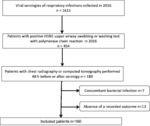
Our study population (Figure 3.) consisted of 160 patients,
including 80/160(50%) men and 80/160(50%) women,
with a median age of 43 years(IQR:32-56).
49/160(30.6%) patients had comorbidities,
12/160(7.5%) had DM, 29/160 (18.1%) had systemic hypertension,
4/160(2.5%) had COPD,
6/160(3.8%) had another pneumopathy and 8/160(5.0%) had immunosuppression. Five of 160(3.1%) patients were smokers.
None of the patients had asthma.
The vast majority of the included patients (147/160,91.8%) were diagnosed in March and April.
Concerning the clinical manifestations at admission,
144 patients had this information written in the medical records.
Based on this subpopulation,
141/144(97.9%) patients had flu-like symptoms,
25/144(17.4%) had dyspnea,
and 7/144 had thoracic pain.
None of the patients were septic or had hemoptysis.
On physical examination,
the median oxygen saturation was 96%(IQR:95-98),
the median HR was 92 bpm(IQR:80-107), 49/141(34.7%) patients had high temperature levels,
with a median temperature of 37ºC(IQR: 36.3-37.7),
the median systolic BP was 125.5mmHg(IQR: 113-138),
and the median diastolic BP was 78.5mmHg(IQR: 69-87).
Regarding the laboratory data,
the median white blood cell count and lymphocytes were 5990/mm³(IQR: 4610-7560) and 950/mm³(IQR: 680-1400),
respectively,
and the median of CRP was 1.90 mg/dL(IQR: 0.96-3.88).
Considering outcome,
37/160(23.1%) patients were hospitalized and classified as having a worse clinical outcome.
Four of these patients (4/37,
10.8%) required ICU admission,
and none of these patients died.
The mean age of this subpopulation was 50 years old (IQR: 34-66).
All patients who were hospitalized had an abnormality on CR and/or CT. Table 1 summarizes the patients’ characteristics and radiological findings.
113 patients underwent CR,
and 8/113(7.1%) of them were abnormal.
Pulmonary infiltrate was detected in 5/8(62.5%) patients,
consolidation was identified in 2/8(25.0%) patients and pleural effusion was found in 1/8(12.5%) patients.
60 patients underwent chest CT,
and 43/60(71.7%) patients showed some abnormality.
27/60(45.0%) patients had GGO,
9/60(15%) patients had consolidation,
26/60(43.3%) patients had bronchial thickening,
and 5/60 (8.3%) patients had pleural effusion.
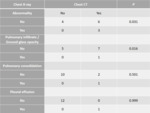
13 patients underwent both CR and chest CT (Table 2).
There was a significant correlation between an abnormal CR and abnormal chest CT (p=0.031) and between the presence of pulmonary infiltrate on CR and GGO on CT (p=0.016).
In contrast,
there was no significant correlation between consolidation and pleural effusion on CR and CT (p=0.501 and p=0.999, respectively).
Considering the clinical data,
the presence of DM,
systemic hypertension,
dyspnea, thoracic pain,
temperature levels and CRP levels were significantly different between the groups (Table 1).
The frequency of DM (7/37,18.9% vs 5/123,4,1%; p=0.003),
systemic hypertension (12/37,32.4% vs 17/106,13.8%; p=0.010),
dyspnea (12/25,32.4% vs 13/107,12.1%; p=0.005), and thoracic pain (5/37,
13.5% vs 2/107,
1.9%; p=0.005) were significantly higher in the patients who required hospitalization.
The temperature was significantly lower in the patients with worse clinical outcomes (36.4ºC vs 37.4ºC,
respectively,
p<0.001),
and the C-reactive protein levels were significantly higher (3.05 vs 1.75,
respectively,
p=0.026).
Regarding the imaging features on CR,
the presence of an abnormality,
pulmonary infiltrate,
consolidation,
and pleural effusion were significantly more frequent in the patients with worse outcomes ([4/14,28.6% vs 4/99,
4%;p=0.001],
[2/14,14.3% vs 1/99,1%;p=0.004], [2/14,14.3% vs 0/99,0.0%;p<0.001],
and [1/14,7.1% vs 0/99,0%;p=0.008],
respectively).
With regards to the imaging features on CT,
the presence of an abnormality,
GGO and consolidation were significantly more frequent in the patients with worse outcomes ([26/30,86.7% vs 17/30,56.7%;p=0.010],
[18/30,60% vs 9/30,30%;p=0.020],
and [8/30,26.7% vs 1/30,3.3%; p=0.011]).
Furthermore,
the distribution of the imaging features on CR and CT were correlated with outcome,
in which a diffuse pattern was more related to worse clinical outcomes.
In the logistic regression,
the following data predicted worse outcomes: DM (OR:8.3;95% CI 1.4-50.2,
p=0.020),
body temperature (OR: 0.4; 95% CI 0.3-0.8,
p=0.005),
thoracic pain (OR: 20.3; 95% CI 2.2- p<0.001),
alteration on CR or CT (OR: 22.7,
p<0.001),
pulmonary infiltrate on CR or GGO on CT (OR: 6.9,
p=0.002),
and pleural effusion on CT or CR (OR: 10.3, p=0.045).
Figures 1 and 2 show patients with and without worse clinical outcomes.
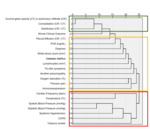
In the hierarchical cluster analysis,
three clusters were identified (Figure 4).
The cluster that better correlated with worse clinical outcomes contained the following variables: GGO on CT or CR,
consolidation on CT or pulmonary infiltrate on CR and the extension of the disease.