The study included 67 women between the ages of 55 and 94 years old (mean: 83,8 years; median: 85 years) who were diagnosed with hormone-receptor positive breast cancer (53,1 % Luminal A and 46,9% Luminal B).
The diagnosis was made with core needle biopsy guided with sonography in the vast majority of cases.
Ductal carcinoma was the most frequent histologic type,
as it is in younger women,
but it has been seen some characteristics more related to breast cancer in old patients,
higher rates of hormone receptor expression and lower rates of HER-2 expression.
[2,3]
Neoadjuvant chemotherapy,
hormone therapy followed by surgery or surgery alone are the standard treatment in early stages of breast cancer[4].
Age is a not sufficient criteria to exclude any of this treatment options.
It is true that in many cases age is associated with high prevalence of comorbidities,
reduced tolerance to physiologic stress,
reduced social support and frailty but these conditions are not always present.
As it is recommended,
each patient has undergone a pre-treatment evaluation,
in which we evaluated the factors that could take a role in the toleration of surgery or chemotherapy,
which could change the risk-benefit balance [5,6].
There are some tools to evaluate this frailty,
such as the one given in the cardiovascular health study index or the comprehensive geriatric assessment in cancer patients (CGS),
but there is not a standard.
When,
after the evaluation,
surgery and chemotherapy were thought to be riskier than beneficial,
primary endocrine therapy was the best alternative.
Additionally,
patients that present low recurrence risk [7] can benefit from the use of this kind of treatment.
This can be due to the subtype of breast cancer they have or their age.
Patients have been undergoing hormone therapy as an alternative primary treatment.
Letrozole was the most used treatment (41/67: 61,2%),
followed by tamoxifen (12/67:18%),
anastrozole (11/67: 16,3%) and exemetastane (3/67: 4,5%).
Aromatase inhibitors were more often given than tamoxifen in older women because of its benefit in adjuvant setting.
There is a higher risk of bone fracture and cardiovascular risk when taking aromatase inhibitors,
so we avoided them when heart or bone disease were known.
[8,9]
All women have been mammographically and ultrasonographically controlled,
at least every 6 months.
The follow-up lasted an average of 2,75 years,
with a maximum of 8,9 years.
In this period of time,
42 patients experienced shrinkage of their tumour size,
being this shrinkage more that 50 % in 24 of them.
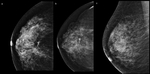
In Figure 1 we can see the evolution of one of this patients during the follow-up,
being a the mammogram at the diagnosis,
b the one after 12 and c after 18 months of treatment with hormone therapy treatment.
We can see the disappearance of the tumor at 24 months.
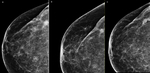
6 were stable from a radiological point of view,
as seen in Figure 2 a case with the mammograms at the diagnosis (a),
after 12 (b) and 24 (c) months,
where we can see that the tumour has remained without change.
Tumour growth only occurred in 9 women.
Additional treatment,
such as surgery or radiotherapy,
was only necessary in 7 of our patients.
Pharmacotherapy was changed in 4 cases,
not because of bad radiological tumour evolution but for intolerance to the initial drug.
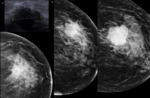
In Figure 3we have the case of one of our patients that required surgery as we see in the mammograms and sonography,
the tumour was not controlled with hormone therapy and it kept growing,
being b and c te studies after 12 and 18 months,
so surgery was decided.
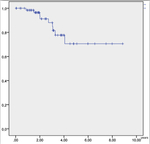
Survival analysis was also considered,
surveying it with help of the Kaplan Meier estimator (Figure 4).
Considering all cases,
the rate of survival after a year of follow-up using hormone therapy as treatment was 98,4%,
at two years 96 % and after five years was around 70%.
If the cases were sorted according to the pathology results,
we have 56 cases of infiltrative ductal cancer and 11 of other types of breast cancer,
including the lobular infiltrating kind.
From the initial group of 67 patients,
56 are still alive nowadays.
The youngest woman of the nine deceased,
was 79 years old,
all others were above the life expectancy in our country (82 years for women) and just two of them have had experienced tumour progression.
Considering our study,
we have to take into account that the value of survival estimation can be not totally accurate as we are studying people of age that could not or would not be subject to surgery as well as it is proven that breast cancer in this sort of patients does not entirely lead to death [2].