A well-taken history is necessary for finding etiological causes of nodular changes including professional (pneumoconiosis) history,
and clinical and laboratory data.
When interpreting the X ray image,
pay attention to the possible enlargement of the lymph nodes of the hilum and the mediastinum (unilateral,
bilateral),
pleural reaction,
changes in heart size,
and configuration of the arteries of the heart-shaped shadow.
HRCT - crucial for definitive diagnosis,
precise information on nodules (intensity,
distribution),
interstitial,
parenchyma.
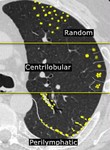
CT distribution of the nodules on the basis of the part of the acinus (lobulus) that they encounter (Fig.
2):
1) Centrilobular distribution
Nodules are limited to the centrilobular region.
Unlike perilymphatic and random nodules,
centrilobular nodules spare the pleural surfaces.
The most peripheral nodules are centered 5-10mm from fissures or the pleural surface
a) Clear nodules (Silicosis / CWP)

Fig. 3

Fig. 4
b) Tree-in-bud (TBC,
aspiration)

Fig. 13

Fig. 6
c) Ground glass nodules
Diffuse pattern is shown in pneumonia,
edema,
alveolitis
Singular pattern is seen in early stages of lung adenocarcinoma (ground glass nodule)

Fig. 7

Fig. 8
2) Perilimphatic distribution (Sarcoidosis,
lymphangitis)
In patients with a perilymphatic distribution,
nodules are seen in relation to pleural surfaces,
interlobular septa and the peribronchovascular interstitium.
Nodules are almost always visible in a subpleural location,
particularly in relation to the fissures.

Fig. 9

Fig. 12
3) Randomly distributed (Histoplasmosis,
metastasis)
Nodules are randomly distributed relative to structures of the lung and secondary lobule.
Nodules can usually be seen to involve the pleural surfaces and fissures,
but lack the subpleural predominance often seen in patients with a perilymphatic distribution.
Coronal sections are good to show random distribution of nodules.

Fig. 10

Fig. 11