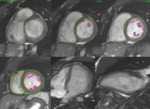
Patients population:
We retrospectively enrolled 39 consecutive patients (15F,
24M,
mean age 59±11 years,
NYHA class II-IV) with a diagnosis of DCM,
ejection fraction (EF) 25 ±5%,
left bundle branch block (LBBB) and QRS length 150 ±23ms,
who had a complete cardiovascular evaluation including clinical examination,
blood parameters,
ECG,
echocardiography and CMR with assessment of the RV morphology and function (Fig. 1).
All patients were treated with optimal medical therapy for at least 3 months (ßb 85%,
ACEI/ ATIIA 90%,
furosemide 92%,
AA 67%). We excluded all patients with ischemic etiology documented by late gadolinium enhancement.
CMR data acquisition:
All the CMR studies were performed in 1.5T Signa HDxt scanner (GE- Healthcare,
Milwaukee,
WI).
A short-axis stack from atrio-ventricular level to the apex was acquired using a steady state free-precession cine sequence (SSFP-cine), slice thickness 8mm with a 2 mm gap,
to quantify atrial dimensions,
left and right ventricular volumes and function.
Long-axis cines were also acquired to define the valve plane throughout the cardiac cycle (Fig. 2) .
An inversion recovery gradient echo sequence was used 10 minutes after gadolinium injection (Gadovist® ,
0.1 mmol/kg or ProHance®,
0.2mmol/Kg) to assess myocardial scar. Inversion times were set to null the normal myocardium.
CMR data analysis:
Analyzes were performed by two expert radiologists (more than ten years experience in CMR) using semi-automated software (Cardiac VX 1.1.0,
2015 GE,
Milwaukee,
WI).
Left and right ventricular volumes and function were calculated by using Simpson's method after manually delineating endocardial surface.
Tricuspid annular plane systolic excursion (TAPSE) was measured from the 4-chamber view (Fig. 3).
We excluded all patients with ischemic etiology documented by late gadolinium enhancement.
Statistical analysis:
Based on the response to CRT patients were divided into two groups:
Responders= improvement ≥15% in the EF at the echocardiographic follow up.
Non Responders= improvement <15% or worsening of the EF (Fig. 4).
CMR-baseline differences between the two populations were assessed by Chi square and nonparametric tests for qualitative and abnormally distributed data,
and with T student and Anova for data with a normal distribution.
We considered statistically relevant a p value <0,05.