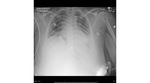
Acute Chest Syndrome: Vaso-occlusive crisis of the pulmonary vasculature commonly seen in people with sickle cell disease.
Will present in a patient with acute chest pain as a new opacification of the lung fields on a chest x-ray.
Other sequelae of sickle cell disease,
including rib enlargement,
cardiomegaly,
and bone infarcts can also be clues which point to chronicity.
The chest x-ray is usually diagnostic of this entity: a CT scan of the thorax may show a mosaic perfusion pattern which could also be associated with pulmonary edema and/or air trapping.
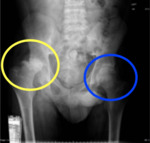
Osteonecrosis: Will usually begin as a vaso-occlusive crisis as a sudden onset of bone or visceral pain secondary to microvascular occlusion and/or ischemia.
Chronicity of these episodes will progress to bone infarction,
avascular necrosis,
and osteonecrosis.
This process has a predilection for portions of bone with inherently decreased vascular supply (e.g.
joints,
bone periphery).
A radiograph will usually be the first line of imaging,
which will show minor osteopenia,
followed by variable density.
Microfractures of the subchondral bone will accumulate as the bone loses its ability to repair leading to articular surface collapse.
The cortex will then collapse into fragments with superimposed degenerative changes.
Additional cross-sectional imaging,
such as MRI and nuclear medicine studies of the bone in question,
will be helpful to better characterize the degree of osteopenia,
especially in early osteonecrosis.
MRI is the most sensitive imaging modality (~95%) and will demonstrate chagnes long before radiographically evident.
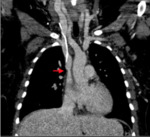
Venous Thromboembolism: Venous thromboembolism is more common in patients with sickle cell disease secondary to the inherent vaso-occlusive state.
Imaging for this clinical condition will depend on the presentation.
If pulmonary embolism is suspected,
usual clinical criterion will be applied and appropriate imaging tests will be performed,
including ultrasound and CT thorax C+.
Additionally,
sequelae of thromboembolism can develop in the sickle cell patient from the presence of chronically retained central lines.
Depending on the location of the central line,
alterante presentations of embolic change,
such as superior vena cava syndrome secondary to chronically retained superior vena cava catheter,
can occur.
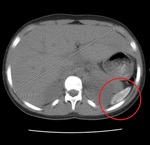
Splenic Sequestration Crisis: Splenic sequestration crisis will present as increasing abdominal pain and rapidly developing anemia in a young patient (almost always under the age of 5) with transient splenomegaly which can become so large that it fills the entire abdomen.
The pathology behind this is due to decreased flow of blood through the spleen due to the inherently sickled nature of the red blood cells.
The clinical presentation of acute abdominal pain with appropriate imaging tests (ultrasound and/or CT of the abdomen) will be diagnostic of the condition.
In patients who are older than the age of 5,
the spleen is usually absent.
Asymptomatic patients will usually have some degree of hepatomegaly and calcified gallstones.
A cholecystectomy is often times electively performed to help prevent acute cholecystitis.
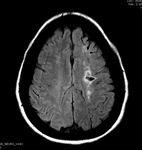
Ischemic Stroke: Due to its vaso-occlusive nature,
individuals with sickle cell disease will present with ischemic stroke at a younger age than the regular population.
It has been estimated that approximately 11% of children with sickle cell disease will have a stroke before the age of 14,
and without additional measures,
half of these patients will present with recurrent stroke in two years.
CT of the head and/or MRI of the brain can be performed in the acute setting to exclude ischemic stroke,
with MRI brain being more sensitive for acute ischemia than CT with its ability to use diffusion-weighted imaging in the hyperacute setting.
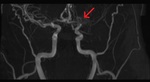
Neurovascular imaging with MRA or CTA should be acquired in all patients with sickle cell disease to look for large vessel disease and to exclude other causes for acute neurologic deficits.