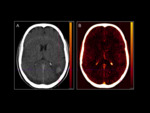
HYPERDENSIC LESIONS.
DIFFERENTIAL DIAGNOSIS
- LYMPHOMA
- HIGH GRADE ASTROCYTOMS
- CAVERNOMA
- METASTASIS
We will focus on the particular characteristics and,
above all,
on the differences of lymphoma,
cavernoma and metastasis,
with respect to the AAG.
- HIGH GRADE ASTROCYTOMS
Tumors of glial strain and poor prognosis,
with high growth rates in a short period of time.
In our experience we are dealing with grade III astrocytomas if they are biopsied soon,
and they usually show histological characteristics of glioblastoma multiforme (GBM) if the surgery is slightly delayed (few weeks from its initial detection).
We will focus on the appearance by CT and MRI of the lesions at their earliest stage.
The objective of the work is to show the characteristics that allow us to suggest the diagnosis in the first moments.
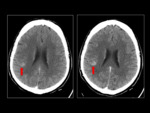
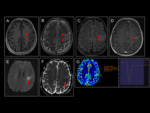
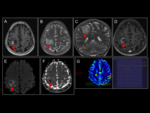
On CT,
the AAG appear as cortical or subcortical spontaneously hyperdense lesions,
with little mass effect,
little or no edema and a variable uptake that tends to oscillate between absent and light (Fig 4).
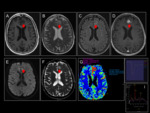
These facts offer a falsely non-aggressive aspect in the initial studies (Fig 1).
On MRI they behave as iso or hypointense lesions in T1 and slightly hyperintense in T2,
with little mass effect and little perilesional vasogenic edema (Fig 2).
They do not usually show significant hemorrhagic remains in T2* or susceptibility sequences.
After administration of gadolinium they have variable enhancement (Fig 3).
It is not uncommon for a lesion that apparently did not capture on CT to show enhancement on MRI.
We recall that they are spontaneously hyperdense on CT and,
therefore,
little uptake can go unnoticed.
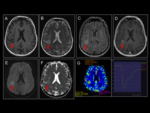
The behavior in diffusion (DWI) is variable,
but it is not unusual for them to condition moderate restraint,
with hyper-signal in DWI and low ADC values ​​(fig 5).
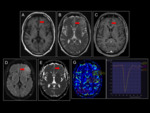
In MRI-perfusion study,
it is common to find high values ​​of rBVB indicative of high angiogenesis (Fig 6).
In MRI spectroscopy,
the choline / creatine ratio increased,
with NAA slightly decreased and lactate peaks present,
although not very high (Fig 9).
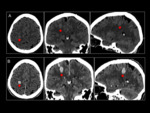
In patients in whom MRI was delayed,
a rapid growth of the lesion and transformation to GBM was evidenced.
We talked about delays that ranged from a few weeks to two months.
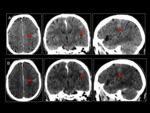
In these cases,
the behavior of the lesions is usually the usual,
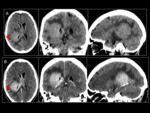
in the form of necrotic masses,
with hemorrhagic remnants,
peripheral uptake and abundant vasogenic edema.
It evolves quickly from a lesion of indolent morphology to a clearly aggressive tumor (Fig 7 y 8).
2.
PRIMARY CEREBRAL LYMPHOMA
Primary tumor of the CNS of lymphocyte lineage that occurs in immunocompetent and immunosuppressed patients,
assuming 2.5% of all brain tumors.
They are usually solitary lesions (60-70%) with mostly supratentorial location (60-80%).
Characteristically the lesions are grouped in the white matter around the ventricles,
often involving the corpus callosum and can also extend along ependymal surfaces.
Typically it has a spectacular response to treatment with corticosteroids,
a fact to be taken into account both in the diagnosis and in the biopsy planning studies.
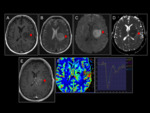
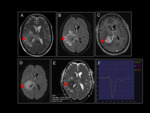
On CT,
they appear as spontaneously hyperdense lesions,
of small / medium size that,
unlike most incipient cortical gliomas,
enhance intensively after administration of intravenous contrast (Fig 10),
useful data in the differential diagnosis.
On MRI:
- well-demarcated lesion,
iso or hypointense on T1 and isointense on cortex on T2 and FLAIR
- it presents intense enhancement after the introduction of gadolinium and great restriction in the diffusion sequence with low values ​​in the ADC map (400-600 x 10-6 mm2 / s) due to its high cellularity
- low-moderate angiogenesis in MRI-perfusion,
unlike high-grade cortical astrocytomas,
GBM and metastases
- in the signal intensity curves after contrast administration,
the lymphoma curve exceeds the baseline (leakage T1),
a characteristic that differentiates it from GBM and metastasis (Fig 11)
- MR spectroscopy: Nonspecific tumor pattern with elevation of choline and lactate and decrease in NAA
- high restriction in ADC,
low signal Flair and T2,
low-moderate perfusion and the leakage pattern T1,
are the most useful data in the differentiation with AAG.
3.
CAVERNOMA
Vascular malformation formed by immature blood vessels closely juxtaposed without neural tissue containing blood at different stages of evolution.
They are congenital lesions that can change morphology over time or appear de novo.
They have a slow internal blood flow.
75% are solitary lesions and 40-60% have an epileptic crisis clinic.
25% are infratentorial and rarely extraaxial (leptomeningeal and cranial nerves).
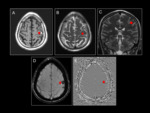
On CT of the skull without contrast,
they are visualized as rounded or ovoid hyperdense lesions with little or no uptake.
They can be calcified in 40-60% of cases (very useful in the differential diagnosis) and do not usually produce a mass effect unless the bleeding is recent.
The most common location is in the cerebral hemispheres,
followed by the brainstem and the cerebellum.
The appearance on MRI is characteristic and we could say pathognomonic in the majority of the occasions.
Nodular lesions with a heterogeneous central content due to the presence of hemoglobin in different stages of degradation and which usually have areas of high signal in T1 and T2 due to the presence of methaemoglobin.
The complete hypointense peripheral halo (hemosiderin) stands out in gradient echo sequence and susceptibility (Fig 12).
4.
ADENOCARCINOMA AND MELANOMA METASTASIS
Brain metastases of adenocarcinoma and melanoma,
unlike those of other primary tumors,
may spontaneously appear hyperdense on CT due to the content of mucin and melanin respectively (Fig 13).
Edema is variable,
although usually higher than in the initial phase AAG.
The uptake is usually greater than in the AAG and lower than in the lymphoma.
The knowledge of the known primary tumor will facilitate the diagnosis but present characteristics on MRI that can suggest it.
On MRI:
- melanoma metastases are hyperintense in T1 (due to the existence of melanin or hemorrhage) and hypointense in T2 and may show deposits of hemosiderin in the gradient echo sequence.
This behavior does not occur in the AAG
- a morphological characteristic of adenocarcinoma metastasis is the low signal in T2 and Flair (focal or global),
without susceptibility artifacts in T2* that justify it.
This signal is attributed to mucin and the fibrosa-desmoplastic reaction.
The uptake is usually not very prominent
- perfusion and spectroscopy can show identical behaviors to the AAG,
with high angiogenesis and tumor metabolites.
In this way,
the differential diagnosis is based on the T1,
T2,
T2* characteristics contrast.
The diffusion is not specific.