Classification of scrotal trauma based on mechanism of injury
Blunt trauma is the most common mechanism of injury (85%) usually happening with a direct blow to the testis with impingement against the symphysis pubis or ischial ramus.
The most important differential diagnosis is between injuries with rupture of the tunica albuginea,
requiring immediate surgical exploration,
and those in which the albuginea is intact,
usually managed conservatively.
- Penetrating scrotal trauma
Penetrating scrotal injuries occur less frequently as result of gunshot and other missile wounds or less commonly of knife violence,
self-mutilation or animal bites.
Nearly half of all these cases present with testicular rupture; therefore current American Urological Association (AUA) and European Association of Urology (EAU) guidelines strongly recommend immediate surgical exploration and imaging is not routinely required.
Classification of imaging modalities most commonly performed in scrotal trauma
While emergent surgical exploration is highly required in all cases of severe penetrating scrotal injury or hemodynamic instability,
in stable patient AUA and EAU guidelines recommend various imaging modalities according to the severity of clinical presentation and the mechanism of injury:
- Scrotal ultrasonography (US) is the first-line imaging method,
widely used in acute scrotum as a simple,
non-invasive and rapidly performing diagnostic tool,
allowing direct visualization of:
-testicular rupture;
-testicular fracture line;
-intra- or extratesticular hematoma;
-hydrocele and/or hematocele;
-incidental non-traumatic testicular masses.
- Color Doppler interrogation allows evaluation of:
-testicular perfusion
-post-traumatic testicular ischemic changes;
-post-traumatic testicular torsion;
-post-traumatic epididymitis.
- Contrast-enhanced US (CEUS) is performed when US is unclear to improve characterization of:
-continuity of tunica albuginea;
-testicular perfusion depicting partial or complete post-traumatic ischemia (valuable resource in acute scrotum injury of a vascular nature);
-intra-testicular fluid collection.
CEUS may also be valuable in patients with minor scrotal trauma,
which may appear normal on a standard US exam but will result hypoechoic and hypoperfused on CEUS.
- MR imaging (MRI) is an accurate diagnostic tool,
currently considered a second-line examination method usually performed when scrotal US is inconclusive,
providing:
-excellent contrast resolution;
-wider panoramicity;
-possibility to characterize blood products.
When surrounding edema or hematoceles do not allow visualization of tunica albuginea,
MRI may be employed for its multiplanar capabilities and better characterization of soft tissue,
detecting also minor tear of tunica albuginea missed on ultrasound.
- Computed tomography (CT) is not the imaging technique of choice for scrotal trauma because MRI and US have higher soft tissue contrast resolution and do not expose gonadal tissue to radiation.
However,
CT is routinely performed in polytrauma patients depicting:
-bone fractures;
-presence and location of bone fragments;
-testicular dislocation due to a blunt pelvic injury;
-concurrent post-traumatic injury of intra-abdominal organs;
-hemoperitoneum;
-active bleeding of scrotal hematoma on contrast-enhanced imaging.
Classification of the most common post-traumatic injuries
1. Testicular injuries
1.1 Testicular rupture
1.2 Post-traumatic testicular torsion
1.3 Testicular fracture
1.4 Testicular dislocation
1.5 Intratesticular hematoma
1.6 Incidental non-traumatic testicular masses
2. Extratesticular injuries
2.1 Post-traumatic epididymal injuries
2.2 Spermatic cord hematoma
2.3 Scrotal wall injuries
3. Hydrocele and hematocele
4. Post-traumatic vascular injuries
1.
Testicular injuries
1.1 Testicular rupture
This is the most severe scrotal injury characterized by traumatic disruption of the tunica albuginea and extrusion of testicular parenchyma into the scrotal sac.
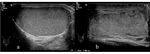
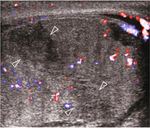
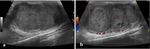
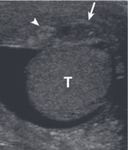
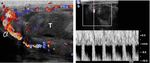
- US is the imaging modality of choice in identification of testicular rupture (Figure 1),
showing:
-contour irregularity of the testis, the most significant predictor for diagnosis of testicular rupture;
-disruption of tunica albuginea: normal tunica albuginea appears as a thin hyperechoic line outlining the testis.
Demonstration of its discontinuity supports a straightforward diagnosis of testicular disruption,
but it may be difficult to appreciate in presence of scrotal contusion;
-heterogeneous testicular echotexture,
with focal hyperechoic or hypoechoic regions corresponding to hemorrhagic or ischemic areas.
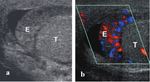
- Color Doppler interrogation is useful to determine viability of the injured testis.
Tunica albuginea rupture is almost always associated with disruption of tunica vasculosa and testicular rupture may result in ischemia at a portion of parenchyma of variable extention (Figure 2).
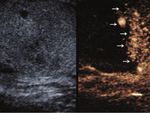
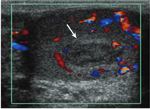
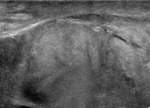
- CEUS is usually used when conventional US is unclear to confirm:
-the continuity of tunica albuginea,
allowing the detection of false negative cases of testicular rupture on US examination;
-partial or complete testicular ischemia resulting to be partilarly valuable in patients with minor scrotal (Figure 3).
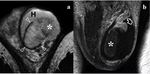
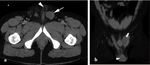
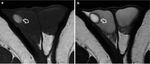
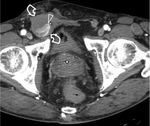
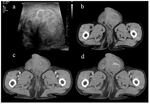
- MRI is a second-line examination method recommended for further evaluation when diagnosis of testicular rupture is equivocal at ultrasound:
-tunica albuginea when intact appears as a low signal intensity line on T2-weighted imaging; disruption of the this tunica appears as a distinct break on the dark signal intensity line on T2-weighted imaging (Figure 4a).
MRI also helps diagnose minor tears of the tunica albuginea otherwise missed on US;
-associated parenchymal necrosis and hemorrhage identified as areas of mixed intensity;
-ischemic changes identified after contrast medium administration (Figure 4b).
1.2 Post-traumatic testicular torsion
Scrotal trauma raises the risk of testicular torsion,
a surgical emergency frequently seen in children and young adults,
especially in presence of predisposing factors like a ‘‘bell clapper deformity’ (congenital condition where the posterior gubernaculum is not anchored and free to rotate within the tunica vaginalis).
Findings vary according to the duration and degree of rotation of the spermatic cord.
-early after torsion testis can appear normal at gray-scale ultrasound; absence of alterations at grey-scale US is indicative of salvageability of the testis;
-hypoechoic pattern may be seen when venous occlusion continues and edema develops;
-the twisted vessels of the spermatic cord may resemble a whirlpool or “snail shell”;
-once arterial occlusion occurs,
testicular tissue becomes heterogeneous and hyperechoic.
- Color Doppler interrogation shows markedly reduced or absent arterial and venous flows compared to the unaffected side (Figure 5).
1.3 Testicular fracture
In this injury,
the testicular parenchyma is broken by one or more fracture lines,
but the tunica albuginea is intact:
-fracture lines in the testis are often difficult to identify;
-when visible (Figure 6),
fractures appear as linear hypoechoic avascular bands extending across the testis;
-testicular shape and ultrasound appearance of tunica albuginea are normal.
- Color Doppler interrogation plays a significant role in guiding patient management,
because testicular fractures are treated conservatively if normal flow is identified,
while emergent surgery is recommended if flow is absent.
- MRI markedly improves visibility of:
-fracture lines;
-integrity of the tunica albuginea;
-associated hematomas,
hematoceles,
and lesion extension to the spermatic cord;
-parenchymal viability assessed after gadolinium contrast administration.
1.4 Testicular dislocation
Testicular dislocation is defined as the displacement of the testis outside its normal position in the scrotal sac; possible sites of dislocation include superficial (inguinal,
pubic,
penile,
preputial,
crural,
perineal or acetabular) and internal (canalicular or intra-abdominal) regions.
It is usually diagnosed on physical examination when empty scrotal sac is found or abnormally located testis is palpated.
When a clinical suspicion exists,
dislocation can be identified at US and MRI.
In the clinical practice,
however,
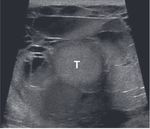
dislocated testis is more often identified incidentally during a CT scan performed for evaluation of abdominal organs in polytrauma patients (Figure 7).
1.5 Intratesticular hematoma
Intratesticular hematomas are common after scrotal traumas.
Small intratesticular hematomas without evidence of testicular rupture are treated conservatively,
while large hematomas may require surgical evacuation.
- US is the imaging modality of choice for detection and follow-up of intratesticular hematomas,
which present different sonographic charateristics with time (Figure 8):
-hyperacute and acute hematoma may appear hyperechoic or isoechoic to the surrounding testicular parenchyma or have a diffusely heterogeneous echotexture;
-chronic hematoma becomes hypoechoic and usually develops a cystic appearance over time.
- Color Doppler interrogation shows lack of intralesional flows,
allowing differential diagnosis with testicular tumors,
because most tumors display vascularization at color-doppler interrogation.
- MRI,
not routinely performed for testicular hematoma,
is indicated when findings at ultrasound are equivocal.
Characteristic signal changes are visible with time on T1- and T2-weighted images (Figure 9): methemoglobin within subacute blood is hyperintense on T1-weighted images,
while hemosiderin deposition produces a low-signal-intensity rim on T2-weighted images.
Lack of internal enhancement helps the differential diagnosis with hypovascular tumors.
- CT scan performed in polytrauma patients.
1.6 Incidental non-traumatic testicular masses
Testicular tumors may be detected in as much as 10–15% of patients with scrotal traumas,
more often incidentally,
but sometimes as palpable masses.
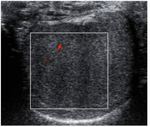
The most important differential diagnosis is between hematomas and incidental testicular tumors: although both tumors and intratesticular hematomas may have similar appearance at conventional ultrasound,
most tumors show vascularization at color Doppler,
while hematomas do not (Figure 10).
In one of our cases a testicular neoplasm,
resulted a seminoma on histologic examination,
was found incidentally during an ultrasound examination performed for a blunt scrotal trauma.
2.
Exratesticular injuries
Extratesticular injuries are more frequent than testicular lesions in case of scrotal traumas and generally require conservative management; the most common are epididymal injuries,
spermatic cord lesions,
fluid collections,
and scrotal wall injuries.
2.1 Post-traumatic epididymal injuries
2.1.1 Post-traumatic epididymitis is the most common trauma-related epididymal injury characterized by hyperemia and swelling of the epididymis:
- US: epididymis appears enlarged and presents heterogeneous echotexture with hypoechoic and hyperechoic areas usually due to small hematomas and contusions (Figure 11a).
- Color Doppler interrogation shows hyperemia of the epididymis (Figure 11b) with high velocity and low resistance flows.
Other less common post-traumatic epididymal injuries are:
2.1.2 Hematomas described as heterogeneous,
well-defined avascular masses; MRI is more sensitive than ultrasound in characterization of epidydimal hematoma.
2.1.3.
Rupture: in these cases epididymis presents ill-defined contours,
heterogeneous echotexture,
and absence of blood flow.
2.2 Spermatic cord hematoma
Although it typically occurs as a complication of hernia repair,
spermatic cord hematoma may also be associated with blunt scrotal trauma usually requiring conservative management
- US appearance is generally a non-specific heterogeneous,
well-defined,
avascular mass located superior to the testis (Figure 12);
- Doppler interrogation may depict associated rupture of the spermatic vessels and consequent testicular ischemia;
- MRI typically shows an avascular mass related to the spermatic cord which presents the characteristic behavior of blood products on the T1- and the T2-weighted images with high signal intensity (due to methemoglobin) on T1-weighted images and a low-signal-intensity rim (due to hemosiderin) on T2- and T2*-weighted images,
without appreciable enhancement.
- CT abdominal scan in polytrauma patients may incidentally detect spermatic cord hematomas showing eventual associated rupture of spermatic vessels with active bleeding after administraton of contrast medium (Figure 13).
2.3 Scrotal wall injuries
Blood extravasation within the scrotal wall may appear:
- US as a thickened,
inhomogeneous area,
or as a circumscribed fluid collection (Figure 14) which changes appearance with time;
- MRI as an avascular lesion in the scrotal wall with signal intensity characteristically changes with time on T1- and T2-weighted images.
3.
Hydrocele and hematocele
3.1 Reactive hydrocele and hematocele is often identified in patients with scrotal trauma.
3.2 Hematocele develops in case of blood extravasation in the potential space between the parietal and visceral layers of the tunica vaginalis and like hematomas presents different appearance with time:
- US: echogenic acutely,
hypoechoic and more complex later and chronically may develops septa,
loculations and fluid-fluid levels with sometimes calcifications (Figure 15).
- MRI: hematoceles display the characteristic signal changes with time already described for the other blood collections.
4.
Post-traumatic vascular injuries
4.1 Scrotal hematoma with active bleeding found in severe testicular rupture in which the high intratesticular pressure determine breaking of tunica vaginalis with bleeding in scrotum.
Although US and MRI are the imaging modalities of choice for detection of scrotal hematoma,
CT may represent an important auxiliary examination method especially in the suspicion of active bleeding within scrotal hematomas,
as in one of our case in which contrast-enhanced CT allowed direct visualization of contrast medium blush within a very large left scrotal hematoma associated with a severe testicular rupture (Figure 16).
Other much more rare post-traumatic vascular lesions,
intratesticular or extratesticular,
are:
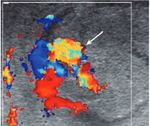
4.2 Pseudoaneurysm usually appears at ultrasound as an anechoic mass containing variably turbulent flow and the neck may be identified with flow entering the aneurysm during systole and exiting during diastole,
producing a characteristic "to-and-fro" pattern (Figure 17);
4.3 Arteriovenous fistula is identified at Doppler interrogation as a color blush displaying aliasing high velocity and turbulent flow (Figure 18).