Patient positioning:
The patient should be in supine position with the bed elevated around 30º.
A low-frequency transducer (2.5-5.0 MHz) is used to identify the abdominal aorta and renal arteries.
The important views “Money views” are: oblique view through the liver for the right renal artery,
lateral decubitus for the left renal artery.
Also,
the anterior approach is used to evaluate the main RA,
in selected cases the posterior approach can be used.
Parameters adjustment:
Doppler gain should be adjusted by increasing the gain to a level just before occurrence of color artifact in adjacent structures.
The pulse repetition frequency (PRF),
or velocity scale,
is the frequency of sampling; under-sampling may underestimate peak velocities.
Doppler gate must include the whole artery lumen and angled with the direction of flow.
The insonation angle must be maintained at 60º or less.
Findings:
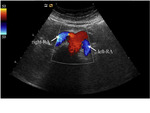
The RAs arise from the lateral sides of the aorta (Fig.
1), usually 1-2 cm below the superior mesenteric artery origin.
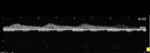
Normally,
the main renal artery shows a low resistance waveform (Fig.
2),
and the peak systolic velocity (PSV) in the main RA and its branches should be lower than 120 cm/s.
.
A resistive index (RI) value of 0.7 is used to differentiate between normal and pathologic resistance to flow.
Intrinsic renal diseases (i.e.
nephro-angiosclerosis,
hypertension,
tubular interstitial disease,
diabetes mellitus,
and severe bradycardia) can cause an increase of RI,
even in the presence of normal serum creatinine levels.
Renal/aortic ratio (RAR) identified as: the comparison of PSV values obtained in the prerenal abdominal aorta with those measured in the RAs.
In normal conditions,
RAR is lower than 3.5.
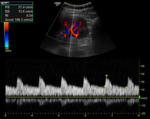
It is thought that the best signals for evaluation are obtained at the level of the large segmental or interlobar arteries as they course directly towards the transducer.(Fig.
3)
Doppler criteria for diagnosis of RAS
Doppler US criteria of RAS can be divided into two groups;
1-Direct criteria (findings obtained at the level of the stenosis)
2-Indirect criteria (alterations observed in waveform acquired at the renal vasculature distal to the site of stenosis).
Direct criteria
Four criteria are used to diagnose significant proximal stenosis or occlusion of the RA.
1-A peak systolic velocity (PSV) greater than 200 cm/s is considered the threshold for Doppler diagnosis of 60% stenosis.
2-RAR of 3.5 or greater identified hemodynamically significant lesions.
3-Identification of RAs with no detectable Doppler signal.
4-Detection of aliasing artifacts at the stenosic area and the presence of turbulence at Doppler interrogation.
Indirect criteria (distal waveform alterations)
1-Loss of early systolic peak
2-Acceleration index (AI) lowers than 3 m/sec
3-Acceleration time (AT) < 0.07 sec
4-A difference between the kidneys in RI > 5% or in pulsatility index >0.12).
These changes causes the famous ‘‘tardus-parvus’’ effect.
Tardus means slow and delayed,
while parvus means small.
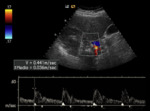
Tardus indicate that systolic acceleration of the waveform is slow with consequent increase in time to reach the systolic peak.
Parvus refers to the fact that the systolic peak is of small height,
indicating a slow velocity (Fig.
4).
Indirect signs are non-specific as multiple extrarenal factors affect systolic acceleration such as aortic and mitral valvular diseases,
left ventricular dysfunction or even cardiovascular medication.
Consequently,
these criteria are used only when obvious on spectral traces or when quantifying the stenosis as severe (> 75%).
It is recommended to use of a combination of intra and extrarenal parameters,
as it results in increase in the overall sensitivity and specificity.
Evaluation in assessing restenosis of renal artery stents
Assessment of restenosis of RA stents is important to assess the long-term benefits of the procedure.
MRA and spiral CTA are not suitable for assessing restenosis due to artifacts caused by the stent material.
In-stent PSV >180 cm/s is considered the threshold value for diagnosis of restenosis.
RAR is of less value in this situation.
It is advised to look for alterations in Doppler waveforms in areas of renal vasculature distal to a stenosis,
instead of directly insonating the RA.
Diagnosis of renal vein thrombosis
In early stages of renal vein thrombosis (RVT),
intrarenal and renal venous flow and pulsatility may be absent and renal arterial diastolic flow may be reversed with elevated RI.
But,
in the early few days after the occurrence of RVT,
some retraction of the thrombus occurs and venous collaterals develop at the renal hilum which allow some venous flow to but the flow would be monophasic with no pulsations.