Case 1
A 28-year-old woman with no past medical history presented to the emergency department with 10 days of headache accompanied with blurred vision.
Firstly,
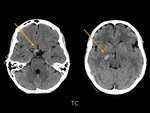
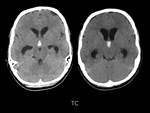
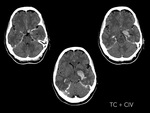
a non-contrast CT was performed,
revealing a hyperdense nodular lesion in the supraselar/chiasmatic region.
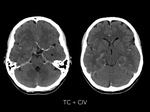
Secondly,
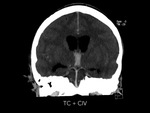
computed tomographic angiography did not show any vascular abnormality or enhancement.
The patient was transferred to neurosurgery service with a suspected supraselar tumor.
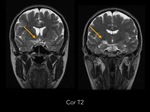
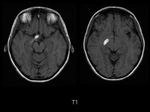
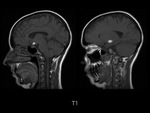
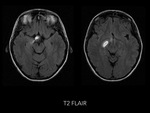
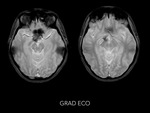
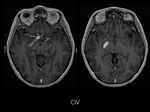
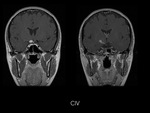
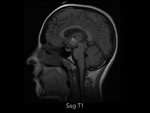
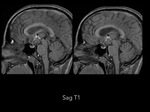
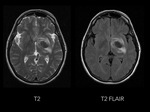
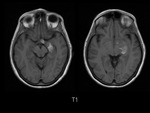
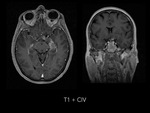
Magnetic resonance imaging (MRI) of the head demostrated a well-defined supraselar mass with involvement of the optic chiasm,
spreading along the right optic tract and perimesencephalic cistern.
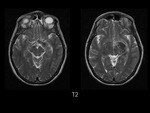
It was therefore hyperintense on T1 and T2-weighted images with surrounding hypodensity referred to as the halo sign,
everything associated with hemorrhagic lesion.
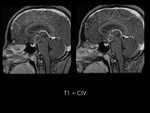
There was perilesional edema and no enhancement after contrast medium administration.
Frontotemporal craniotomy revealed a thickening of the right optic tract.
Pathological examination of a resected section of tumor confirmed cerebral pilocytic hemorrhagic astrocytoma.
Case 2
A previous healthy 18-year-old woman presented to the emergency department with 3 days of headaches,
nausea and vomiting.
Her headache was progresively worsening and associated with disorientation and drowsiness.
An urgent CT scan of brain revealed recent hemorrhage of the third ventricle with obstruction of both foramina Monro and hydrocephalus with transependymal oedema.
Computed tomographic angiography did not show any vascular abnormality or enhancement.
In addition, MRI of the head demostrated an heterogeneous hypothalamic/chiasmatic mass,
with cystic and solid components.
Intratumoral hemorrhage with bleeding in the third ventricle was observed.
The mass exhibited heterogeneous enhancement of the solid component and ring-like enhancement of surrounding lesion.
Right frontal craniotomy with interhemispheric transcallosal approach was performed and the mass and the haematoma were evacuated through the foramen of Monro.
Pathological examination confirmed cerebral pilocytic hemorrhagic astrocytoma.
Case 3
A 54-year-old woman with no past medical history presented to emergency department with progressive alteration in vision over the last 7 days.
Neurology department observed right homonymous hemianopsia.
An urgent CT scan of brain revealed a hyperdense mass lesion in chiasmatic/left optic tract region and extending to left thalamus with surrounding hypodensity suggesting oedema.
Computed tomographic angiography did not show any vascular abnormality or enhancement.
In addition,
MRI exploration found a suprasellar mass,
extending from the left optic tract to the lateral geniculate nucleus.
The lesion was hyperintense on T1-and hypointense on T2-weighted images and enhancement was not significant.
Left pterional craniotomy was performed and hematoma was evacuated.
Pathological examination of a resected section of tumor confirmed hemorrhagic pilocytic hemorrhagic astrocytoma of the hypothalamic/chiasmatic region.
Discussion
Pilocytic astrocytoma (PA) is a relatively well-defined astrocytoma,
classified as grade I by the World Health Organisation (WHO) and have a low growth rate.
Dissemination is uncommon,
seen in only 3-5% of newly diagnosed PAs.
The cerebellum,
optic nerve and chiasm and hypothalamic region are the most common locations,
although it can be found in cerebral hemisphere,
spinal cord or ventricles.
PA occurs most commonly in children and young adults.
Only 25% of astrocytomas are older than 18 years of age. The most common symptoms when PA is located in hypothalamic/chiasmatic region are the developmental delay and the ones related to mass effect.
It is rare to be associated with hemorrhages.
A review of the literature conducted until 2017 showed only 26 cases,
7 of them located in the hypothalamic and chiasmatic regions.
For the pathogenesis of hemorrhage in PA,
abnormal vasculature such as thin-walled ectatic blood vessels and degenerative vascular changes have been reported.
At MRI imaging,
PA is typically hypointense in T1-weighted pulse sequences and hyperintense in T2/Flair sequences.
The degree of surrounding edema is diminished in comparison with that seen in high-grade glial neoplasm.
However,
imaging findings are dependent on the type and severity of bleeding.
Findings could be similar to any spontaneous hemorrhage and identification of underlying pathology would be difficult in those cases.