Fourteen of the 32 patients included in our study underwent anterior resection of the rectum and 15/32 abdominoperineal resection.
Three patients were monitored with endoscopy and concomitant biopsy and underwent FU with MRI investigation every 3-6 months for the first year and then annually.
The mean time between the end of neoadjuvant therapy and restaging MR imaging was 53.4 days (range: 38-82 days) and the mean time between the post-CRT MR imaging and surgery (or biopsy) was 21.2 days (range: 2-60 days).
Pathologic examination revealed 32/33 rectal adenocarcinoma and 1/33 mucinous type adenocarcinoma (32 patients,
one with a double synchronous lesion).
The histopathological examination provided the following results: 4/33 lesions were considered G0,
13/33 as G1,
7/33 as G2,
2/33 as G3 and 7/33 as G4 (4/7 with histopathological examination of the surgical specimen and 3/7 evaluated on the biopsy material); the CR group is therefore composed of 7/33 patients and the n-CR group of 26/33 patients.
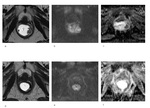
A statistically significant (P <0.0001) reduction of median tumor volume of both VT2and VDWIpre- vs.
post-CRT was noted for all 33 lesions included in the study,
respectively from 26.4 cm³ to 11.4 cm³ and from 14.8 cm³ to 5.3 cm³ (Table 1).
The pre- and post-CRT median tumor volumes of CR group were significantly lower compared to n-CR group,
both on T2-weighted images (VT2pre-CRT: 16.1cm³vs.
29.97 cm³,
P = 0.0037; VT2post-CRT : 1.3 cm³ vs.
14.3 cm³,
P = 0.001) and on DWI (VDWIpre-CRT: 6.6 cm³ vs.
17.99 cm³,
P = 0.008; VDWIpost-CRT: 0.00 cm³vs.
8.7 cm³,
P = 0.0001) (Table 1).The ΔV% was significantly higher in CR group compared to n-CR group,
both in T2-weighted images (ΔVT2%: 84.9% vs.
50.7%,
P = 0.005) and in DWI (ΔVDWI%: 100% vs.
43.7%,
P = 0.0001) (Table 1).
Forthe 33 lesions included in the study a significant increase in median ADC value post- vs.
pre-CRT (1.47 ± 0.27 x 10-³mm²/sec vs.1.11 ± 0.29 x 10-³mm²/sec,
P = 0.0001),
expressed by the value ΔADC% (24.5%),
was found.
Nevertheless,
no statistically significant difference was found between median ADC values pre-CRT (P = 0.8),
post-CRT (P = 0.7) and ΔADC% (P = 0.4) in the CR group compared to the n-CR group (Table 1).
The ROC curves were used to compare the diagnostic performances of VT2and ΔVT2%,
of VDWIand ΔVDWI%,
as well as the ADC values and the ΔADC% (Table 2,
Fig.
2).
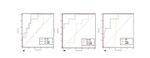
The AUC for the above values pre/post-CRT was respectively 0.86/0.91 for VT2,
0.82/1 for the VDWIand 0.53/0.54 for ADC.
A significantly greater accuracy was documented for VT2and VDWIvs.
the ADC values,
pre- and post-CRT; nevertheless there were no significant differences in AUC among VT2and VDWI(Table 2,
Fig.
2a,b).
The results for AUC of ΔVT2% (0.84) and ΔVDWI% (1) were significantly better than AUC of ΔADC% (0.58) (Table 2,
Fig.
2c),
without statistically significant differences between the ΔVT2% and ΔVDWI%.
In the absence of significant differences between VT2and VDWI,
(pre- and post-CRT) andΔV%,
the more accurate parameters for the assessment of CR (AUC = 1) wererepresented by the VDWIpost-CRT and ΔVDWI%.
We correctly identified as CR 6/7 lesions on the basis of the absence of SI on DWI on high b-value.
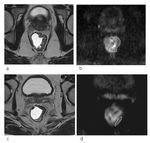
One false negative (FN) was documented: on the post-CRT DW images a focal area of high SI at the location of primary tumor was misinterpreted as residual tumor; histopathological examination revealed the complete absence of malignant epithelial cells in the presence of diffuse fibrosis enclosing mucin pools (Fig.
3).
The VDWIpost-CRT and ΔVDWI% of FN were,
respectively,
0.5 cm3 and94.2%; these values hang outward the range of VDWIpost-CRT and ΔVDWI% of n-CR patients (Table 1); moreover,
no overlap was found in comparison to the 2/33 lesions of the G3 group (VDWIpost: 5.28-21.69 cm3; ΔVDWI%: 32.5- 41.7%).