Non-neoplastic lesions
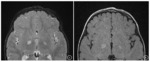
Dysplastic white matter lesions are zones of myelin vacuolization histopathologically (Fig.1).
- They are characterized as multifocal hyperintensities on T2W/FLAIR images and also called as “focal areas of signal intensity (FASI)”.
- They do not enhance following contrast administration.
- These areas are commonly seen in the basal ganglia (especially in the globi pallidi),
cerebellar white matter,
thalamus and brainstem.
- They do not cause a mass effect.
Usually,
these foci regress in the 20s and disappear eventually [2].
Bone dysplasias occur in the skull,
spine and long bones. Sphenoid wing dysplasia is a characteristic feature of NF1 due to hypoplasia/dysplasia of the greater sphenoid wing,
posterosuperior orbital wall defect.
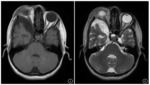
An enlarged middle cranial fossa may be seen (Fig.2).
Middle cranial fossa contents may protrude into the orbit and cause proptosis [2].
Buphthalmos is another imaging finding that may be seen in patients with NF1.
It is diffuse enlargement of the ocular globe with increased anteroposterior diameter.
It is caused by increased intraocular pressure secondary to obstruction of the canal of Schlemm,
which is located between the cornea and iris and provides resorption of the aqueous humor [3]. In NF1,
abnormal mesodermal tissue causes obstruction of this canal.
Differential diagnosis includes congenital or infantile glaucoma.
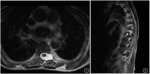
Dural ectasia refers to dilatation of the dural sac (Fig.3).
It may be a consequence of underlying bone weakness and associated with dystrophic skeletal changes leading to spinal instability and deformity.
Dural ectasia may cause dilatation of the optic nerve sheath and Meckel cave [1].
Dural ectasia or neurofibromas may cause posterior vertebral scalloping which is common in NF1 and characterized by the concavity of the posterior aspects of the vertebral bodies.
It is best seen in the sagittal plane [4].
Dystrophic bone changes include thinning of the vertebral pedicles,
transverse processes,
and laminas.
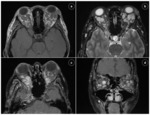
Neural foramina may also be expanded because of dumbbell neurofibromas (Fig.4).
Dumbbell neurofibroma is a tumor which has contiguous components in both neural foramen and paravertebral space.
Coronal plane with STIR sequence is the imaging modality of choice.
The differential diagnosis includes meningocele [4].
Although the most NF1-associated vascular lesions are extracranial (such as renal artery stenosis,
aortic coarctation or aneurysmal dilatations of the great vessels),
there can also be intracranial vascular involvement (Fig.5).
The most common type of intracerebral vascular involvement is intimal fibrosis of the supraclinoid internal carotid arteries,
which causes progressive stenosis resulting in a moya moya pattern [1].
Intracranial aneurysms and arteriovenous fistulas may rarely occur.
Even though they’re mostly asymptomatic in terms of cerebrovascular disease,
the risk of both ischemic and hemorrhagic stroke is increased in these patients,
so early detection is important [5].
MR angiography (MRA) and susceptibility-weighted imaging (SWI) sequences are helpful to evaluate.
Neoplastic Lesions
Neurofibromas are benign peripheral nerve sheath tumors.
Even though they consist mainly of Schwann cells,
unlike schwannomas,
they are inseparable from the nerve,
and surgical excision may result in adjacent nerve damage [6].
Neurofibromas can be specified in two types:
Cutaneous neurofibromas can be solitary or multifocal.
- They are often round or ovoid shaped (Fig.6).
- They may be diffuse or localized,
the latter being more common.
- Diffuse cutaneous neurofibromas are more frequent in children and young adults and often involve the subcutaneous tissue of the head and neck.
- Cutaneous neurofibromas are hypointense to the brain on T1W and hyperintense on T2W images.
- Strong but heterogeneous enhancement following contrast administration is typical.
Plexiform neurofibromas (PNFs) are pathognomonic for NF1.
- They are diffusely infiltrating,
large-bulky tumors which may be both deep and superficial (Fig.7).
- Superficial plexiform neurofibromas are more common than the deep ones.
- They are often located through a major nerve distribution.
- They often extend through the scalp and head and neck spaces such as pterygopalatine fossa,
buccal space and masticator space (Fig.8).
- An imaging finding called “target sign” is common,
which is characterized by a hyperintense rim and a relatively hypointense center due to central collagenous stroma on T2W images (Fig.8) [2].
- PNFs enhance strongly and have a typical appearance as "bag of worms” [1].
Gliomas
- Gliomas tend to occur at younger ages and be multicentric in patients with NF1,
compared to sporadic cases.
- They are most commonly seen in cerebellum and brainstem.
- Astrocytomas are the major type of gliomas in NF1,
and pilocytic astrocytoma (WHO grade I) is the main histological subtype [7].
The most common type of glioma in patients with NF1 is the optic pathway glioma (OPG).
- OPGs are characterized by unilateral or bilateral enlarged optic nerves (Fig.9).
This enlargement can be diffuse,
fusiform or lobulated.
- On T2W images,
there is a centrally high and peripherally low signal in the optic nerve.
Enhancement is variable on T1C+ images.
- A glioma in the optic nerve may extend to the optic chiasm,
hypothalamus,
optic tracts or adjacent structures such as temporal lobes,
cerebral peduncles and brainstem [1].
Patients may present with vision loss or visual field defects.
It is crucial to detect these tumors in the early stage,
especially in children.
- Fat-suppressed contrast-enhanced thin-slice MRI sequences must be the modality of choice for the lesions in the orbit.
- While optic chiasm is better evaluated in coronal plane,
axial plane is preferred for the optic nerves [8].
Brainstem gliomas are the most-frequent non-optic gliomas in NF1 and they are typically indolent.
20% of them are malignant (WHO grades II-IV) such as diffusely infiltrating fibrillary astrocytoma,
anaplastic astrocytoma,
and glioblastoma [1].
Tectal gliomas can cause stenosis of the cerebral aqueduct and result in obstructive hydrocephalus [8].
Malignant Peripheral Nerve Sheath Tumors (MPNSTs) are aggressive tumors with poor prognosis.
- They may arise from plexiform neurofibromas,
de novo or secondary to radiation therapy.
- They most commonly occur in the deep soft tissues,
usually close to a nerve trunk (Fig.10).
- Clinical presentation depends on the lesion’s location.
Pain is the most common symptom.
Neurological deficits may be seen due to damage or compression of the nerve [9].
When an MPNST arises from a plexiform neurofibroma,
it may be difficult to differentiate.
Rapid growth in follow-up studies,
heterogeneous signal intensity,
intratumoral cysts,
and perilesional edema are the features suggesting the MPNST diagnosis. F-18 FDG PET/CT may be helpful in distinguishing benign tumors from MPNSTs [1].