Polyarteritis Nodosa (PAN)
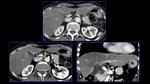
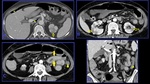
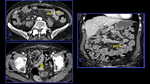
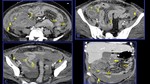
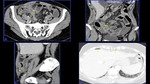
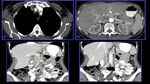
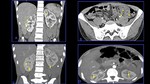
It is a necrotizing vasculitis that is characterized by the presence of multiple aneurysms (approximately 50-60%) due to erosion and weakening of the arterial wall by the inflammatory process.
This vasculitis most commonly affects the kidney (80-90%),
followed by the gastrointestinal tract (GIT) (50-70%),
liver (50-60%) and spleen (45%).
Two thirds of patients present symptoms like abdominal pain,
nausea and vomiting associated with organ damage secondary to ischemia or infarction,
causing manifestations such as hypertension,
peripheral neuropathy,
heart failure,
skin nodules,
among others.
The small intestine is the most frequently involved in GIT followed by the mesentery and the large bowel (Fig.
2,
3 and 4).
There are not specific diagnostic test.
Anti-HB antibodies are positive in 30%,
with ANCA + (perinuclear) in a variable percentage.
If left untreated it is associated with kidney failure,
GI complications such as ischemic areas or perforations; and cardiovascular complications.
With immunosuppressive therapy the disease can be controlled in 90% of cases.
Diagnosis is made by findings in biopsied tissue or linked with findings in the angiography of microaneurysms within the renal,
mesenteric or hepatic vasculature,
without being pathognomonic of PAN as they may be found in other necrotizing vasculitis,
such as the ones associated with drug abuse,
Wegener granulomatosis,
and systemic lupus erythematosus (SLE).
SYSTEMIC LUPUS ERYTHEMATOSUS (SLE).
Disease of unknown etiology in which tissues and cells are damaged by autoantibodies and immune complexes.
Abdominal manifestations may be secondary to the primary involvement with SLE or complications of immunosuppressive therapy.
Vasculitis in SLE can be present in any part of the GI tract,
from the esophagus to the rectum.
Other causes of vascular insufficiency should be considered before making a diagnosis of lupus vasculitis (CMV or other infections,
colitis and mesenteric vessels thrombosis associated with antiphospholipid syndrome).
The exact incidence of lupus vasculitis is unknown.
It may occur in less than 5% of patients with SLE. The manifestations can be range from quiescent to a colitis with diarrhea,
mucosal ulceration with bleeding,
intestinal infarction,
and perforation.
Although less common than the involvement of the small bowel; cases of necrotizing vasculitis of the appendix,
transverse colon,
splenic flexure,
sigmoid colon and rectum with perforation have been documented.
Imaging findings are characterized by the presence of a circumferential thickening of the intestinal walls,
with multisegmental and symmetric compromise,
primarily in the jejunum and ileum in a variable length.
Typically involves more than one vascular territory predominantly the superior mesenteric artery (SMA). CT features includes conspicuous prominence of mesenteric vessels with palisade pattern or comb-like appearance (CT comb sign) supplying focal or diffuse dilated bowel loops,
ascites with slightly increased peritoneal enhancement,
small bowel wall thickening with double halo or target sign,
and increase in attenuation of mesenteric fat (Fig .
5).
Pneumatosis intestinalis is rare and is associated with severe ischemia and necrotizing enterocolitis.
It is suggested that intestinal thickness of 9 mm should be considered high risk factor for recurrent enteritis.
Early high dose steroid therapy revealed complete or marked resolution of the abnormal CT findings.
BEHÇET´S DISEASE
Gastrointestinal manifestations in Behcet's disease are very common.
The most frequently associated signs include abdominal pain,
nausea,
diarrhea,
anorexia and abdominal distension.
The incidence varies from 15 to 50% based exclusively on symptoms and 0.7 to 30 % according to endoscopic or imaging findings.
It is characterized mainly by presenting large penetrating ulcers which may be complicated by perforation,
hemorrhage,
or fistula.
It can exist in all GI tract,
from the mouth to the anus,
being the terminal ileum and cecum the main sites of ulcers with diffuse intestinal involvement in less than 15%.
The above findings difficult to distinguish with inflammatory bowel disease (mainly Chron´s disease) (Fig.
6).
GIANT-CELL ARTERITIS (GCA)
It's one of the most common systemic vasculitis in adults.
It affects primarily the extracranial branches of the carotid artery in patients older than 50 years.
The dreaded complication is loss of vision.
Approximately 40% of patients may present with atypical manifestations in which headache,
jaw claudication and visual symptoms do not occur or are less prominent,
and may involve the supra-aortic trunks and the abdominal aorta (Fig.
7).
PAN-LIKE VASCULITIS ASSOCIATED WITH HIV INFECTION.
It is classified as vasculitis associated with systemic diseases.
The PAN associated with HIV,
predominantly affects small arteries of the skin,
nerves and GI tract,
being the renal involvement rare unlike the classic PAN.
The pathogenesis are immune complexes deposited in the microcirculation.
Another difference with classic PAN includes the lack of association with hepatitis B and its clinical course.
PAN used to be fulminant or with a progressive worsening with acute relapses,
that is not typical in the HIV population where is usually constant (Fig 8).