ANTINEOPLASTIC DRUGS
Antineoplastic drugs can be used in combination with each other and the side effects affect multiple districts and organs both during the treatment and years after the end of therapy (tab.1).
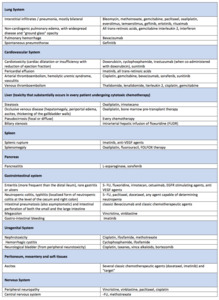
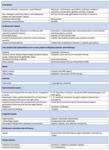
Table 1: List of the most frequent side effects of chemotherapy, classic and "target", divided by drugs and organs (not exhaustive). Adapted from: CT findings of chemotherapy-induced toxicity, Torrisi et al., Radiology. 2011;258(1): 41-56.
References: CT findings of chemotherapy-induced toxicity, Torrisi et al., Radiology. 2011;258(1): 41-56.
- Pulmonary adverse effects
The pulmonary system is among the most frequently involved in the toxicity linked to oncological therapies,
both from classical and molecular chemotherapeutic drugs (the most frequent are bleomycin,
methotrexate,
gefitinib),
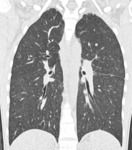
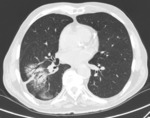
which can cause interstitial/ hypersensitivity pneumonitis (fig.1),
pulmonary hemorrhage,
ARDS and pleural effusion,
which may be more or less clinically evident,
often with dyspnoea.
The pulmonary thickening and interstitial infiltrates with subsequent development of fibrosis,
more often bilateral,
are the typical radiological images that should not be mistaken for disease progression,
inflammatory or cardiogenic pathology.
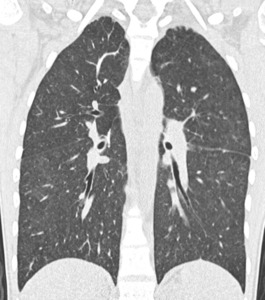
Fig. 1: 24-year-old Patient with Hodgkin's sclero-nodular lymphoma sc II.
NSIP CT pattern related to bleomycin administration.
- Abdominal adverse effects
In the abdominal area,
one of the most organs involved by drug related toxicity is the liver,
especially if the patient is treated with classical cytotoxic drugs.
Focal or diffuse hepatic steatosis (CASH,
"chemotherapy associated steatohepatitis") is frequently observed,
and this may reduce the functional reserve of the organ,
preventing resection in patients with metastases from colorectal adenocarcinoma.
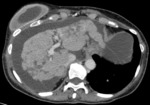
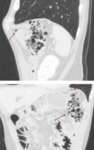
Chemotherapeutic drugs are also related to the development of pseudocirrosis (fig.2) (with rapid evolution even in 1-3 months,
frequently found in patients undergoing chemotherapy for breast cancer),
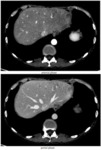
biliary sclerosis and veno-occlusive disease (fig.
3).
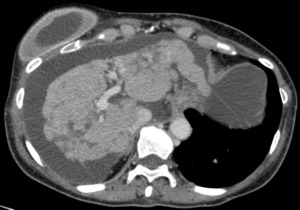
Fig. 2: 67-year-old Patient affected by breast adenocarcinoma, treated with multiple lines of chemotherapy; last cycles with Gemcitabine.
CT shows pseudocirrosis with ascites.
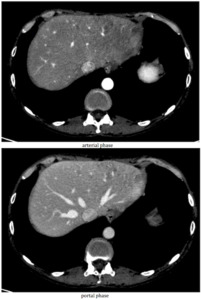
Fig. 3: 64-year-old Patient affected by uterine carcinoma, IV stage FIGO, undergoing radical surgery and chemotherapy (paclitaxel + carboplatin). CT shows hepatic sinusoidal occlusive syndrome.
The bowel is another site frequently subject to toxicity,
especially after the administration of chemotherapeutic drugs with development of: enteritis (widespread or more frequently with prevalent involvement of distal ileum),
neutropenic colitis,
typhlitis (localized form of neutropenic colitis limited to the cecum and to the right colon),
pseudomembranous colitis,
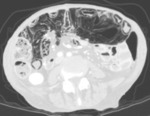
intestinal pneumatosis (which can be asymptomatic) (fig.4),
perforation (infrequent,
associated with bevacizumab) (fig.5),
subocclusion and bleeding.
Gastritis and duodenitis are observed less commonly.
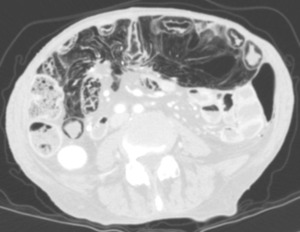
Fig. 4: An 80-year-old Patient with advanced adenocarcinoma of sigma and pulmonary and hepatic metastases, subjected to multiple lines of chemotherapy (the last one cetuximab).
Routine staging CT shows important intestinal pneumatosis, in an asymptomatic subject.
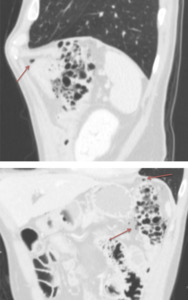
Fig. 5: 59-year-old Patient with T lymphoma treated with Cyclophosphamide, Doxorubicin and Vincristine.
CT imaging of mild pneumatosis of the left colonic flexure, with air bubbles (arrows) in the peritoneal cavity, compatible with perforation.
Less frequently are toxicity to the spleen (splenomegaly,
rupture,
atrophy),
pancreas (pancreatitis,
associated more frequently with the administration of L-asparaginase in the treatment of leukemia),
urogenital system (eg renal insufficiency related to cisplatin,
ifosfamide and methotrexate,
hemorrhagic cystitis,
rarely neurological bladder).
- Cardiovascular adverse effects
Toxicity to the cardiovascular system is expressed as a consequence of vascular toxicity with cardiopathies and radiological evidence of cardiac dilatation and pericardial effusion,
hypertension with subsequent cerebral hemorrhages,
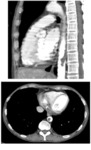
venous/arterial thrombosis and vasculitis (fig.6).
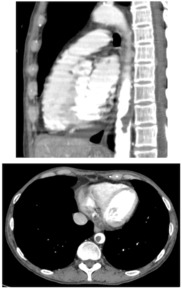
Fig. 6: The same 64-year-old Patient (in figure 2) affected by uterine carcinoma, IV stage FIGO, undergoing radical surgery and chemotherapy (paclitaxel + carboplatin). CT shows also the presence of a floating thrombus in thoracic aorta.
Both classic chemotherapies and target therapies may be associated with the appearance of ascites.
Its only appereance does not indicate disease progression,
but simple fluid retention.
RADIATION SIDE EFFECTS
For assessing radiation damage (tab.
2),
it is essential to know the location and the dose administered.
Acute irradiation toxicity occurs within 3 months after therapy,
and this is a precursor of the chronic effects typically occurring between 6 months and 1 year after treatment and may cause fibrotic phenomena in the treated areas.

Table 2: Main post-radiotherapy complications divided by irradiated organ.
In the thoracic area,
pulmonary fibrosis,
actinic pneumonia,
esophageal dysmotility,
and pericardial effusion can be seen (fig.7).
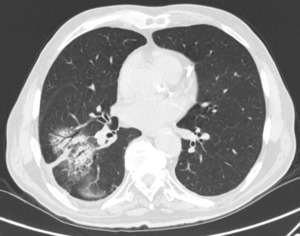
Fig. 7: 84-year-old Patient affected by renal cell carcinoma with a radiotreated pulmonary metastasis.
CT imaging compatible with parenchymal consolidation after 4 months from treatment.
In the abdominal area,
for example,
intestinal strictures,
post-actinic hepatitis,
pancreatic atrophy and nephritis may develop.
Radiation damage also affects the nervous system (the most frequent example is the brachial plexus neuropathy); in the skeleton,
the irradiated bone undergoes osteopenia and demineralization with consequent pathological fractures,
osteoradionecrosis,
findings not to be confused with metastasis.
Finally,
the risk of the occurrence of secondary neoplasms (eg post-actin sarcomas) is increased.