subependymal node.
They have a slow growth,
a benign behavior and the indications for the resection are the increase of tumor size,
hydrocephalus or a focal neurological deficit.
They arise at the foramen of Monro and often show calcification and enhancement.
- TC: Iso/hypodense.
- MRI: Iso/hypointense in T1 sequence and iso/hyperintense in T2 sequence.
These tumors capture contrast avidly. The enhancement of subependymal hamartomas is variable and is not a useful feature in distinguishing them from subependymal giant cell astrocytomas (SGCA)
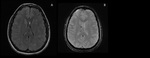
-EPENDYMOMAS (Fig.
9)
They represent 3-5% of intracranial neoplasms.
Ependymomas arise from the ependyma of the ventricular system.
The majority of intracranial ependymomas (60%) are located in the posterior fossa (infratentorial).
In pediatric patients,
ependymomas are frequently seen near the fourth ventricle,
causing characteristic widening of the fourth ventricle as well as the foramina of Luschka and Magendie.
The main differencial diagnosis are the medulloblastomas.
They tend to displace and efface the fourth ventricle.
The other 40% are located supratentorially and up to half of these are intraparenchymal.
This tumor is typically an heterogeneous mass with areas of necrosis, calcification,
cystic and hemorrhage,
that adopt an heterogeneous appearance on all modalities.
- CT: iso/hypo/hyyperdense with heterogeneus enhancement.
- MRI: iso/hypointense in T1,
iso/hyper in T2.
Heterogeneus enhancement,
with edema,
hemorrhage or calcification areas and shows restricted diffusion may be seen in solid components,
especially in anaplastic tumor.
- MRS: Ependymomas have lower NAA:Ch ratios than astrocytomas,
but the Cr:Ch ratio is higher for ependymomas than for astrocytomas and PNETs.
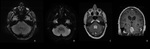
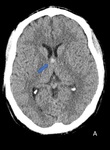
-SUBEPENDYMOMAS (Fig.
10)
Subependymomas are benign tumors that represent 0.2-0.7% of intracranial neoplasms.
Subependymomas are most commonly seen in elderly patients and males.
They typically occur near the ventricular system,
including the floor of the fourth ventricle,
along the septum pellucidum,
and along the lateral ventricular ependyma.
Subependymomas typically do not enhance and there is usually no extraventricular invasion.
- CT: hypo/isodense.
- MRI: iso/hypointense in T1,
iso/hyper in T2,
without enhancement and no edema.
They may show hemorrhage or calcification areas.
2. SECONDARY TUMOURS:
They are any intraparenchymal tumors that invade the ventricle by exophytic growth and metastases.
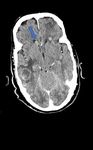
The most frequent brain tumor is glioblastoma multiforme. We present a primary brain lymphoma case (Fig.
11) and the common metastases are of the breast,
lung and kidney cancer (Fig.
12).
3.INTRAVENTRICULAR NON-TUMORAL MASSES include infectious processes such as tuberculomas or neurocysticercosis; cystic lesions (simple,
colloids,
of plexus cystics) and normal variants of the CSF space such as cavum septum pellucidum.
-CYSTIC LESIONS
Ependymal cyst is a very rare benign cystic lesions,
covered with linear ependyma and located in the lateral ventricle or near to the ventricles.
They are usually asymptomatic and incidental findings.
(Fig.
13).
- CT and MRI: attenuation and signal similar to CSF,
without restriction,
no contrast enhancement,
sometimes they may present a mass effect.
Colloid cyst typically occurs near the foramen of Monro.They can cause obstructive hydrocephalus.
(Fig.14).
- CT: hyperdense cyst
- MRI:variable signal intensities on T1- and T2-weighted images.
-NORMAL VARIANTS OF THE CSF SPACE
Cavum septum pellucidum: it is a collection of LCR located between the two leaves of the pellucid membrane.
(Fig 15).
It can be presented alone or associated with the cavum vergae.
Cavum vergae: It constitutes the posterior extension of the CSP,
extending to the posterior columns and the foramen of Monro.
Cavum velo interpositum: It is a dorsal base triangular cavity located in the choroidal fissure.