Retinoblastoma is the most common paediatric intraocular tumour.
It usually presents as leukocoria and strabismus in children between 1-5 years of age.
Around 47-58 percent of leukocoria cases in children are due to retinoblastoma,
making it the leading cause of white pupillary reflex1.
Though retinoblastoma is a life-threatening disease,
it is curable with early diagnosis and appropriate treatment.
Establishing the best management of retinoblastoma and differentiating it from other causes of leukocoria is imperative for preservation of visual function.
Persistent Hyperplastic Primary Vitreous (PHPV) is the second most common cause of leukocoria1,
2making it an important differential to rule out.
PHPV is a congenital disorder occurring due to abnormal persistence of foetal intraocular vessels in the anterior or posterior segments of the eye.
Primary vitreous forms around the 7th week of gestation and starts involuting during the 20th week and almost always disappears at the time of birth.
Failure of regression of primary vitreous results in PHPV and associated complications like vitreal haemorrhage,
vitreal and retinal detachments3.
While histopathology remains the gold standard for diagnosis and evaluation of high risk features of retinoblastoma,
imaging studies are the non-invasive means of establishing diagnosis and planning treatment for patients presenting with leukocoria4.
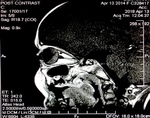
MRI is the investigation of choice when evaluating patients with suspected retinoblastoma; it is indicated in evaluation of all ocular tumours.
The tumour mass usually appears hyperintense to vitreous on T1 and hypointense to vitreous on T2 weighted sequences and shows significant post-contrast enhancement.
Details provided by MRI can also be useful in mapping a treatment plan.
However,
calcifications and lesions less than 2mm have been inconsistently detected on MRI5.
MRI can also be used for the diagnosis of PHPV where a hyperintense retrolental membrane,
tubular hyaloids vessels,
retinal detachment and microphthalmia provide clues for diagnosis6,7.
If a triangular retrolental vascular mass with a central stalk of hyaloid artery remnant connected to the optic disc is seen in the vitreous,
PHPV should be the top most differential.
The overall shape of PHPV has been likened to a martini glass3. The closest differential of PHPV is retinal detachment but,
in the latter,
there is a hyperintense band extending from optic disc to ora-serrata rather than to posterior surface of lens3.
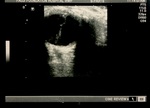
Ultrasound is the ideal imaging modality for ophthalmological pathologies due to the superficial and fluid filled nature of the eye.
It provides painless,
radiation free imaging that does not require general anaesthesia.
Ultrasound is a diagnostic aid when there is restriction of fundoscopic examination due to cataracts and hyphema4.
Retinoblastoma is visualized as an echogenic soft-tissue mass that contains calcification5.
Approximately 95 percent tumours show histological evidence of calcification.
It is the main feature that differentiates retinoblastoma from other causes of leukocoria4.
Calcification is also important in differentiating retinoblastoma from other tumours in children and ultrasound has been shown to identify 92-95 percent of calcifications that are present histologically8,9.
Colour Doppler can be used to determine the vascularity of the tumour.
It is useful in distinguishing retinoblastoma from PHPV which shows characteristic retrolental membrane that may have persistent patent hyaloid artery and may also have features of retinal detachment along with vitreous hemorrhage10.Tumor seeding and optic nerve involvement have also been reported to have been detected by ultrasound11.
In a case report,
it was seen that ultrasound can be used in detecting PHPV in antenatal scans as well.
Two cases were reported in which bilateral PHPV was diagnosed in foetuses in early third trimester.
The ultrasound findings were comparable to post-natal scans with retinal detachments and echogenic membranes extending from posterior part of lens to the posterior pole of eyeball12.
This study aims to determine the diagnostic accuracy of ultrasound in differentiating retinoblastoma from PHPV taking MRI as gold standard in order to explore the possibility of utilizing ultrasound as a cost-effective screening tool in children presenting with leukocoria.