Conventional radiography:
Radiographs of the abdomen may demonstrate mass effect from the tumor due to their large size at presentation. The calcifications may be detected with abdominal radiographs.
On excretory urography,
adrenal carcinoma often causes mass effect on the ipsilateral superior pole of the kidney,
usually displacing the upper pole of the kidney laterally and inferiorly.
Computed tomography (CT)
With the advent of cross-sectional imaging,
the evaluation,
staging,
and treatment of adrenocortical carcinoma have vastly improved.
CT is usually the first imaging modality used to define an adrenal mass such as adrenocortical carcinoma.
Adrenocortical carcinoma is seen as a large mass,
often with central necrosis.
Calcification may be present.
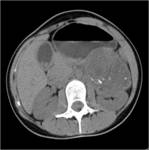
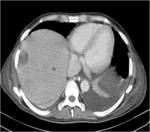
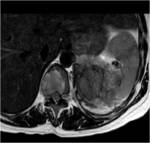
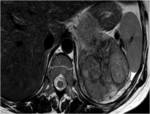
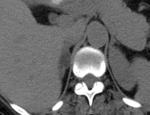
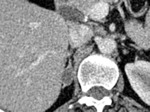
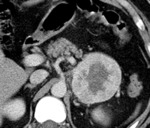
On unenhanced images (Figures 2 and 3),
heterogeneity is seen with larger masses.
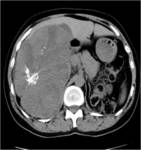
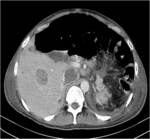
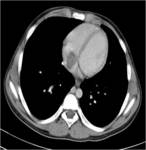
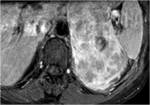
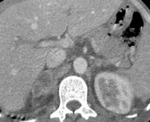
On contrast enhanced images (Figures 1 and 4),
the tumor shows heterogeneous enhancement,
with the greatest enhancement often at the periphery.
CT findings that increase the index of suspicion for adrenocortical carcinoma include the following:
-
Large mass (>4 to 5 cm)
- Sudden growth
-
Central necrosis or hemorrhage,
resulting in variable enhancement◦relative contrast retention (washout <40%) on delayed contrast-enhanced CT
-
Heterogeneous enhancement
-
Invasion into adjacent structures
-
Venous extension into the renal vein or inferior vena cava
- Calcification in some cases.
- Margin irregularity
CT can also demonstrate metastasis to lymph nodes,
lung,
bones and liver.
(Figures 5-7)
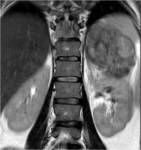
Magnetic resonance imaging (MRI) (Figures 10-13)
Occasionally,
differentiating an adrenal carcinoma from other pathology in the upper abdomen may be difficult because the mass is large and the fat planes are indistinct.
In these patients,
multiplanar magnetic resonance imaging (MRI) is the better imaging test.
MRI often demonstrates a large mass with lower signal intensity than the liver on T1-weighted images and higher signal intensity than the liver on T2-weighted images.
Often,
the tumor demonstrates heterogeneously hyperintensity on T1- and T2-weighted images,
due to the central necrosis and hemorrhage.
Because the mass usually does not contain any significant intracellular lipid,
it will not lose signal on out-of-phase imaging.
Coronal and sagittal images may be helpful in determining adrenal origin of the mass,
thus differentiating it from renal cell carcinoma or hepatocellular carcinoma,
especially if CT is equivocal.
MRI is advantageous for evaluating tumors,
since its depiction of vascular invasion and extension into surrounding structures often is superior to that of CT.
Additionally,
the most cephalad extension of the tumor must be evaluated so that the surgeon can obtain vascular control of the tumor.
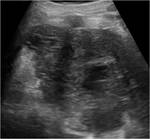
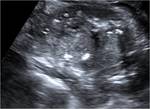
Ultrasonograghy
Adrenocortical carcinoma demonstrates a homogeneous echo texture when small,
but becomes heterogeneous with cystic areas when the tumor grows as a result of hemorrhage and necrosis.
(Figures 8 and 9)
It is helpful in some patients to determine the organ of origin of the mass.
Nuclear Imaging
It helps to exclude other lesions of adrenal origin.
Iodine-121 metaiodobenzylguanidine (MIBG) and indium-111 octreotide can be used to visualize pheochromocytomas,
while iodine-131 6-beta-iodomethyl-19-norcholesterol (NP-59) can be used to detect aldosteronomas or other hyperfunctioning cortical tumors.
Positron emission tomography imaging performed with fluorine-18 fluorodeoxyglucose (FDG) can be used for differentiating benign adrenal lesions from malignant lesions. FDG PET/CT has higher specificity to rule out suspected adrenocortical carcinoma (ACC) recurrences diagnosed by CT.
Therefore,
FDG PET/CT can play a significant role in patient management as a second-line modality in the postoperative surveillance of ACC patients after CT detection of a potential recurrence.
Angiography
Prior to cross-sectional imaging,
arteriography was the preferred modality for evaluating abdominal masses.
On angiograms,
adrenal carcinomas are usually hypovascular masses.
The predominant arterial supply to the adrenal gland and to adrenal carcinoma is the superior adrenal artery.
Percutaneous biopsy
With the new imaging modalities,
there is a decreasing need to perform percutaneous fine needle aspiration (FNA) or biopsy for definitive characterization.
Prior to FNA or biopsy, a clinical and laboratory assessment should be done to exclude the possibility of a pheochromocytoma as hypertensive crisis may be precipitated during the procedure.
Adrenal biopsies can be performed via a posterior approach with the patient in the prone position.
The lateral decubitus approach is also safe.
Non radiological investigations include:
- Twenty-four-hour urine test: to measure the amounts of cortisol or 17-ketosteroids.
- Low-dose dexamethasone suppression test.
- High-dose dexamethasone suppression test.
- Serum potassium,
sodium.
Differential diagnosis
• Metastases ( Fig 14 )
Lung carcinoma ,
breast carcinoma and melanoma are the common primary tumors.
A diagnosis of adrenal metastasis is important because the metastasis indicates inoperable stage IV disease (except in ipsilateral renal cancer).
Adrenal metastases have no specific imaging features.
•Adenoma ( Fig 15,
16 )
The most common tumor in the adrenal gland is the adenoma.
Adrenal adenomas have two properties that differentiate them from non-adenomas.
1.
70% of adenomas contain high intracellular fat (lipid-rich adenomas) and will be of low attenuation on unenhanced CT.
2.
Adenomas rapidly wash out contrast.
A density equal to or below 10 HU is considered diagnostic of adenoma.
Few adrenal adenomas do not contain enough intracellular lipid to have a density of less than 10 HU and cannot be differentiated from malignant masses on an unenhanced CT.
These adenomas are called lipid-poor.
On CECT,
most adenomas show mild enhancement,
while malignant tumors show strong enhancement
Adenomas can be differentiated from malignant masses on the basis of their fast wash-out of contrast.
Larger adrenal adenomas are radiologically similar to adrenal cortical carcinomas.
The pathologic distinction between adrenal adenoma and adrenal carcinoma is largely based on size.
•Adrenal haemorrhage
• Phaeochromocytoma ( Fig 17 )
Pheochromocytomas are paragangliomas arising from the adrenal medulla.
Usually,
they are larger than 3 cm at the time of detection.
They are highly vascular and larger tumors are prone to hemorrhage and necrosis,
even when they are benign.