In every clinical suspicion of stroke in young,
neuroimaging forms a cornerstone.
Here we have a series of atypical presentations found on imaging in below mentioned differing case scenarios.
CASE I. A 27-year-old female patient presented to the casualty with sudden onset and progressive right-sided hemiplegia,
ataxia,
and slurring of speech.
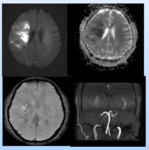
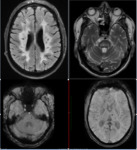
Initial MRI screening revealed restricted diffusion mainly in left occipital and high fronto-parietal lobes.
MR brain angiogram revealed marked narrowing of cavernous portion of left ICA with opening of multiple prominent lenticulostriate collaterals.
Fig. 1
Diagnosis: MOYA MOYA DISEASE/ PHENOMENON
Moyamoya disease is seen as a progressive vasculopathy leading to stenosis of the main intracranial arteries with resultant prominence of collateral vessels.
[1] A number of causes such as collagen vascular disease,
infection,
HCV-infected individuals,
patients with cryoglobulinemia and sickle-cell disease individuals have been described for this vasculopathy.
The causal relationship when identified,
the disease is described as Moya Moya syndrome.
However,
the absence of such causes is termed as Moyamoya phenomenon.
TYPICAL IMAGING FINDINGS:
- On both CT and MRI,
the presence of occlusions or stenoses of large intracranial vessels with the corresponding prominence of collateral vasculature suggest a suspicion of the disease,
especially in young individuals.
- MRI allows a better evaluation of the range and time phase of ischaemic lesions.
[2]
- CT and MR angiography are useful in depicting the classical puff of smoke appearance.
- FLAIR sequence is useful to diagnose the ‘ivy sign’,
i.e.
seen as hyperintensity along the fissures and gyri of cerebral hemispheres,
suggesting reduced cortical flow.
CASE 2. A 43-year-old male patient who comes with the complaint of mild weakness in bilateral upper and lower limbs and progressive dementia.
There appears to be no account of family history for the same.
The MMSE score in this patient was 14/30.
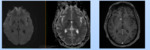
MRI findings in this patient were suggestive of multiple varying age infarcts in bilateral centrum semiovale and bilateral corona radiata. Similar lacunar infarcts were seen in midbrain and pons. Few microfoci showing blooming on SWI were seen in brainstem and left thalamus. Also,
the cerebral atrophy appears to be out of proportion.
There was relative sparing of occipital white matter and subcortical U fibres. Fig. 2
Diagnosis: Cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy (CADASIL)
CADASIL and CARASIL are autosomal dominant and recessive conditions causing recurrent subcortical strokes,
often complicated by subcortical dementia.[3] MR imaging plays a central role in the diagnosis and evaluation of patients with these diseases.
TYPICAL IMAGING FINDINGS:
MRI forms the gold standard investigation modality.
There are three basic features on neuroimaging:
- White matter hyperintensities (WMHs) on MRI and white-matter hypodensities on CT mainly in the periventricular region and in deep white matter but less frequently in superficial white matter with predominantly affected regions being frontal,
parietal,
and anterior temporal,
followed by external capsule.
- Lacunar infarcts in the semioval center,
thalamus,
basal ganglia,
and pons.
- Cerebral microbleeds.
The typical presence of anterior temporal white matter hyperintensity and involvement of external capsule is classical.
CASE 3. A 21-year old male patient comes with sudden onset history of weakness in left upper and left lower limbs and slurring of speech with the symptoms being stagnant for 3 days and sudden worsening of existing symptoms within 2 hours.
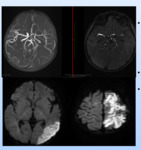
On MRI,
acute infarction with hemorrhagic conversion was seen involving subcortical white matter area in the right frontotemporal lobe and right ganglio-capsular region. MR angiography was suggestive of dissection with intimal flap formation in cavernous portion of right ICA.
Diagnosis: Cervicointracranial artery dissection
These dissections could be both traumatic or spontaneous.
[4] Such patients can prevent with features suggesting stroke and on neuroimaging the findings are suggestive of territorial infarcts.
TYPICAL IMAGING FINDINGS:
- CT angiography/ MR angiography features suggesting dissection present with possible associated intramural hematoma.
- Most often,
ICA dissection is characterized by a narrow eccentric lumen with increase of the external diameter of the artery seen on CT angiography.
- Time-of-flight (TOF) MR angiography can demonstrate subacute intramural hematoma.
In these patients,
the neuroimaging can reveal both ischemic and hemorrhagic stroke components.
CASE 4. A 27-year old female patient comes with sudden history of right hemiplegia and slurring of speech with history of symptoms being stagnant for 6-7 hours and suddenly sudden worsening of existing symptoms.
On examination,
no peripheral pulses were palpable.
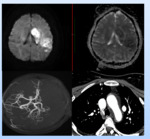
MR imaging was suggestive acute infarct with hemorrhagic conversion mainly in left MCA territory.
MR angiography was suggestive of significant luminal narrowing on left CCA and ICA.
Also luminal narrowing was appreciated in scanned portion of arch of aorta. Further patient was evaluated with CT angiography to look for extent of involvement.
Diagnosis: Vasculitis
It is an inflammatory disease of large arteries with aorta and its main branches getting mostly affected.
Young female patients are mostly affected. Pathologically,
there is accumulation of inflammatory infiltrates in tunica intima which later progresses to involve all three layers of arterial wall.
Resultant narrowing of arterial lumen and in chronic phase the vessel wall becomes calcified and fibrosis with opening of few collaterals.
Such patients in addition to stroke like symptoms can present with other variable differing constellation of symptoms which could include skin lesions,
weight loss,
fever,
fatigue etc.
TYPICAL IMAGING FINDINGS:
- MR imaging is particularly useful to look for parenchymal changes.
DW imaging is particularly useful to look for acute and chronic stages of infarction as these patients usually have infarcts which are of varying age due to presence of neo-angiogenesis.
- T2 and FLAIR images are further helpful to determine ischemic or gliotic changes and frank infarction as well as other lesions while within the subarachnoid space and white matter lesions at brain -CSF interface present near.
- Post contrast-T1W imaging helps to look for leptomeningeal enhancement and associated intraparenchymal lesions. SW MR imaging aids in the detection of microhemorrhages associated with vasculitis.
- CT angiography can show classical wall thickening,
stenosis and post-stenotic dilatation in large arteries.
Small vessel changes cannot be demonstrated on CT angiography.
5.
MISCELLANEOUS
Subacute infarct can present with confusing enhancement on post-contrast imaging leading to mis-diagnosis,
if previous history/ scans suggestive of infarction has not been elicited.