Our intention with this observer evaluation and objective phantom measurement study was to obtain valuable information about the clinical utility of the MBIR algorithm and to estimate the potential dose reduction in order to assess the desired clinical image quality in abdominal CT for optimization purposes.
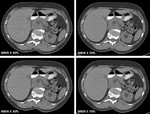
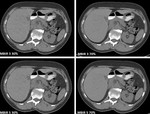
A visual demonstration of image quality comparison between 30% and 70% dose levels reconstructed with MBIR strenghts 3 and 5 at slice thickness 1mm (Fig. 10),
2 mm (Fig. 11) and 3 mm (Fig. 12) in a 65 year old study patient.
There are several clinical studies that have evaluated the dose reduction potential of the MBIR with varying range of possible dose reductions [8,9,10] when assessing different aspects of image quality.
Delineation of the liver parenchyma and overall image quality was found to be inferior for the higher strength of the MBIR,
independent of the variation in slice thickness,
and did not allow for any potential dose reduction in concurrence with Kataria et al's [8] subjective image quality assessment study.
A possible explanation for this is that noise reduction in IR images is non-linear as the algorithm reduces noise aggressively in regions that are uniform and less aggressively in regions with edges and anatomical features.
Since MBIR strength 5 reduces noise substantially (Fig. 8),
which
contributes to the unusual appearance of the images,
therefore some degree of noise is preferable to render the image as sharper and increase the diagnostic confidence.
Other studies [11,
12] on the other hand,
have found no difference in image quality between MBIR strengths 3 and 5.
Perhaps the use of lower kV settings,
that have higher inherent noise in the images,
can partly explain the improvement in image quality for the higher strength in these studies.
MBIR 3,
on the other hand renders images of better quality, for all criteria assessed,
due to less noise reduction compared to MBIR 5 as demonstrated in Fig. 8
In conclusion MBIR strength 5,
compared to strength 3,
has different effects on different image quality criteria.
With increase in slice thickness from 1mm to 2mm or 3mm,
independent of the IR algorithm strength,
a decrease in noise and increase in resolution and CNR is observed,
and a dose reduction should be possible.
A comparison of MBIR strength 5 and strength 3 at same slice thickness also shows improved image quality for certain image quality criteria,
in favor of the higher strength,
possibly allowing for some dose reduction.
However,
strength 3 is still superior in image quality compared to strength 5 thereby rendering better image quality for all the criteria assessed.
The clinical utility of strength 5 is limited.
Acknowledgements
We thank our participating radiologists,
Anki Pozson,
Jenny Ă–man,
Senija Halilic and Thomas Wiessler for grading the images.
We acknowledge medical physicist Henrik Elgström who performed the quantitative analyses of Noise-Power Spectra.
This work was supported by ALF- and LFoU-grants from Region Östergötland and the Medical Faculty at Linköping University.