ANATOMY
The scrotum is a sack of skin containing the testicles,
epididymis and part of the spermatic cords,
and it is divided in two parts by the perineal raphe.
The covering of the scrotum consists of at least six layers (from lower to greater depth): the skin,
dartos muscle,
external spermatic fascia,
cremaster layer,
internal spermatic fascia and tunica vaginalis.
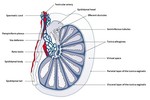
The contents of the scrotum are (Fig.
1):
- The testicles are two oval and symmetrical glands,
surrounded by the tunica albuginea.
They are composed of numerous seminiferous tubules separated by radiating septa that divide it into multiple lobules.
The septa converge posteriorly to form the central mediastinum testis,
which is an invagination of the tunica albuginea.
The seminiferous tubules join together to form the rete testis.
These tubules terminate in efferent ductules that drain into the epididymis and then into the vas deferens.
- The epididymis is an elongated structure situated posterolaterally to the testis.
It is composed of three parts: the head,
the body and the tail.
- The spermatic cord is a cylindrical complex originating from the posterior margin of the testis and terminating at the internal inguinal ring passing through the inguinal canal.
It contains a number of structures,
all enveloped by the spermatic fascia: the ductus deferens; the testicular,
cremasteric and deferential arteries; the pampiniform plexus of veins; and the nerves and lymphatic system of the testis.
- Epididymal and testicular appendages represent remnants of embryonic ducts.
The appendix testis (hydatid of Morgagni) is seen as an oval structure located between the epididymis and testis.
An appendix epididymis is an often-pedunculated structure arising from the epididymal head.
The scrotum and its contents are mainly irrigated by three arteries: the cremasteric,
the testicular and the deferential.
The venous drainage is done through the pampiniform plexus.
The scrotal lymphatics drain to the ipsilateral superficial inguinal lymph nodes.
Anastomotic connections to the lymphatics of the contralateral network across the median raphe exist.
The innervation of the scrotum is mainly carried out by: genital branch of genitofemoral nerve,
sympathetic nerves,
branches of the ilioinguinal nerve.
ULTRASOUND TECHNIQUE
Ultrasound is the main imaging method used to assess the scrotum.
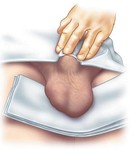
Patients are usually explored in supine decubitus.
A towel may be placed between the thighs to help hold the scrotum (Fig.
2).
The ultrasound study of the testicles should be performed with a high frequency linear probe (7-15 MHz),
as they are superficial organs.
In cases where the scrotum is increased in size,
it may be necessary to use low frequency convex probe (3-4 MHz).
Both testicles should be examined transversally and longitudinally,
comparing each testicle with the contralateral in terms of shape,
size,
echogenicity and vascularization in Doppler mode.
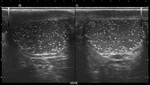
NORMAL SCROTAL ANATOMY ON ULTRASONOGRAPHY
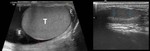
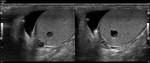
The normal scrotal ultrasound findings are (Fig.
3):
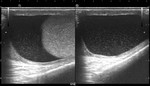
- The normal testicle measures approximately 5×3×2 cm (length × height × breadth) with a homogeneous,
intermediate echogenicity.
The septa are displayed as hypoechoic lines and the mediastinum testis as a hyperechoic linear structure.
The rete testis can be identified as a hypoechoic area adjacent to the mediastinum testis.
- The tunica albuginea is seen as a thin echogenic band outlining the testis.
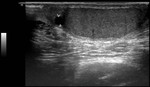
- The epididymis (5-7 cm) is shown as an isoechoic structure to the adjacent testicular tissue.
- The spermatic cord appears as a highly echogenic band within the inguinal canal.
- The appendix testis and epididymis appears isoechoic to testicular tissue.
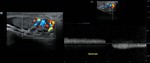
Doppler mode shows a pattern of low resistance in intratesticular and capsular arteries and low or high resistance in the extratesticular circulation.
ACUTE EDEMA AND SCROTAL PAIN
The ultrasound is very important in the study of acute edema and scrotal pain.
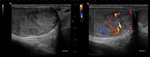
Testicular torsion
Complete absence of flow within the twisted testicle,
but with the presence of demonstrable flow in the asymptomatic contralateral testicle.
It is a surgical emergency: its repair within 6 hours has a chance of resolution without sequelae between 80-100% down to 20% after 12 hours.
Ultrasound findings:
- Early (4-6 hours): normal or decreased testicular echogenicity,
testicular swelling,
and reactive hydrocele.
- Late (24 hours): testicle presents heterogeneous echogenicity,
secondary to vascular congestion,
hemorrhage and infarction.
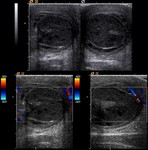
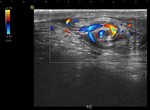
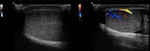
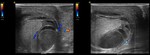
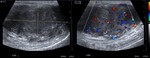
- Doppler mode: absence of unilateral intratesticular flow (Fig.
4).
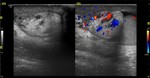
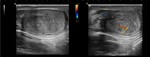
Another sign to know is the "whirlpool sign": it is highly specific of testicular torsion and is manifested as a spiral shaped doughnut seen with no flow or low flow if intermittent torsion (Fig.
5).
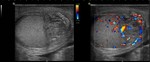
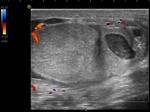
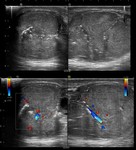
When the testicle is detorsionated,
it is observed: increased flow in and around the testicle simulating an epididymo-orchitis (Fig.
6).
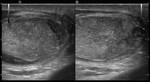
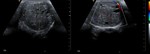
Torsion of testicular appendix
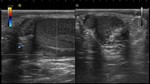
The common ultrasound finding is a hyperechoic mass with hypoechoic central area between the upper pole of the testicle and the head of the epididymis.
In Doppler mode it shows no color signal on the inside of the appendix,
demonstrating an increase in peripheral flow around the appendix and intratesticular normal flow (Fig.
7).
Epididymitis and epididymo-orchitis
It is the most common cause of acute scrotum.
The association of orchitis is due to the direct spread of infection to the testicular parenchyma (20-40%).
Ultrasound findings (Fig.
8):
- Focal or diffuse hypoechogenicity of the epididymis with increasing size.
Orchitis is manifested as an increase in the size of the testicle with a heterogeneous echogenicity.
- Increase of local or diffuse blood flow of the epididymis or testicle,
usually unilateral.
- Reactive hydrocele.
- Scrotal wall edema.
Complications:
- Segmental infarction: hypoechoic area of geographical margins with its vertex to the testicular mediastinum.
- Pyocele: complex hydroceles with loculations and partitions.
- Venous infarction: diastolic reverse-flow in the Doppler mode.
- Abscess (Fig.
9): heterogeneous lesions with irregular walls and internal echoes.
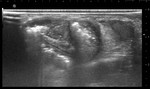
Funiculitis
It is the inflammation of the spermatic cord.
It often occurs along with epididymitis but can occur by itself as well.
On ultrasound,
cord structures appear thickened and echogenic with increased vascularity with associated reactive hydrocele (Fig.10).
TESTICULAR TRAUMA
Testicular trauma can manifest as fluid collections (hematocele,
hydrocele,
or hematoma),
testicular disruption (fracture or rupture) or vascular injury.
A discontinuity in the usual testicular parenchyma is considered a testicular fracture.
It is identified as a hypoechoic linear stripe within the testicle that does not demonstrate vascularity (Fig.
11).
Emergent surgical repair performed within 72 hours has a high testicular salvage rate (>80%).
Post-traumatic hematomas can be seen in intra or extratesticular locations.
Acute hematomas have a hyperechoic appearance on ultrasonography.
Over time,
the hematoma appears increasingly hypoechoic with potentially complex and cystic components.
Doppler ultrasonography demonstrates no flow within these lesions (Fig.
11).
Hematoceles are blood collections between the two layers of the tunica vaginalis,
which appear echogenic in the acute phase.
Older hematoceles appear more hypoechoic and may demonstrate fluid-fluid levels or septations (Fig.
12).
PALPABLE LESIONS AND INCIDENTAL FINDINGS
One of the main roles of ultrasound is the evaluation of the scrotal masses and to determine whether they are located inside or outside the testicle.
The vast majority of extratesticular lesions are benign,
but the intratesticular are very likely to be malignant.
It is also important to determine if the lesion is cystic or solid,
if it has internal vascularization in the Doppler mode,
and if it is palpable.
Testicular cyst
Simple cysts in the parenchyma of the testicle are usually incidental findings.
They are solitary,
anechoic,
well circumscribed,
round to oval lesions with increased through-transmission (Fig.
13).
Careful examination for solid or mural components is advised in order not to miss a potentially malignant cystic lesion.
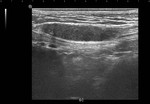
Epididymal cyst
Can occur anywhere within the epididymis and appear as well-circumscribed anechoic lesions (Fig.
14).
They can be multiple or bilateral,
being more frequent in the head.
Spermatocele
Retention cysts filled with non-viable sperm.
They are frequent after vasectomy,
epididymitis,
or inguinal herniorrhaphy.
Ultrasonographically they are indistinguishable from epididymal cysts (Fig.
14).
However,
spermatoceles tend to be larger in size and may present as a multilocular cystic lesion with internal echoes.
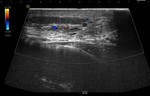
Varicocele
Dilation and tortuosity of the veins of the pampiniform plexus in the spermatic cord or epididymis.
It is the most frequent mass of the spermatic cord.
It can be idiopathic (incompetence of valves of the testicular veins) or secondary to an abdominal mass which compresses or invades the left renal vein or inferior vena cava.
In ultrasound it appears as multiple anechoic tubular structures,
serpiginous,
at the rear and upper edge of the testicle.
In Doppler mode,
there is slow flow at rest and an increase in diameter and of reverse flow during the Valsalva maneuver (Fig.
15).
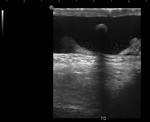
Hydrocele
Abnormal collection of fluid between the visceral and parietal layers of the tunica vaginalis and the most common cause of painless scrotal swelling.
Can be congenital or acquired.
Hydroceles present as anechoic fluid collections with increased through-transmission that surround the anterolateral aspect of the testicle (Fig.
16).
Microlithiasis
Are usually found incidentally.
Ultrasonography demonstrates intra-tubular calcifications of 2-3 mm in size as multiple,
non-shadowing small echogenic foci that are randomly distributed throughout the testicle (Fig.
17).
Current literature does not provide any proof that testicular microcalcifications can be regarded as a premalignant condition.
Scrotal pearls or scrotoliths
Are mobile calcifications in the scrotum that result from torsion of the appendix epididymis/appendix testis or reactive fibrous proliferation during intrascrotal inflammation.
On ultrasonography,
they appear as free-floating,
echogenic foci measuring up to 10 mm with posterior acoustic shadowing and are located outside the testicle (Fig.
18).
They have no clinical significance.
Vasectomy‐related changes
After a vasectomy,
there is a higher incidence of thickened epididymis (Fig.
19),
tubular ectasia of rete testis and spermatic granulomas.
Inguinoscrotal hernia
The scrotal sacs can accommodate intra-abdominal contents.
Ultrasound can demonstrate the presence of bowel or echogenic fat (Fig.
20).
Adenomatoid tumor
Is a benign neoplasm that most commonly arises from the epididymal tail.
Accounting for approximately 30% of extratesticular tumors,
it is the most common solid neoplasm of the epididymis.
Ultrasonography assessment reveals a well-circumscribed hypoechoic,
rounded mass with a usually homogeneous echotexture.
Germ cell tumors
Account for approximately 95% of all testicular tumors.
They are further divided into seminoma and non-seminomatous tumors.
Seminoma is the most frequent pure testicular tumor and represents up to 50% of germ cell tumors.
The average age at the time of diagnosis is 35-39 years.
The main ultrasound findings (Fig.
21):
- Are typically unilateral,
hypoechoic,
tend to be homogeneous and can be lobular or multinodular.
- Dense echogenic calcifications and cystic spaces are relatively uncommon.
- They are variable in size and in more than 50% of cases can be large enough to completely replace the normal testicle.
- In Doppler mode,
the tumor shows an increase in vascularization compared to the adjacent testicular parenchyma.
Among the non-seminomatous tumors,
embryonic carcinoma is the most frequent subtype,
being the second most frequent histological type of testicular tumor after seminoma.
It is present in 80% of the mixed tumors,
but in its pure form it represents only 2-3%.
It affects patients between the ages of 25 and 35.
By ultrasound,
this type of tumors are heterogeneous and cystic masses with irregular margins.
Echogenic foci within the mass may be seen,
which can represent calcification,
hemorrhage,
or fibrosis (Fig.
22,
23 and 24).
The tumor may present with increased vascularity mimicking acute testicular inflammation.
Sex cord stromal tumors
They are rare neoplasms that account for only 5% of testicular tumors.
They are typically benign,
although malignant cases have been reported.
The clinical features that are distinguished are the early presentation age and the symptoms related to the hormones they secrete,
such as precocious puberty or gynecomastia.
In ultrasound they may present the same characteristics as seminoma:
- Leydig cell tumor: hypoechoic nodule.
- Sertoli cell tumor: variable appearance,
being able to appear as multicystic lesions or diffuse increase of the testicular echogenicity.
Lymphoma
It is the most common testicular neoplasia in men over 60 years of age.
Most are diffuse large-cell lymphomas B.
They constitute 1%-9% of all testicular neoplasms and 1% of non-Hodgkin's lymphomas.
It is the most common bilateral testicular neoplasia,
with a general prevalence of synchronous affectation close to 20%.
Testicular tumor may be the primary manifestation of lymphoma or most often occurs secondarily.
It is generally painless,
which allows clinical differentiation with epididymo-orchitis.
Findings in ultrasound: hypoechoic and hypervascular lesion,
similar to seminoma and epididymo-orchitis (Fig.
25).
Metastasis
Although it is uncommon,
a variety of primary tumors can metastasize to the testicles.
The most common primary malignancy with dissemination to the testicle is the adenocarcinoma of prostate,
which represents 35% of the cases.
The appearance in imaging of testicular metastasis is non-specific and can overlap with the seminoma.
The epidemiological factors may help in the diagnosis:
- Older presentation (approximately 55 years).
- They usually occur in the context of an advanced metastatic disease.
- Most metastases are unilateral (bilateral in up to 15% of patients).
NO PALPABLE TESTES
Cryptorchidism
It is the partial or complete failure of descent of the intra-abdominal testis to the scrotal sac.
The testicle can be found at any level in its descent,
being the inguinal canal the most frequent place.
It can be associated with complications like increased risk of malignant degeneration,
infertility and torsion.
Ultrasonographically,
it appears as a rounded or ovoidea hypoechoic structure and smaller than the normal testis (Fig.
26).
Testicular atrophy
It can be congenital or acquired.
It is usually bilateral,
although it may be unilateral.
In the ultrasound the testicle is significantly smaller than the contralateral with variable echogenic pattern (Fig.
27).