Teaching points
Emphysematous pyelonephritis is a life-threating necrotizing infection of the kidneys characterized by gas formation within or surrounding the kidneys.
The majority of patients are diabetes,
hypertension,
immunocompromised.
The pathogenesis of Emphysematous pyelonephritis generally accepted theory proposes that high levels of glucose provide a favorable environment for acidic fermentation of gas-forming microbial organisms.
The organisms are characteristically gas-forming.
The pathogen most common are Escherichia coli,
Proteus mirabilis,
Citrobacter,
Enterobacter and Candida are less frequently isolated.
The less common underlying causes include urinary tract obstruction; end-stage renal disease,
and immunosuppression unrelated to diabetes mellitus,
such as severe alcoholism or renal transplantation.
The clinical diagnosis may be difficult as the symptoms are usually non-specific,
including fever,
nausea,
general malaise,
confusion,
flank pain and dysuria.
The majority of patients have no focal physical findings; a few have costovertebral-angle tenderness.
Degree of parenchymal destruction
The characteristics of type 1 that we proposed include an absence of fluid on computed tomography images or the presence of streaky or mottled gas,
although bubbly and loculated gas may also be present.
The streaky pattern that radiates from the center of the kidney to the periphery corresponds to the macrostriations of acute pyelonephritis found on computed tomography images,
The streaky gas is probably attributed to the rapid destruction of the renal parenchyma and the outlining of the residual tissue of fibrous network by the surrounding gas,
which consists of hydrogen,
carbon dioxide,
and nitrogen.
The mottled patter probably represents partial coalescence of the streaky gas after dehiscence of the residual tissue due to high gas pressure.
Why are there no abscesses or pus? The absence of fluid or pus in virtually all patients with type 1,
appears to be an important sign.
Why? Inflammation is a process by which cells and exudate accumulate in irritated tissues and protect them from further injury by localizing the injurious agent and setting the stage for repair.
When there is tissue injury in patients with an intact immune response and uncompromised vascular supply,
there is leukocyte migration and increased vascular permeability,
which may lead to abscess formation.
In instances of vascular compromise or occlusion,
however,
there may be no fluid collection or abscess formation.
The only patient with type 1 who revealed minimal fluid collection and an almost completely destroyed left kidney recovered after nephrectomy.
The presence of exudate may imply an affective immune response.
The gas pattern or type II,
was characterized by the presence of bubbly or loculated gas and the absence of streaky or mottled gas.
Gas bubbles may become loculated or nonuniform in shape and size when they coalesce.
When the abscess cavity extends to the subcapsular or perirenal spaces,
crescent-shaped gas may develop due to distention of the capsule or fascia with both fluid and gas.
The absence of streaky or mottled gas and presence of fluid in type II would appear to reflect a good immune response and thus a slower course of the disease and a better prognosis.
Imaging findings
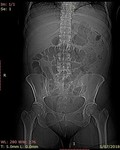
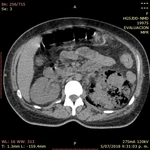
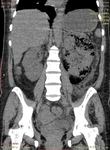
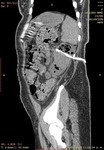
The presence of gas in the renal parenchyma with emphysematous pyelonephritis should be detected by abdominal plain radiograph which is the first imaging modality.
Diffuse mottling of the renal parenchyma with a radial distribution of gas bubbles along the pyramids has been suggested as the earliest sign.
The presence of gas bubbles in the renal parenchyma,
surrounded by a crescent of gas extending into the retroperitoneal spaces,
denotes extension of the disease.
Intravenous urography usually gives no more information than the pain radiograph because of the poor renal function and poor visualization of the collecting system in patient with emphysematous pyelonephritis.
On ultrasonography examination,
intrarenal gas is identified as echogenic foci with sharp and usually flat anterior margins and distal,
dirty acoustic shadows.
However,
ultrasonography is not sensitive in detecting intrarenal gas because of confusion either with surrounding bowel gas or with calcifications within the kidneys.
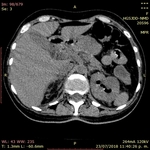
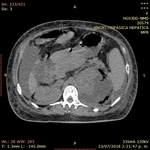
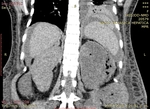
The computed tomography technique is reported as the most sensitive method for detecting gas in and adjacent to the kidney.
It has been suggested that determining whether the location of gas is in the renal parenchyma,
collecting system or perinephric space may have substantial prognostic and therapeutic implications.
Two classification systems have been developed to predict prognosis of patients with Emphysematous pyelonephritis.
Type 1 is acutely more fulminant,
with renal hemorrhagic necrosis and infarction,
than the other types.
Type 1 reveals a streaky or mottled gas pattern and no adjacent fluid collections.
Type 2 has a lower mortality rather than type 1,
and shows a bubbly gas pattern in the renoureteral unit and fluid either in the kidney or surrounding the kidney.
Treatment based on CT
A classification system proposed by Huang and Tseng that categorizes patients on the basis of the extent and location of the gas collections using only computed tomography,
to guide management and predict prognosis.
| Class 1: findings gas in collecting system only. |
Management IV antibiotics; if abscess is present,
then also percutaneous catheter drainage and decompression of urinary tract obstruction. |
| Class 2: Gas within the renal parenchyma without extension to the perirenal space. |
Management same as class 1. |
| Class 3A: Extension of gas or abscess to the perirenal space. |
Immediate nephrectomy and antibiotics if clinical risk factors (thrombocytopenia,
acute renal failure,
mental status changes and shock) are apparent. |
| Class 3B: Extension of gas or abscess to the pararenal spaces. |
Management same as class 3A. |
| Class 4: Bilateral Emphysematous pyelonephritis or a solitary functioning kidney with Emphysematous pyelonephritis. |
Management IV antibiotics,
catheter drainage and decompression of urinary tract obstruction if warranted; nephrectomy if above management fails. |
Differential Diagnosis
- Emphysematous pyelitis
- Iatrogenic (instrumentation,
or intervention of urinary tract)
- Fistolous communication with bowel